Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
MEDICAL EDUCATION / PUBLIC HEALTH
The status quo of doctors’ occupational burnout and its correlation with the cognition of doctor-patient relationship tensity
1
Kaifeng Central Hospital, China
2
Department of Oncology, Nanjing Drum Tower Hospital, School of Chemistry and Chemical Engineering, Nanjing University, China
3
Henan Provincial People’s Hospital, People’s Hospital of Zhengzhou University, China
4
The Third People’s Hospital of Zhengzhou, China
5
NanYang Central Hospital, China
6
Henan No.3 Provincial People’s Hospital, China
Submission date: 2019-09-20
Final revision date: 2020-06-23
Acceptance date: 2020-07-05
Online publication date: 2021-04-15
Publication date: 2026-04-30
Corresponding author
Arch Med Sci 2026;22(2):655-662
KEYWORDS
TOPICS
ABSTRACT
Introduction:
The aims of the study were to understand the status quo of doctors’ occupational burnout and analyze the correlation between occupational burnout and cognition of tensity of the doctor-patient relationship (DPR).
Material and methods:
We took 265 doctors in a general hospital in China as respondents, conducted a survey of the degree of occupational burnout with the Maslach Burnout Inventory, scored the cognitive quantification of DPR tensity with Difficult Doctor-Patient Relationship Questionnaire-8, and analyzed the correlation between them. The cognitive quantitative scores of DPR tensity were also given to 782 inpatients and compared with the doctors’ cognitive scores.
Results:
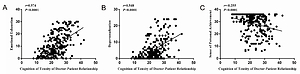
The degrees of occupational burnout in doctors, including three dimensions of emotional exhaustion, depersonalization and sense of personal achievement, were high. The proportions of moderate or more burnout were 50.9%, 53.2% and 48.7%, respectively. There was a statistically significant difference in occupational burnout among doctors of different ages and professional titles (p < 0.05). Doctors’ cognition of DPR tensity was significantly worse than patients’ cognition (p < 0.01). The degrees of emotional exhaustion and dehumanization were positively correlated with the poor cognition of DPR tensity in doctors (p < 0.001). The degree of sense of personal achievement was negatively correlated with the poor cognition in doctors (p < 0.001).
Conclusions:
Doctors’ age and professional title are important factors that affect the high degree of occupational burnout. Doctors do not have positive cognition of DPR tensity, which is different from that of patients. The degree of occupational burnout is closely related to the poor cognition of DPR tensity in doctors.
The aims of the study were to understand the status quo of doctors’ occupational burnout and analyze the correlation between occupational burnout and cognition of tensity of the doctor-patient relationship (DPR).
Material and methods:
We took 265 doctors in a general hospital in China as respondents, conducted a survey of the degree of occupational burnout with the Maslach Burnout Inventory, scored the cognitive quantification of DPR tensity with Difficult Doctor-Patient Relationship Questionnaire-8, and analyzed the correlation between them. The cognitive quantitative scores of DPR tensity were also given to 782 inpatients and compared with the doctors’ cognitive scores.
Results:
The degrees of occupational burnout in doctors, including three dimensions of emotional exhaustion, depersonalization and sense of personal achievement, were high. The proportions of moderate or more burnout were 50.9%, 53.2% and 48.7%, respectively. There was a statistically significant difference in occupational burnout among doctors of different ages and professional titles (p < 0.05). Doctors’ cognition of DPR tensity was significantly worse than patients’ cognition (p < 0.01). The degrees of emotional exhaustion and dehumanization were positively correlated with the poor cognition of DPR tensity in doctors (p < 0.001). The degree of sense of personal achievement was negatively correlated with the poor cognition in doctors (p < 0.001).
Conclusions:
Doctors’ age and professional title are important factors that affect the high degree of occupational burnout. Doctors do not have positive cognition of DPR tensity, which is different from that of patients. The degree of occupational burnout is closely related to the poor cognition of DPR tensity in doctors.
REFERENCES (35)
1.
Chinese Medical Doctor Association. White paper on the practice status of Chinese doctors. 2019. http://www.cmt.com.cn/detail/1....
2.
Makara-Studzińska M, Wontorczyk A, Izydorczyk B. Stress and occupational burnout in a population of Polish doctor – organizational-professional and non-professional-social predictors. Ann Agric Environ Med 2020; 27: 456-68.
3.
West CP, Dyrbye LN, Erwin PJ, Shanafelt TD. Interventions to prevent and reduce physician burnout: a systematic review and meta-analysis. Lancet 2016; 388: 2272-81.
4.
Dhingra M, Tewari R, Li M. Resilience training in medical school: the solution to doctor burnout? Med Teach 2016; 38: 319-20.
5.
Zhou X, Pu J, Zhong X, et al.; China Neurologist Association. Burnout, psychological morbidity, job stress, and job satisfaction in Chinese neurologists. Neurology 2017; 88: 1727-35.
6.
Sablik Z, Samborska-Sablik A, Drozdz J. Universality of physicians’ burnout syndrome as a result of experiencing difficulty in relationship with patients. Arch Med Sci 2013; 9: 398-403.
7.
Zheng X, Guo WQ, Chen Y, Su J. Investigation on occupational burnout among doctors in stomatology department in Hainan Province. J Kunming Med Univ 2016; 37: 131-4.
8.
Wu H, Liu L, Wang Y, Gao F, Zhao X, Wang L. Factors associated with burnout among Chinese hospital doctors: a cross-sectional study. BMC Public Health 2013; 13: 786-8.
9.
Hahn SR. Physical symptoms and physician-experienced difficulty in the physician-patient relationship. Ann Intern Med 2001; 134: 897-904.
10.
Wu H, Zhao X, Fritzsche K, et al. Quality of doctor-patient relationship in patients with high somatic symptom severity in China. Complement Ther Med 2015; 23: 23-31.
11.
Van der Feltz-Cornelis CM, Van Oppen P, Van Marwijk HW, De Beurs E, Van Dyck R. A patient-doctor relationship questionnaire (PDRQ-9) in primary care: development and psychometric evaluation. Gen Hosp Psychiatry 2004; 26: 115-20.
12.
Mingote Adán J, Moreno Jiménez B, Rodríguez Carvajal R, Gálvez Herrer M, Ruiz López P. Psychometric validation of the Spanish version of the Patient-Doctor Relationship Questionnaire (PDRQ). Actas Esp Psiquiatr 2009; 37: 94-100.
13.
Martín-Fernández J, del Cura-González MI, Gómez-Gascón T, Fernández-López E, Pajares-Carabajal G, Moreno-Jiménez B. Patient satisfaction with the patient-doctor relationship measured using the questionnaire (PDRQ-9). Aten Primaria 2010; 42: 196-203.
14.
Porcerelli JH, Murdoch W, Morris P, Fowler S. The Patient-Doctor Relationship Questionnaire (PDRQ-9) in primary care: a validity study. J Clin Psychol Med Settings 2014; 21: 291-6.
15.
Yang H, Wang HQ. Reliability and validity of Chinese version of doctor-patient relationship scale PDRQ-15. Chinese Med Ethics 2011; 24: 350-3.
16.
Yang H. Development and Evaluation of Chinese Version PDRQ/DDPRQ Scale: Quantitative Study of Doctor-patient Relationship. Datong: Shanxi Medical University; 2011.
18.
Mazur A, Czarkowska M, Goś A, Humeniuk E. Existential attitudes as predictors of burnout in Polish nurses employed in rural primary healthcare settings. Ann Agric Environ Med 2018; 25: 552-8.
19.
Dyrbye LN, Shanafelt TD. Physician burnout: a potential threat to successful health care reform. JAMA 2011; 305: 2009-10.
20.
Makara-Studzińska M, Załuski M, Tylec A, Panasiuk L. Do Polish doctors suffer from occupational burnout syndrome? An attempt to find an answer – Pilot study. Ann Agric Environ Med 2019; 26: 191-7.
21.
Kupcewicz E, Jóźwik M. Association of burnout syndrome and global self-esteem among Polish nurses. Arch Med Sci 2020; 16: 135-45.
22.
Leszczyński P, Panczyk M, Podgórski M, et al. Determinants of occupational burnout among employees of the Emergency Medical Services in Poland. Ann Agric Environ Med 2019; 26: 114-9.
23.
Mcmanus IC, Keeling A, Paice E. Stress, burnout and doctors’ attitudes to work are determined by personality and learning style: a twelve year longitudinal study of UK medical graduates. BMC Medicine 2004; 2: 29.
24.
Ogundipe OA, Olagunju AT, Lasebikan VO, Coker AO. Burnout among doctors in residency training in a tertiary hospital. Asian J Psychiatr 2014; 10: 27-32.
25.
Brewer EW, Sharpard L. Employee burnout: a meta-analysis of the relationship between age or years of experience. Human Resource Development Review 2004; 3: 102-23.
26.
Woodside JR, Miller MN, Floyd MR, McGowen KR, Pfortmiller DT. Observations on burnout in family medicine and psychiatry resident. Acad Psychiatry 2008; 32: 13-9.
27.
Shen WW, Bao Y. Cognitive differences between doctors and patients on doctor-patient relations. Chinese General Practice 2015; 18: 2329-32.
28.
Robinson G. Effective doctor patient communication: building bridges and bridging barriers. Can J Neurol Sci 2002; 29: 30-2.
29.
Ekstedt M, Söderström M, Åkerstedt T, Nilsson J, Søndergaard H-P, Aleksander P. Disturbed sleep and fatigue in occupational burnout. Scand J Work Environ Health 2006; 32: 121-31.
30.
Montgomery A, Panagopoulou E, Kehoe I, Valkanos E. Connecting organisational culture and quality of care in the hospital: is job burnout the missing link? J Health Organ Manag 2011; 25: 108-23.
31.
Shanafelt TD, Gradishar WJ, Kosty M, et al. Burnout and career satisfaction among US oncologists. J Clin Oncol 2014; 32: 678-86.
32.
Williams ES, Manwell LB, Konrad TR, Linzer M. The relationship of organizational culture, stress, satisfaction, and burnout with physician-reported error and suboptimal patient care: results from the MEMO study. Health Care Manage Rev 2007; 32: 203-12.
33.
Wen J, Cheng Y, Hu X, Yuan P, Hao T, Shi Y. Workload, burnout, and medical mistakes among physicians in China: a cross-sectional study. Biosci Trends 2016; 10: 27-33.
34.
Cohen D, Rhydderch M, Reading P, Williams S. Doctors’ health: obstacles and enablers to returning to work. Occup Med (Lond) 2015; 65: 459-65.
35.
Merrett A, Jones D, Sein K, Green T, Macleod U. Attitudes of newly qualified doctors towards a career in general practice: a qualitative focus group study. Br J Gen Pract 2017; 67: e253-9.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.