Introduction
Atrial fibrillation (AF) is the most common heart arrhythmia [1]. The condition is known to increase the risk of ischemic stroke (IS) and peripheral embolism [2]. According to epidemiological studies, more than 5.6 million people in the USA are expected to suffer from AF by 2050, while in the European Union, the number of people over 55 with AF is expected to increase to 17.9 million between 2010 and 2060 [3, 4]. Classical risk factors for the development of AF include hypertension, advanced age, diabetes mellitus, coronary heart disease, and lipid metabolism disorders [5–7]. Importantly, these are also recognized risk factors for ischemic stroke [8–10]. Researchers have observed that patients with recurring IS often show evidence of untreated AF [11]. Brambatti et al. argue that the relationship between AF and thromboembolic events is related to many more factors than just the duration of AF. Some thromboembolic events may be due to AF-induced stagnation, some may be caused by chronic endothelial changes due to many previous AF episodes, or may be the result of co-existence of mechanisms other than AF for which AF is only a risk marker, e.g. co-existence of hypertension [12]. Therefore, the purpose of this study was to investigate AF risk factors in patients with IS.
Material and methods
We retrospectively examined 2374 patients with acute IS. The study group consisted of 696 patients (446 women and 250 men) with acute IS and NVAF and the control group had 1678 patients (855 women and 823 men) with acute IS without AF. All patients were hospitalized at the Department of Neurology in Szczecin.
Diagnosis of AF was based on medical history or ECG examination on admission to the Neurology Department or during hospitalization. IS was defined as sudden onset of a focal neurological deficit lasting more than 24 h by means of brain computed tomography and/or magnetic resonance imaging. Congestive heart failure diagnosis was based on signs and symptoms of low cardiac output based on medical charts [13]. Diabetes mellitus was defined as a fasting blood glucose level greater than 126 mg/dl after a minimum of 2 tests or glucose level greater than 200 mg/dl any time during the day [14]. Dyslipidemia was defined as the combination of serum cholesterol concentration > 190 mg/dl, low-density lipoprotein (LDL) cholesterol > 115 mg/dl, serum triglyceride concentration > 150 mg/dl and high-density lipoprotein (HDL) cholesterol < 40 mg/dl in males and < 45 mg/dl in females [15]. Hypertension was diagnosed when the blood pressure (BP) was ≥ 140/90 mm Hg in repeated tests [16]. Coronary heart disease was determined by a previous history of myocardial infarction and angina pectoris. Smoker was defined as someone having smoked one or more cigarettes. Previous stroke was considered to be present if the medical charts included a stroke diagnosis. The CHA2DS2-VASc score (congestive heart failure/LV dysfunction (one point), hypertension (one point), age ≥ 75 years (two points), diabetes mellitus (one point), stroke (two points), vascular disease (one point), age 65–74 years (one point), (female) sex category (one point) is a scale used to assess the risk of thromboembolic complications in patients with AF. It is an improved CHADS2 score, augmented with additional risk factors of thromboembolic complications. The CHA2DS2-VASc score was determined for each patient participating in this study. The Pomeranian Medical University Ethics Committee approved the study protocol (KB-0012/46/02/19).
Statistical analysis
To compare the characteristics of NVAF stroke patients with stroke patients without AF, we used the Mann-Whitney test (quantitative data) and the Fisher exact test (qualitative data). In addition, univariable and multivariable logistic regression models were calculated for assessing the odds ratio of chosen risk factors of AF incidence among IS patients. Statistical significance was set at p < 0.05.
Results
Comparison of risk factors for atrial fibrillation in patients with ischemic stroke and nonvalvular atrial fibrillation and patients with ischemic stroke without atrial fibrillation
Cigarette smoking, hypertension, older age, diabetes mellitus, female gender, dyslipidemia, coronary heart disease, history of ischemic stroke, and higher CHA2DS2-VASc score were significantly more frequent in patients with IS and NVAF than in patients without AF (p < 0.01, p < 0.01, p < 0.01, p < 0.01, p < 0.01, p < 0.01, p < 0.01, p < 0.01, p < 0.01). A case comparison is presented in Table I.
Table I
Characteristics of patients with ischemic stroke. Patients with NVAF vs. patients without AF
Analysis of risk factors for AF in patients who suffered an ischemic stroke
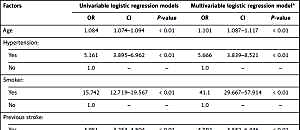
In this study we found – based on a univariable and multivariable logistic regression model – that compared to the patients with IS without AF, the group of patients who suffered from IS with NVAF had a higher proportion of patients who smoked cigarettes (OR = 15.742, p < 0.01; OR = 41.1, p < 0.01), had hypertension (OR = 5.161, p < 0.01; OR = 5.666, p < 0.01), history of a previous stroke (OR = 3.951, p < 0.01; OR = 4.792, p < 0.01), dyslipidemia (OR = 2.312, p < 0.01; OR = 1.592, p < 0.01), coronary heart disease (OR = 2.306, p < 0.01; OR = 1.988, p < 0.01), a greater proportion of female patients (OR = 1.717, p < 0.01; OR = 2.095, p < 0.01), higher incidence of diabetes mellitus (OR = 1.341, p < 0.01; OR = 1.261, p = 0.106) and more patients in old age (OR = 1.084, p < 0.01; OR = 1.101, p < 0.01) (Table II).
Table II
Analysis of risk factors for atrial fibrillation in patients with non-valvular atrial fibrillation who suffered a stroke compared to patients without AF (multivariate logistic regression)
| Factors | Univariable logistic regression models | Multivariable logistic regression model* | ||||
|---|---|---|---|---|---|---|
| OR | CI | P-value | OR | CI | P-value | |
| Age | 1.084 | 1.074–1.094 | < 0.01 | 1.101 | 1.087–1.117 | < 0.01 |
| Hypertension: | ||||||
| Yes | 5.161 | 3.895–6.962 | < 0.01 | 5.666 | 3.839–8.521 | < 0.01 |
| No | 1.0 | – | – | 1.0 | – | – |
| Smoker: | ||||||
| Yes | 15.742 | 12.719–19.567 | < 0.01 | 41.1 | 29.667–57.914 | < 0.01 |
| No | 1.0 | – | – | 1.0 | – | – |
| Previous stroke: | ||||||
| Yes | 3.951 | 3.253–4.804 | < 0.01 | 4.792 | 3.582–6.446 | < 0.01 |
| No | 1.0 | – | – | 1.0 | – | – |
| Dyslipidemia: | ||||||
| Yes | 2.312 | 1.93–2.772 | < 0.01 | 1.592 | 1.217–2.084 | < 0.01 |
| No | 1.0 | – | – | 1.0 | – | – |
| Congestive heart failure: | ||||||
| Yes | 0.862 | 0.664–1.111 | 0.257 | 0.758 | 0.454–1.252 | 0.284 |
| No | 1.0 | – | – | 1.0 | – | – |
| Sex: | ||||||
| Females | 1.717 | 1.433–2.062 | < 0.01 | 2.095 | 1.574–2.803 | < 0.01 |
| Males | 1.0 | – | 1.0 | – | – | |
| Diabetes mellitus: | ||||||
| Yes | 1.341 | 1.114–1.614 | < 0.01 | 1.261 | 0.952–1.671 | 0.106 |
| No | 1.0 | – | – | 1.0 | – | – |
| Coronary heart disease: | ||||||
| Yes | 2.306 | 1.924–2.767 | < 0.01 | 1.988 | 1.511–2.623 | < 0.01 |
| No | 1.0 | – | – | 1.0 | – | – |
* Full adjusted model; Independent variables: age; hypertension (yes/no); smoker (yes/no); previous stroke (yes/no); dyslipidemia (yes/no); congestive heart failure (yes/no); sex (F/M); diabetes mellitus (yes/no); coronary heart disease (yes/no). Group A (Status = 1) – NVAF. Group B (Status = 0) – No NVAF.
Discussion
According to our analysis, stroke patients with concurrent AF were significantly older (p < 0.01), more frequently female (p < 0.01), and significantly more frequently (p < 0.01) had type 2 diabetes, dyslipidemia, arterial hypertension, coronary heart disease, smoked tobacco products, and had a history of additional prior ischemic stroke, compared to stroke patients without AF. Patients with AF significantly more frequently manifested features which, according to our study, are not only independent risk factors for stroke, but most likely also increase risk of AF. Based on uni- and multivariable regression, the risk of atrial fibrillation among ischemic stroke patients is particularly high in patients with hypertension, stroke history, dyslipidemia, coronary heart disease, type 2 diabetes, older patients, smokers, and women.
Smoking is a well-known risk factor for cardiovascular diseases [17]. Nicotine stimulates a significant release of catecholamines into the serum, thus increasing the risk of cardiac arrhythmias. A study by Goette et al. concluded that exposure of healthy atrial tissues to nicotine caused a 10-fold increase in collagen III at the mRNA level, comparable to that observed in smokers [18]. The resulting atrial fibrosis is a central mechanism in the development of AF.
Arterial hypertension related to dysfunction of the renin-angiotensin-aldosterone system is associated with left ventricular hypertrophy, impaired left ventricular diastolic filling, increased left atrial pressure, atrial fibrosis, increased atrial ectopic activity, and a reduced rate of electrical conduction in and between atria [19]. Epidemiological studies show that arterial hypertension is associated with a 1.8 times higher risk of AF and a 1.5 times higher risk of AF progression, compared to chronic unchanging AF [7, 20]. Although as yet no randomized studies have conclusively shown that hypotensive therapy reduces the risk of AF, studies do suggest that effective hypertension treatment, especially renin-angiotensin-aldosterone antagonists, may reduce the likelihood of developing AF [21].
Coronary heart disease is both a risk factor for the development of AF and a disease whose progress is modulated by AF. The presence of coronary heart disease in patients with previously diagnosed atrial fibrillation has been associated with recurrent episodes of AF and a substantially increased risk of mortality [22].
The risk of AF increases with age, and the condition is much less common in people under 50 years of age. After the sixth decade of life, the incidence of AF increases significantly, from 0.5% in people aged over 50 to almost 9% in the eighth decade of life [4, 23]. It is not surprising, therefore, that among our patients, age is not only a risk factor for stroke, but also for AF. The incidence of AF in all age groups is higher in men. However, our study found that the incidence of atrial fibrillation was higher among women. Females with AF have a higher stroke risk than males with AF [24]. This could be a reason for the higher incidence of AF in this study of stoke patients.
Diabetes mellitus is one of the leading chronic diseases in patients with AF. For many years, diabetes mellitus was not taken as a risk factor for developing AF. The view on DM and AF changed in the last decade of the previous century. As shown in the Framingham study, diabetes is an independent risk factor for atrial fibrillation with an OR of 1.6 for women and 1.4 for men. Carbohydrate metabolism disorders have a direct damaging effect on the myocardium, promoting the development of AF [7].
Dyslipidemia is a major risk factor for cardiovascular disease. The association between dyslipidemia and AF, however, has been controversial. One study showed that hypercholesterolemia was more frequent in the non-AF group than in the AF group [25]. In another study low serum levels of total cholesterol, triglyceride and high-density lipoprotein cholesterol (HDL-C) levels were found in patients with paroxysmal AF [26]. In another cross-sectional study low levels of HDL-C were associated with the development of AF in women. This study also found that women have a 28% higher risk of developing AF with every 10% decrease in HDL-C. There was no correlation between TG levels and AF [27]. There are some potential mechanisms by which dyslipidemia is associated with AF and our study also confirms this. Elevated LDL and decreased levels of HDL cholesterol are associated with reduced systolic and diastolic left ventricle function and the development of heart failure, which are risk factors for AF [28]. Inflammation and oxidative stress are strongly associated with dyslipidemia. Both of them elevate the susceptibility to AF [29, 30]. The results of the meta-analysis carried out by Wang et al. and including twenty randomized controlled trials showed that statin therapy is useful for the prevention of AF [31].
CHA2DS2-VASc score is a scale used to assess the risk of thromboembolic complications in patients with AF. It is an improved CHADS2 score, augmented with additional risk factors of thromboembolic complications. Its individual components not only predict the risk of stroke associated with AF, but are also associated with the development of AF. In several studies this score has been used to predict the presence of AF in patients with ischemic stroke, although the results were inconsistent [32, 33]. Liu et al. in their study observed that among all risk factors, including the CHA2DS2-VASc score, only age and circulatory insufficiency were independently related to the newly detected AF in patients with acute IS [34]. In our study, patients with IS and coexisting AF had significantly higher CHA2DS2-VASc scores. This finding is not surprising because the CHA2DS2-VASc score takes into account causal risk factors for AF, and in our study patients with IS and co-existing AF were characterized by significantly more frequent AF risk factors such as hypertension, older age, diabetes mellitus, female gender, coronary heart disease and history of ischemic stroke.
Our study had several limitations. This was a single-center retrospective study, with a limited number of stroke patients. We selected only the most common atrial fibrillation risk factors. The participants in our ‘IS with no NVAF’ group may have undiagnosed AF. Further prospective studies with a larger sample size are needed.
In conclusion, it is not surprising that ischemic stroke patients with non-valvular atrial fibrillation – which is considered to be the primary risk factor for a cerebral episode – also display other risk factors. It should be emphasized, however, that in the examined group of patients, the most important stroke risk factors were significantly more closely associated with the concurrent AF. This was especially true for smoking, hypertension, dyslipidemia, coronary heart disease, and diabetes mellitus. Therefore, it should be assumed that these may be independent risk factors not only for stroke, but also for AF. This interpretation is particularly salient from a neurological point of view. The role of AF as an important risk factor for ischemic stroke remains underestimated, possibly due to the difficulty of detecting AF in its paroxysmal presentation. Therefore, it is necessary to perform long-term monitoring of cardiac function (e.g. Holter) to detect this arrhythmia.
Our study demonstrates a need for thorough and systematic monitoring of post-ischemic stroke patients in whom AF has not been detected and who display other important risk factors. Regardless of the stroke, these factors may be responsible for development of AF, and therefore it should be assumed that these patients have yet undiagnosed but already existent paroxysmal AF, or that their risk of developing AF is particularly high. This is important due to the resulting need to prescribe anticoagulants for the prevention of subsequent cerebral vascular episodes, as opposed to the standard antiaggregant drugs used for the prevention of ischemic stroke in the majority of cases.