Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
ATHEROSCLEROSIS / RESEARCH PAPER
Investigation of IgG anti-oxLDL antibody levels and HDL and LDL subclasses in patients with ST-segment elevation acute myocardial infarction
1
Department of Laboratory Diagnostics, Public Health Institution „Health Center“, Bosnia and Herzegovina
2
University of Belgrade - Faculty of Pharmacy, Serbia
3
Clinical Hospital Center “Zemun”, Serbia
4
University of Belgrade - Faculty of Medicine, Serbia
5
Clinical Hospital Center “Bezanijska Kosa”, Serbia
6
Institute for Rehabilitation, Serbia
Submission date: 2020-12-11
Final revision date: 2021-03-30
Acceptance date: 2021-04-14
Online publication date: 2021-04-30
Corresponding author
Jelena Vekic
University of Belgrade - Faculty of Pharmacy, Vojvode Stepe 450, 11000, Belgrade, Serbia
University of Belgrade - Faculty of Pharmacy, Vojvode Stepe 450, 11000, Belgrade, Serbia
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Dyslipidemia, inflammation and immunological processes play a key role in the development of atherosclerosis. This study investigates the relationship of different phenotypes of low-density lipoprotein (LDL) and high-density lipoprotein (HDL), human antibodies G classes against oxLDL (IgG anti-oxLDL antibodies) and inflammatory marker pentraxin-3 (PTX3) in patients with ST-segment elevation acute myocardial infarction (STEMI). Among STEMI patients with different Synergy Between Percutaneous Coronary Intervention With Taxus and Cardiac Surgery (SYNTAX) score, we analyzed predictive abilities of these biomarkers to assess disease outcome.
Material and methods:
In 69 STEMI, 21 patients with stable angina pectoris (AP) and 67 healthy controls, IgG anti-oxLDL antibodies and PTX3 were determined by ELISA. Gradient gel electrophoresis was used for lipoprotein subclasses separation.
Results:
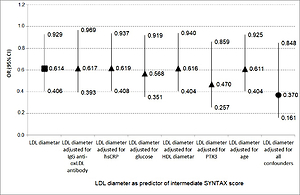
We found significantly lower HDL and LDL diameters (p<0.001 and p<0.001, respectively) and higher PTX3 concentration (p<0.001) in patients than in controls. Control subjects with small-sized HDL and LDL B phenotype had significantly higher IgG anti-oxLDL antibody levels (p=0.015), whereas STEMI patients with the same profile had higher PTX3 concentration (p=0.005). STEMI patients with intermediate SYNTAX score had lower levels of IgG anti-oxLDL antibodies (p=0.008). Multivariate logistic regression analysis showed that smaller LDL diameter was an independent predictor of intermediate SYNTAX score (OR=0.370; p=0.019).
Conclusions:
Smaller LDL and HDL particles are associated with elevated IgG anti-oxLDL antibodies in healthy subjects, but with increased PTX3 level in STEMI patients. In addition, we found that smaller LDL size was independent predictor of higher SYNTAX score. Further studies are needed to expand our preliminary observations.
Dyslipidemia, inflammation and immunological processes play a key role in the development of atherosclerosis. This study investigates the relationship of different phenotypes of low-density lipoprotein (LDL) and high-density lipoprotein (HDL), human antibodies G classes against oxLDL (IgG anti-oxLDL antibodies) and inflammatory marker pentraxin-3 (PTX3) in patients with ST-segment elevation acute myocardial infarction (STEMI). Among STEMI patients with different Synergy Between Percutaneous Coronary Intervention With Taxus and Cardiac Surgery (SYNTAX) score, we analyzed predictive abilities of these biomarkers to assess disease outcome.
Material and methods:
In 69 STEMI, 21 patients with stable angina pectoris (AP) and 67 healthy controls, IgG anti-oxLDL antibodies and PTX3 were determined by ELISA. Gradient gel electrophoresis was used for lipoprotein subclasses separation.
Results:
We found significantly lower HDL and LDL diameters (p<0.001 and p<0.001, respectively) and higher PTX3 concentration (p<0.001) in patients than in controls. Control subjects with small-sized HDL and LDL B phenotype had significantly higher IgG anti-oxLDL antibody levels (p=0.015), whereas STEMI patients with the same profile had higher PTX3 concentration (p=0.005). STEMI patients with intermediate SYNTAX score had lower levels of IgG anti-oxLDL antibodies (p=0.008). Multivariate logistic regression analysis showed that smaller LDL diameter was an independent predictor of intermediate SYNTAX score (OR=0.370; p=0.019).
Conclusions:
Smaller LDL and HDL particles are associated with elevated IgG anti-oxLDL antibodies in healthy subjects, but with increased PTX3 level in STEMI patients. In addition, we found that smaller LDL size was independent predictor of higher SYNTAX score. Further studies are needed to expand our preliminary observations.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.