Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
AUTOIMMUNITY / RESEARCH PAPER
Epidemiology and risk factors for fractures among patients with autoimmune diseases: a nationwide population-based study
1
Department of Pediatrics, Taipei Veterans General Hospital, Taipei, Taiwan, Taiwan
2
Faculty of Medicine, School of Medicine, National Yang Ming Chiao Tung University, Taipei,
Taiwan, Taiwan
3
Division of Pediatric Surgery, Department of Surgery, Taipei Veterans General Hospital,
Taipei, Taiwan, Taiwan
4
Department of Medical Education, Taipei Veterans General Hospital, Taipei, Taiwan, Taiwan
5
Institute of Emergency and Critical Care Medicine, School of Medicine, National Yang Ming
Chiao Tung University, Taipei, Taiwan, Taiwan
Submission date: 2025-05-22
Final revision date: 2025-11-14
Acceptance date: 2026-02-11
Online publication date: 2026-05-01
Corresponding author
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Studies concerning the effects of biologic disease-modifying antirheumatic drugs (DMARDs) on fracture risk in patients with autoimmune diseases are limited. This study aimed to identify demographic, disease-specific, and treatment-related risk factors associated with clinical fractures.
Material and methods:
Individuals aged >18 years with a newly diagnosed autoimmune disease between 2003 and 2014 were identified from Taiwan’s National Health Insurance Research Database. Multivariate Cox proportional hazards regression was employed to identify risk factors associated with fractures.
Results:
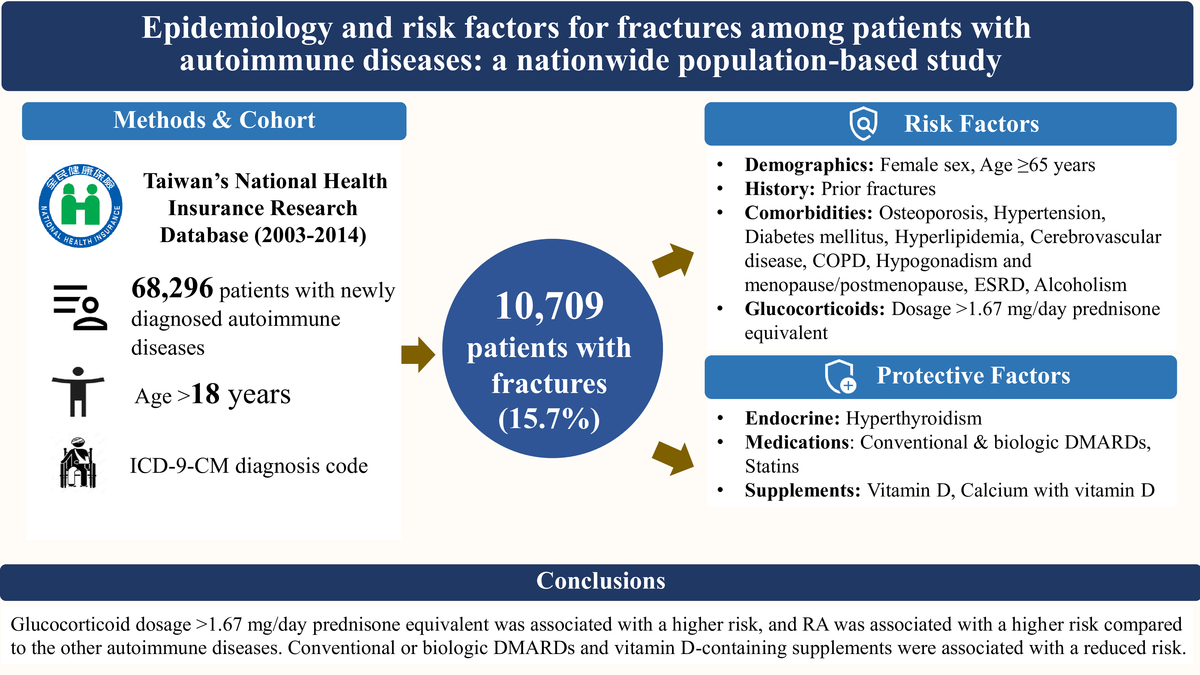
Among 68,296 patients (mean age 51.9±15.4 years; 78.4% female), rheumatoid arthritis was the most common autoimmune disease. During a mean follow-up of 5.6±3.5 years, 10,709 (15.7%) patients had fractures. Independent predictors included female sex, age ≥65 years, prior fractures, comorbidities (osteoporosis, hypertension, diabetes mellitus, hyperlipidemia, cerebrovascular disease, chronic obstructive pulmonary disease, hypogonadism and menopause/postmenopause, end-stage renal disease, alcoholism), and glucocorticoid use >1.67 mg/day prednisone equivalent. The fracture risk was lower in patients with systemic lupus erythematosus, systemic sclerosis, vasculitis, pemphigus, Sjögren’s syndrome, polymyositis/dermatomyositis and inflammatory bowel disease compared to those with rheumatoid arthritis. The use of conventional DMARDs, biologic DMARDs (TNF-α and IL-6 inhibitors and selective T-cell co-stimulatory modulator), and vitamin D–containing supplements was independently associated with a reduced fracture risk.
Conclusions:
Both general and disease-specific factors contributed to fracture risk. The lower fracture risk among patients treated with DMARDs and vitamin D highlights the benefits of controlling inflammation and optimizing bone health. These findings provide robust, large-scale epidemiologic evidence from a Taiwanese population and underscore the importance of minimizing glucocorticoid exposure.
Studies concerning the effects of biologic disease-modifying antirheumatic drugs (DMARDs) on fracture risk in patients with autoimmune diseases are limited. This study aimed to identify demographic, disease-specific, and treatment-related risk factors associated with clinical fractures.
Material and methods:
Individuals aged >18 years with a newly diagnosed autoimmune disease between 2003 and 2014 were identified from Taiwan’s National Health Insurance Research Database. Multivariate Cox proportional hazards regression was employed to identify risk factors associated with fractures.
Results:
Among 68,296 patients (mean age 51.9±15.4 years; 78.4% female), rheumatoid arthritis was the most common autoimmune disease. During a mean follow-up of 5.6±3.5 years, 10,709 (15.7%) patients had fractures. Independent predictors included female sex, age ≥65 years, prior fractures, comorbidities (osteoporosis, hypertension, diabetes mellitus, hyperlipidemia, cerebrovascular disease, chronic obstructive pulmonary disease, hypogonadism and menopause/postmenopause, end-stage renal disease, alcoholism), and glucocorticoid use >1.67 mg/day prednisone equivalent. The fracture risk was lower in patients with systemic lupus erythematosus, systemic sclerosis, vasculitis, pemphigus, Sjögren’s syndrome, polymyositis/dermatomyositis and inflammatory bowel disease compared to those with rheumatoid arthritis. The use of conventional DMARDs, biologic DMARDs (TNF-α and IL-6 inhibitors and selective T-cell co-stimulatory modulator), and vitamin D–containing supplements was independently associated with a reduced fracture risk.
Conclusions:
Both general and disease-specific factors contributed to fracture risk. The lower fracture risk among patients treated with DMARDs and vitamin D highlights the benefits of controlling inflammation and optimizing bone health. These findings provide robust, large-scale epidemiologic evidence from a Taiwanese population and underscore the importance of minimizing glucocorticoid exposure.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.