Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
CARDIOLOGY / CLINICAL RESEARCH
Comparison of clinical characteristics, treatment, in-hospital and 12-month outcomes in patients after myocardial infarction with ejection
fraction < 40% with or without atrial fibrillation
1
3rd Department of Cardiology, SMDZ in Zabrze, Medical University of Silesia, Katowice, Silesian Center for Heart Diseases in Zabrze, Poland
2
Collegium Medicum, Kardynał Stefan Wyszynski Univeristy in Warsaw, Poland
3
National Institute of Cardiology in Warsaw, Poland
4
Department of Cardiology and Structural Heart Diseases, Medical University
of Silesia in Katowice, Poland
5
Department of Cardiology, University Hospital, Institute of Medical Sciences, University of Opole, Poland
6
Clinical Department of Cardiology, Department of Cardiology, Congenital Heart Disease and Electrotherapy, Silesian Center for Heart Diseases, Zabrze, Poland
Submission date: 2020-05-27
Final revision date: 2020-07-19
Acceptance date: 2020-07-22
Online publication date: 2020-10-26
Publication date: 2026-04-30
Corresponding author
Przemysław Trzeciak
3rd Department of Cardiology SMDZ in Zabrze Medical University of Silesia Katowice Silesian Center for Heart Diseases in Zabrze Poland
3rd Department of Cardiology SMDZ in Zabrze Medical University of Silesia Katowice Silesian Center for Heart Diseases in Zabrze Poland
Arch Med Sci 2026;22(2):750-759
KEYWORDS
TOPICS
ABSTRACT
Introduction:
The study aimed to compare the characteristics, treatment, and 12-month outcomes of patients after myocardial infarction (MI) and with left ventricular ejection fraction (LVEF) < 40%, with or without atrial fibrillation (AF).
Material and methods:
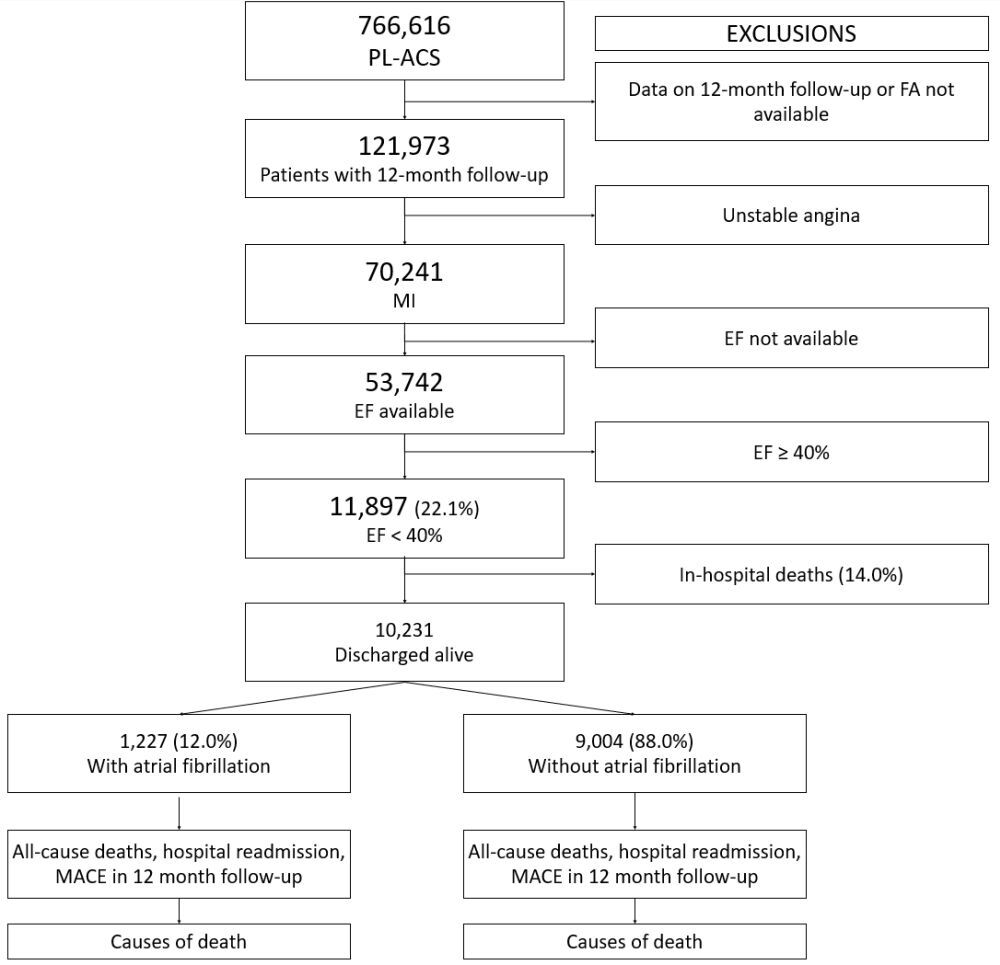
The analysis involved 10,222 surviving patients who were enrolled in the ongoing, prospective Polish Registry of Acute Coronary Syndromes (PL-ACS). The major adverse cardiac events (MACE) involved death, non-fatal MI, rehospitalization due to heart failure (HF), and stroke within 12 months after MI.
Results:
Patients with AF were older (73.7 [13.1] vs. 68.3 [16.4], p < 0.001) and had a greater prevalence of previous MI (37.3% vs. 32.4%, p = 0.0007), percutaneous coronary intervention (PCI) (27.5% vs. 23.6%, p = 0.002), and HF hospitalization (34.6% vs. 19.7%, p < 0.001). In patients with AF, coronary angiography (87.3% vs. 92.5%, p < 0.001) and PCI (76.8% vs. 82.7%, p < 0.001) were performed less frequently. Patients with AF had a higher rate of all-cause mortality (26.8% vs. 17.4%, p < 0.001), HF hospitalization (35.0% vs. 25.3%, p < 0.001), stroke (5.5% vs. 2.1%, p < 0.001) and MACE (56.2% vs. 42.8%, p < 0.001). In the multivariate analysis, AF was revealed to be associated with a higher all-cause mortality (odds ratio 1.20, 95% confidence interval 1.03–1.40, p = 0.018).
Conclusions:
Patients after MI with LVEF < 40% and with AF, compared to those without AF, had worse clinical characteristics, were less frequently subjected to coronary angiography and PCI during hospitalization, and had significantly less favorable 12-month outcomes.
The study aimed to compare the characteristics, treatment, and 12-month outcomes of patients after myocardial infarction (MI) and with left ventricular ejection fraction (LVEF) < 40%, with or without atrial fibrillation (AF).
Material and methods:
The analysis involved 10,222 surviving patients who were enrolled in the ongoing, prospective Polish Registry of Acute Coronary Syndromes (PL-ACS). The major adverse cardiac events (MACE) involved death, non-fatal MI, rehospitalization due to heart failure (HF), and stroke within 12 months after MI.
Results:
Patients with AF were older (73.7 [13.1] vs. 68.3 [16.4], p < 0.001) and had a greater prevalence of previous MI (37.3% vs. 32.4%, p = 0.0007), percutaneous coronary intervention (PCI) (27.5% vs. 23.6%, p = 0.002), and HF hospitalization (34.6% vs. 19.7%, p < 0.001). In patients with AF, coronary angiography (87.3% vs. 92.5%, p < 0.001) and PCI (76.8% vs. 82.7%, p < 0.001) were performed less frequently. Patients with AF had a higher rate of all-cause mortality (26.8% vs. 17.4%, p < 0.001), HF hospitalization (35.0% vs. 25.3%, p < 0.001), stroke (5.5% vs. 2.1%, p < 0.001) and MACE (56.2% vs. 42.8%, p < 0.001). In the multivariate analysis, AF was revealed to be associated with a higher all-cause mortality (odds ratio 1.20, 95% confidence interval 1.03–1.40, p = 0.018).
Conclusions:
Patients after MI with LVEF < 40% and with AF, compared to those without AF, had worse clinical characteristics, were less frequently subjected to coronary angiography and PCI during hospitalization, and had significantly less favorable 12-month outcomes.
REFERENCES (30)
1.
Lauritsen J, Gustafsson F, Abdulla J. Characteristics and long-term prognosis of patients with heart failure and mid-range ejection fraction compared with reduced and preserved ejection fraction: a systematic review and meta-analysis. ESC Heart Fail 2018; 5: 685-94.
2.
Ibánez B, James S, Agewall S, et al. ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Rev Esp Cardiol 2017; 70: 1082.
3.
Ponikowski P, Voors AA, Anker SD, et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 2016; 37: 2129-200.
4.
Batra G, Svennblad B, Held C, et al. All types of atrial fibrillation in the setting of myocardial infarction are associated with impaired outcome. Heart 2016; 102: 926-33.
5.
Podolecki, T, Lenarczyk R, Kowalczyk J, et al. Significance of atrial fibrillation complicating ST-segment elevation myocardial infarction. Am J Cardiol 2017; 120: 517-21.
6.
Schmitt J, Duray G, Gersh BJ, et al. Atrial fibrillation in acute myocardial infarction: a systematic review of the incidence, clinical features and prognostic implications. Eur Heart J 2009; 30: 1038-45.
7.
Jons C, Jacobsen UG, Joergensen RM, et al. The incidence and prognostic significance of new-onset atrial fibrillation in patiens with acute myocardial infarction and left ventricular systolic dysfunction: a CARISMA substudy. Heart Rhythm 2011; 8: 342-8.
8.
Lehto M, Snapinn S, Dickstein K, Swedberg K, Nieminen MS. Prognostic risk of atrial fibrillation in acute myocardial infraction complicated by left ventricular dysfunction: the OPTIMAAL experience. Eur Heart J 2005; 26: 350-6.
9.
Moss AJ, Zareba W, Hall WJ, et al. Prophylactic implantation of a defibrillator in patients with myocardial infarction and reduced ejection fraction. N Engl J Med 2002; 346: 877-83.
10.
Wita K, Kułach A, Wita M, et al. Managed Care after Acute Myocardial Infarction (KOS-zawał) reduces major adverse cardiovascular events by 45% in 3-month follow-up – single-center results of Poland’s National Health Fund program of comprehensive post-myocardial infarction care. Arch Med Sci 2019; 16: 551-8.
11.
Poloński L, Gąsior M, Gierlotka M, et al.; Polish Registry of Acute Coronary Syndromes (PL-ACS). Characteristics, treatments and outcomes of patients with acute coronary syndromes in Poland. Kardiol Pol 2007; 65: 861-72.
12.
Gąsior M, Pres D, Wojakowski W, et al. Causes of hospitalization and prognosis in patients with cardiovascular diseases. Secular trends in the years 2006-2014 according to the SILesian CARDiovascular (SILCARD) database. Pol Arch Med Wewn 2016; 126: 754-62.
13.
Gierlotka M, Zdrojewski T, Wojtyniak B, et al. Incidence, treatment, in-hospital mortality and one-year outcomes of acute myocardial infarction in Poland in 2009-2012 – nationwide AMI-PL database. Kardiol Pol 2015; 73: 142-58.
14.
Thygesen K, Alpert JS, White HD, Joint ESC/ACCF/AHA/WHF Task Force for the redefinition of myocardial infarction. Universal definition of myocardial infarction. Joint ESC/ACCF/AHA/WHF task force for the redefinition of myocardial infarction. Eur Heart J 2007; 28: 2525-38.
15.
Bardy GH, Lee KL, Mark DB, et al. Amiodarone or an implantable cardioverter-defibrillator for congestive heart failure. N Engl J Med 2005; 352: 225-37.
16.
Goldenberg I, Moss AJ, McNitt S, et al. Time dependence of defibrillator benefit after coronary revascularization in the Multicenter Automatic Defibrillator Implantation Trial (MADIT)-II. J Am Coll Cardiol 2006; 47: 1811-7.
17.
Zareba W, Klein H, Cygankiewicz I, et al. Effectiveness of cardiac resynchronization therapy by QRS morphology in the Multicenter Automatic Defibrillator Implantation Trial-Cardiac Resynchronization Therapy (MADIT-CRT). Circulation 2011; 123: 1061-72.
18.
Piotrowski R, Zaborska B, Pilichowska-Paszkiet E, Sikora-Frąc M, Baran J, Kułakowski P. RIVAroxaban TWICE daily for lysis of thrombus in the left atrial appendage in patients with non-valvular atrial fibrillation: the RIVA- TWICE study. Arch Med Sci 2019; 16: 289-96.
19.
Kotlęga D, Gołąb-Janowska M, Meller A, et al. Beneficial effects of pre-stroke statins use in cardioembolic stroke patients with atrial fibrillation: a hospital-based retrospective analysis. Arch Med Sci 2019; 15: 385-92.
20.
Zafrir B, Lund LH, Laroche C, et al. Prognostic implications of atrial fibrillation in heart failure with reduced, mid-range, and preserved ejection fraction: a report from 14 964 patients in the European Society of Cardiology Heart Failure Long-Term Registry. Eur Heart J 2018; 39: 4277-84.
21.
Xu HX, Zhu YM, Hua Y, Huang YH, Lu Q. Association between atrial fibrillation and heart failure with different ejection fraction categories and its influence on outcomes. Acta Cardiol 2020; 75: 423-32.
22.
Sartipy U, Dahlström U, Fu M, Lund LH. Atrial fibrillation in heart failure with preserved, mid-range, and reduced ejection fraction. JACC Heart Fail 2017; 5: 565-74.
23.
Son MK, Park JJ, Lim NK, Kim WH, Choi DJ. Impact of atrial fibrillation in patients with heart failure and reduced, mid-range or preserved ejection fraction. Heart 2020; 106: 1160-8.
24.
Crespo-Leiro MG, Anker SD, Maggioni AP, et al. European Society of Cardiology Heart Failure Long-Term Registry (ESC-HF-LT): 1-year follow-up outcomes and differences across regions. Eur J Heart Fail 2016; 18: 613-25.
25.
Lee SE, Cho HJ, Lee HY, et al. A multicentre cohort study of acute heart failure syndromes in Korea: rationale, design, and interim observations of the Korean acute heart failure (KorAHF) registry. Eur J Heart Fail 2014; 16: 700-8.
26.
Lee SE, Lee HY, Cho HJ, et al. Clinical characteristics and outcome of acute heart failure in Korea: results from the Korean acute heart failure registry (KorAHF). Korean Circ J 2017; 47: 341-53.
27.
Stevenson WG, Stevenson LW, Middlekauff HR, et al. Improving survival for patients with atrial fibrillation and advanced heart failure. J Am Coll Cardiol 1996; 28: 1458-63.
28.
Maisel WH, Stevenson LW. Atrial fibrillation in heart failure: epidemiology, pathophysiology, and rationale for therapy. Am J Cardiol 2003; 91 (6A): 2D-8D.
29.
Santhanakrishnan R, Wang N, Larson MG, et al. Atrial fibrillation begets heart failure and vice versa: temporal associations and differences in preserved versus reduced ejection fraction. Circulation 2016; 133: 484-92.
30.
Olsson LG, Swedberg K, Ducharme A, et al. Atrial fibrillation and risk of clinical events in chronic heart failure with and without left ventricular systolic dysfunction: results from the Candesartan in Heart failure-Assessment of Reduction in Mortality and morbidity (CHARM) program. J Am Coll Cardiol 2006; 47: 1997-2004.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.