Introduction
Some modern types of lifestyle, including sedentary behaviour with overconsumption of caloric food rich in simple sugars, significantly contribute to metabolic and age-related diseases with preceding pathophysiological changes such as hyperglycaemia, obesity, hypertension, dyslipidaemia and a pro-inflammatory state associated with accumulation of adipose tissue [1]. The combination of these changes is called metabolic syndrome (MeS); clinical criteria for diagnosing it include criteria for insulin resistance, central obesity, elevated blood pressure and dyslipidaemia (Table I). MeS is diagnosed when three or more criteria are fulfilled. The criteria for MeS diagnosis of different international organizations are described in Table I.
Table I
MeS criteria. For MeS diagnosis 3 of the following criteria must be fulfilled (WHO criteria: insulin resistance criterion and 2 others). The individuals with the values above the most stringent threshold of measured criteria (bolded) were assumed to have the higher MeS burden (B-MeS) in this study
[i] BP – blood pressure, FG – fasting glucose, UAE – urinary albumin excretion, WC – waist circumference, W/H – waist-to-hip ratio, ATP-III – National Cholesterol Education Program (NCEP) Adult Treatment Panel III, Consensus – consensus between IDF-AHA/National Heart Lung and Blood Institute, IDF – International Diabetes Federation, WHO – World Health Organization.
MeS is associated with increased risk of developing diabetes mellitus type 2, atherosclerosis and myocardial infarction [2, 3]. According to the samples from the general population using definitions of the metabolic syndrome developed by the National Cholesterol Education Program (NCEP) and World Health Organization (WHO), MeS presents a 30–52% risk for the development of diabetes mellitus, 12–17% for cardiovascular disease and 6–7% risk for all-cause mortality [4, 5]. The prevalence of MeS of 24% in the U.S. adults, aged 20 to 70 years, reported in 2002 [6], was surpassed in many countries around the world by 2007, e.g. South Africa of 33.5%, Turkey 33.4%, Iran 33.7%, Venezuela 31.2% and urban Brazil 25.4% [7–9]. A high proportion of the population with MeS was also reported elsewhere: in parts of China (Shanghai 23%), urban south India 26%, and a part of Mexico 27% [7]. No industrialized part of the world is spared; the prevalence of MeS was 14% in Finnish adults of 24 to 39 years in 2007 [10]. The MeS prevalence increases with age, as for example 24% of U.S. adults had MeS in the group of 20–70 years and 40% of subjects over 60 years according to the data from 2004 [6]. Another study published in 2009 based on the data of the National Health and Nutrition Examination Survey (NHANES) 2003–2006 reported the overall prevalence of MeS in the US in adults over 20 years as 34%, with large differences between age groups: individuals of 40–59 years of age were about three times as likely as those of 20–39 years of age to meet the criteria for metabolic syndrome diagnosis [11]. Large gender-specific differences were seen in the oldest group; males of 60 years of age and over were more than four times and females six times as likely to be diagnosed with MeS, respectively.
Visceral (splanchnic) obesity has been established as an important factor in development of MeS [12, 13]. While genetic and environmental influences contribute to MeS development, the major risk factors are chronic caloric overnutrition, possibly with high fructose intake [12, 14], and physical inactivity [15, 16].
At the molecular level, elevated mitochondrial oxidative stress is frequently associated with MeS and may contribute to its development [1]. The superoxide radical, generated by mitochondria, is dismutated rapidly to hydrogen peroxide by manganese superoxide dismutase (MnSOD), which is present at high concentrations in the mitochondrial matrix [17]. The matrix hydrogen peroxide is degraded by glutathione peroxidase 1 (GPX1) and peroxiredoxin III [18], and diluted by its diffusion out of the mitochondrion. Catalase (CAT) is another enzyme that protects cells from reactive oxygen species (ROS) by removal of hydrogen peroxide. Single nucleotide polymorphisms (SNPs) in genes encoding the antioxidant enzymes may change the amounts or activity of these enzymes. The CAT rs1001179 polymorphism in the transcription factor binding site (c.-262 C>T) promotes transcription of the T allele to result in increased translation [19]; however, the relationship between the polymorphism and the enzyme activity is complex [20]. MnSOD rs4880 (p.Ala16Val) reduces activity of mitochondrial SOD [21]; GPX1 rs1050450 polymorphism (p.Pro198Leu) also results in a less active variant [22].
ROS also regulate expression of proteins involved in inflammation, immune response and cell death [23]. Chronic inflammation is common in obesity and contributes to insulin resistance and diabetes mellitus type 2 [24]. Pathogen- or damage-associated signals, such as ROS, also contribute to assembly and activation of NLRP3 inflammasomes [25]. When activated, these protein complexes activate caspase-1 that processes pro-interleukin-1β to interleukin-1β (IL-1β) thus initiating downstream inflammatory responses [24]. NLRP3 inflammasome activation is associated with insulin resistance, circulating immune markers, macrophage function and chronic inflammation. SNPs of inflammasome components, NLRP3 rs35829419 (p. Gln705Lys) and CARD8 rs2043211 (p. Cys10Ter), were both associated with proinflammatory phenotype [24, 26, 27]. NLRP3 Gln705Lys phenotype results in increased production of IL-1β [28], while the polymorphism causing a non-functional CARD8 protein leads to loss of inhibition of caspase-1; the truncated protein does not prevent NF-κB stimulation of the inflammatory response [29]. This CARD8 polymorphism had no effects on cytokine profiles in a cohort of healthy blood donors [26]. CARD8 rs2043211 T allele reduced the risk of ischemic stroke, but not of coronary artery disease [30].
As detection of signs and symptoms that belong to the clinical criteria for MeS is important because of the likelihood of developing the associated diseases, it is of great importance to identify early markers of increased risk of developing the MeS in healthy population of young adults of about 20 years. Such markers could be assessed during the periodic health check-ups to detect individuals at risk of developing MeS (with the MeS burden, B-MeS) [31] in order to start lifestyle modifications as early as possible. This would enable timely counselling/lifestyle modification advice to still healthy individuals for prevention or delay of clinical symptoms referred to as MeS and of MeS-associated diseases. We performed a pilot study to assess the indicators of early metabolic alterations in young healthy adults to identify individuals with a higher metabolic syndrome burden who may benefit from timely introduction of preventive lifestyle modifications.
Material and methods
First year students of the Nursing programme at the University of Ljubljana, Faculty of Health Sciences were invited to participate in the study. The participants had no formal or informal training on MeS development and the importance of lifestyle choices prior to participation in the study. All subjects were informed of the study aims and were included after signing a written informed consent form. The study was approved by the Slovenian Ethics Committee for Research in Medicine and was conducted in compliance with the Helsinki Declaration.
All participants agreed to be surveyed and to donate a peripheral blood sample for biochemical and genetic analyses. Anthropometric measurements and dietary and exercise habits were recorded on the day of recruitment. Height, weight, waist and hip circumferences, blood pressure and two-compartment body composition were measured and body mass index (BMI) was calculated. A single frequency bioelectrical impedance analysis (BIA) at 50 kHz by Omron HBF-511 was used to determine the two-compartment body composition; BIA was performed always in the afternoon at least 2 h after a meal. Amounts of visceral fat were calculated from BIA measurements by an inbuilt Omron algorithm (arbitrary scale 1–30).
The individuals who met at least one criterion for diagnosis of MeS were assumed to have higher MeS burden (B-MeS). For assignment, the most stringent criteria for metabolic syndrome diagnosis were used: the waist circumference larger than 85 and 94 cm for women and men, respectively, waist-to-hip ratio larger than 0.85 and 0.9 for women and men, respectively, BMI more than 30 kg/m2 and blood pressure above or equal to 130/85 mm Hg (Table I).
Lifestyle and socioeconomic status was inferred from the questionnaire that included questions on diet, exercise, education level and social status. The highest education level reached by any parent in the family was set as the parent’s education. Diet was assessed by a food frequency questionnaire (FFQ) section composed of 36 individual food items, in total 9 categories of beverages and alcoholic drinks and questions on consumption of pre-processed food, fast food and food supplements. The FFQ section was derived from the questionnaires used for Spanish (Alimentacion y Salud 2.0) [32, 33] and Brazilian populations [34] that were adapted to local foods and eating habits.
Leukocytes were isolated from blood, genomic DNA was extracted by the FlexiGene DNA Kit (QIAGEN, Hilden, Germany) and genotyped for inflammasome (NLRP3 rs35829419, CARD8 rs2043211) and antioxidant genes (CAT rs1001179, MnSOD rs4880 and GPX1 rs1050450) polymorphisms using fluorescence-based competitive allele-specific polymerase chain reaction (KASP assays, LGC group, Teddington, UK). Catalase activity was determined from plasma of 84 individuals by a Catalase assay kit (Cayman Chemical). C-reactive protein (CRP) was measured by CRP (Latex) HS assay (Roche Diagnostics).
Statistical analysis
The median was used to present the central tendency with the 25th to 75th percentile range as a measure of variability. The Χ2 test was used to assess Hardy-Weinberg equilibrium (HWE) and to compare proportions between groups. The Mann-Whitney test was used to assess significance between the groups of non-parametric variables (age). Logistic regression was used to assess statistical significance (p-value), odds ratio (OR) and 95% confidence interval (95% CI) between individuals who were assigned to a higher risk group for MeS development and controls. All significance tests were two-tailed and conducted at the 0.05 level of significance. Analyses were performed using R (R Core Team (2014)).
Results
Out of 103 young, healthy Caucasian individuals included in our study, 81% were women. The median age of the study group was 20 years (25–75%, range: 20–22 years). Anthropometric parameters and blood pressure are routinely measured at the periodic health evaluations of the Slovenian population; therefore, these parameters were used to estimate the higher MeS burden (B-MeS, Table I). Thirty-four (33%) individuals, 28 (82%) women and 6 men, above the cut-off values for one of these parameters, were assigned to the B-MeS group. Gender and age did not differ significantly between the B-MeS and other individuals, i.e. controls (p = 0.75, p = 0.07, respectively).
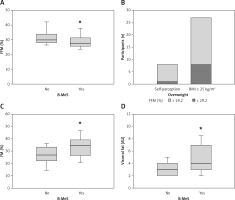
The percentage of fat free mass (FFM) of all participants measured by single frequency bioelectrical impedance analysis (BIA) was relatively homogeneous, with a median (25–75% range) of 29.3% (27.5–32.6%). Nevertheless, the participants in the B-MeS group had lower FFM, with a median of 27.7% (25.9–31.0%) compared to the control group with 30.0% (28.2–33.7%) (p = 0.012; OR = 0.88; 95% CI: 0.79–0.96) (Figure 1). The percentage of fat mass (FM) was more varied among all participants, with a median of 30% (22.9–35.3%). The B-MeS group had a significantly higher percentage of FM (p = 0.0006; OR = 1.11; 95% CI: 1.05–1.18), as the B-MeS group had median FM of 34.5% (26.9–38.7%), while the control group had 26.9% (22.5–32.8%). The median visceral fat was 4 arbitrary units (3–5), considered in the normal range by the manufacturer. The B-MeS group also had significantly higher visceral fat values, with a median of 4 (3.2–6.7) vs. 3 (2–4) in the group without an MeS burden (p = 0.0004; OR = 1.58; 95% CI: 1.25–2.09). Although 27 (26.2%) participants had a BMI equal to 25 or above, only 8 (7.7%) of them considered themselves overweight (Figure 1). Higher BMI values can be calculated also in individuals with high FFM; therefore the participants were divided further into two groups, according to the amount of the FFM, i.e. below or above the population’s median value of 29.2%. Out of 8 participants, 7 men and 1 woman, half of the men (4) and the woman were in the B-MeS group, but no man had the percentage of the FFM above the median calculated for the male population only. About one third of the participants (9) with the BMI equal to or above 25 had FFM above the median value. None of these participants had BMI greater than 30, an inclusion criterion for the B-MeS group.
Figure 1
Two-compartment body measurements in participants with and without metabolic syndrome burden (B-MeS). A, C – body composition measured by single frequency BIA. D – amounts of visceral fat. B – number of participants with self-perception of being overweight versus the number of participants with the BMI equal to or above 25 kg/m2. The amounts of FFM above and below the population’s median (29.2%) are indicated in light and dark grey, respectively
The thin line indicates the median value in box and whisker plots; *statistical significance. FFM – fat free mass, FM – fat mass, AU – arbitrary units, B-MeS – metabolic syndrome burden.
The median BMI of the B-MeS group was 25 kg/m2 (22–28.4 kg/m2) compared to 22 kg/m2 (19.8–23.4 kg/m2) in the rest of the participants (p < 0.0001; OR = 1.36, 95% CI: 1.18–1.61) (Figure 2). Nevertheless, 16 (47%) individuals in the B-MeS group were not overweight; i.e. their BMI was lower than 25 kg/m2. Seven out of 34 (20%) B-MeS participants, 5 women and 2 men, exceeded the MeS threshold for waist-to-hip ratio. The waist-to-hip ratio of the rest of the B-MeS participants who did not exceed the MeS threshold was also higher than that of the rest of the participants. There was a significant difference between the groups (p = 0.0003; OR = 8.17 × 105; 95% CI: 8.37 × 102–2.52 × 109), with a median of 0.78 (0.73–0.84) and 0.73 (0.70–0.77) in the participants with B-MeS and the others, respectively (Figure 2).
Figure 2
Anthropometric measurements in participants with and without the metabolic syndrome burden
The thin line indicates the median value; *statistical significance; BMI – body mass index, BP – blood pressure.
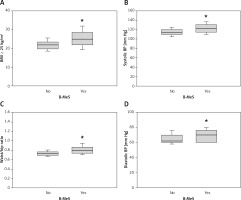
Half of the participants (17 out of 34) were assigned to the B-MeS group because of the blood pressure above or equal to 130/85 (15 systolic only, 2 diastolic only). The blood pressure in the B-MeS group was significantly higher (systolic blood pressure: p = 0.00004; OR = 1.14; 95% CI: 1.08–1.22; diastolic blood pressure: p = 0.01; OR = 1.07; 95% CI: 1.02–1.13).
Lifestyle factors had a considerable effect on the probability of B-MeS. The family background significantly influenced B-MeS risk, as the education level of participants’ parents correlated significantly with the risk for B-MeS status (p = 0.03; OR = 0.49; 95% CI: 0.24–0.89). Significantly more B-MeS individuals had parents with only primary or secondary school education (B-MeS group: 85.3%; other participants: 58%), while no individual assigned to the B-MeS group had a parent with a BSc or a higher degree (Figure 3).
Figure 3
Lifestyle indicators in participants with and without the metabolic syndrome burden
The thin line indicates the median value.
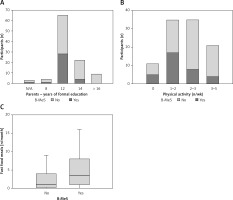
Exercise and diet also correlated with the probability of B-MeS (Figure 3). The individuals who were more active were less likely to be in the B-MeS group (p = 0.012; OR = 0.54; 95% CI: 0.33–0.86). Most of the individuals consumed fast food meals occasionally. The median number of fast food meals per month was 3 (range: 1–8) for the participants of the B-MeS group and 1 (range: 0.25–4) for the other participants. Therefore, the individuals in the B-MeS group seemed to consume more fast food meals per month, but this difference was not statistically significant. No other close association of increased B-MeS was found with a particular food item or beverage or their combinations.
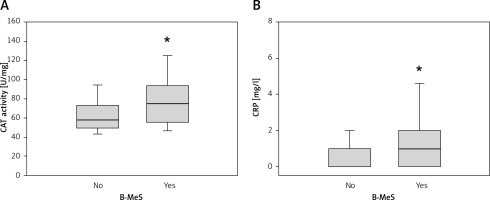
The distribution of CARD8, NALP3, CAT, GPX1 and SOD2 genotypes did not differ significantly between the B-MeS group and other participants (Table II). On the other hand, biochemical measurements correlated with B-MeS, although all participants had values still within the normal range. The individuals in the B-MeS group had statistically significantly higher enzyme activity of serum catalase (p = 0.024; OR = 1.02; 95% CI: 1.00–1.05) (Figure 4). Similarly, the CRP values of the individuals in the B-MeS group were significantly higher than in the rest of the participants (p = 0.05; OR = 1.26; 95% CI: 1.01–1.63).
Table II
Polymorphisms of genes encoding the NRLP3 inflammasome (CARD8, NALP3) and of antioxidant enzymes (CAT: catalase, GPX1: glutathione peroxidase 1, SOD2: superoxide dismutase 2)
Discussion
We have studied the indicators of early metabolic alterations in young healthy adults to identify the individuals with higher metabolic syndrome burden who may benefit from timely introduction of preventive lifestyle modifications. As the participants had no formal or informal training on development of MeS prior to the study, we consider the sample representative of the young adult student population. According to the Statistical Office of the Republic of Slovenia 47% of the young people between 19 and 24 years are students [35]. The sample thus may be representative for about half of the Slovenian young adult population.
There were about 4 times more female than male participants in our study. We detected no parameter that differed according to gender; therefore, we have presented the data together. Although there are some data that may lead to the conclusion that there are gender differences in MeS prevalence, Zimmet and co-authors discussed in detail the problems of comparing the prevalence data for MeS between the countries and even between studies in the same region, when using MeS syndrome criteria of different international bodies. From 14 studies using the ATPIII definition they concluded that neither sex appeared to have a clearly higher prevalence of the metabolic syndrome [36].
Assessment of anthropometric parameters, lifestyle indicators and laboratory tests has confirmed that the characteristics of the group assigned as B-MeS on the basis of fulfilment of a single diagnostic criterion for MeS were significantly different when compared to the rest of the study participants. The B-MeS group has significantly more FM, including visceral fat, higher waist-to-hip ratio, BMI and blood pressure and lower FFM. Similar findings were obtained in other studies. Upper-normal waist circumference was reported as a risk factor for metabolic syndrome in a study of over 173 000 normal-weight subjects [37]. Lapice et al. [38] found that among non-obese young people those with abdominal adiposity had an adverse cardiovascular risk factor profile. An association between abdominal obesity and higher risk of MeS was also reported in adolescents [31]. A correlation between waist-to-hip ratio and blood pressure was also reported in a sample of 140 children aged 6–16 [39].
In our study, each individual was placed in the B-MeS group on the basis of fulfilment of the single criterion (the most stringent) for MeS. Nevertheless, the participants in the B-MeS group had significantly higher median values for all other parameters tested, although still within the normal clinical range. Simple anthropometric measurements were found to suffice for early differentiation of metabolic differences. This agrees with the report that anthropometric measurements were good enough predictors of glycaemia and insulin resistance in the sense that other complex measurements such as MRI, DXA and CT contributed little to the prediction of MeS in Indian men [40].
Simple body measurements and body proportions are easily assessed; however, we found that only one third of individuals with BMI values that classify them as overweight considered themselves as overweight. The same metabolic alterations may be present in overweight as well as in some lean individuals. It is conceivable that the lean individuals do not notice that they are at risk for MeS, as they perceive their body shape as normal. Therefore, timely assessment by medical professionals is needed.
Lifestyle indicators, such as the amount of physical activity, socio-economic status of the family and diet, also differed between the groups. Our observation that the B-MeS group was less physically active is in agreement with findings of other authors [41–43]. Physical inactivity for only 14 days was reported to reduce the insulin sensitivity in young adult men [16].
Low levels of education of participants’ parents correlated with higher B-MeS. This correlation may also be due to the fact that we examined young adults, who have only recently moved away from their parents. Such an influence of socio-economic status was reported before. Socio-economic status was related to morbidity and mortality from diabetes mellitus in ten European countries [44]. It had an effect on the probability of developing MeS also in South Korea, where men with the lowest education level and women with the highest were significantly less likely to have metabolic syndrome [45].
The number of consumed fast food meals that was indicated by the participants tended to correlate with the B-MeS and is in agreement with a report on Iranian children and adolescents where the fast food intake was associated with the incidence of MeS, abdominal obesity, and hypertriglyceridaemia [46]. It is possible that we did not reach statistical significance because of the small number of participants in our study. The dietary fibre intake and carbohydrate quality and quantity were negatively associated with the all-cause and CVD mortality risks in more than 500 000 Europeans with confirmed diabetes mellitus [47]. We found no other association of B-MeS and a single or a combination of food ingredients, although such connections were reported from much larger populations, e.g. from more than 15 000 participants in the Brazilian study [48, 49].
We also assessed the role of genetic factors, but the genotype distribution of polymorphic genes coding for inflammasome or antioxidative enzymes did not differ between the B-MeS individuals and other participants. This may be due to the small study group. Polymorphism in the gene for the pro-inflammatory cytokine IL-6 (SNP rs1800795 G allele) was recently associated with increased odds for MeS in a 3-times larger Brazilian population [50]. Higher inflammation and oxidative stress are generally present in individuals with MeS; therefore, the higher levels in activity of an antioxidative enzyme, plasma catalase, that we observed in the participants of the B-MeS group seem consistent. This seems to agree with the results of Pennathur et al. [51] from 25 non-diabetic subjects with MeS where oxidative stress markers, including serum catalase, decreased after 24-week lifestyle intervention. However, higher catalase activity was not always detected. Although oxidative stress was detected in the MeS group, the levels of plasma catalase activity were not increased in the study, which included only 24 MeS and 18 matched controls [52].
Like the participants in our B-MeS group, the metabolic syndrome patients had persistently higher levels of CRP with no clinical symptoms of inflammatory diseases [53, 54]. Higher CRP was found to correlate with visceral obesity also in non-obese young people [38, 55]. In a randomized control trial in 52 women with MeS, CRP was lowered only in the group provided with the 6-month therapeutic lifestyle modification (health education and exercise) programme [56]. CRP values were found to oscillate with the menstrual cycle in women [57]. In our study, the CRP levels were higher also in the B-MeS group when only male participants were analysed.
Clinical signs of MeS develop over time, as is also seen in its lower prevalence in the younger compared to the older population groups [6, 11, 58]. Limitations of the current MeS definitions, which are dichotomous, necessitated development of continuous MeS scores that may better represent an aggregated burden for MeS especially in paediatric populations [31, 59, 60]. There is a tendency to simplify the algorithms for calculation of the continuous MeS score; however, this approach will always include calculations to evaluate the MeS burden. We observed here that individuals who fulfilled a single diagnostic MeS criterion had a phenotype significantly more similar to that of the MeS population compared to the rest of the study participants even among the young adults. Therefore, determination of B-MeS as shown here is potentially a practical crude screening method that can be applied at any GP practice. The proportion of the healthy population that fulfilled a single MeS criterion that will progress to the MeS diagnosis needs to be validated and is a limitation of this study.
In conclusion, as lifestyle modification is an efficient measure for the reversal of some MeS parameters [56], early detection of individuals at risk, especially young ones, should improve the health of the population. With the total number of adults with diabetes expected to rise to 6.4% of the world adult population by 2030 [61] and an estimated 93.6 million disability-adjusted life years related to metabolic problems due to overweight and obesity in 2010 [62], the early attenuation/reversal of metabolic modifications may considerably reduce the healthcare costs. Validation of this pilot study on larger cohorts is needed and assessment of different populations will enable the appropriate population threshold values to be established.