Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
EPIDEMIOLOGY / RESEARCH PAPER
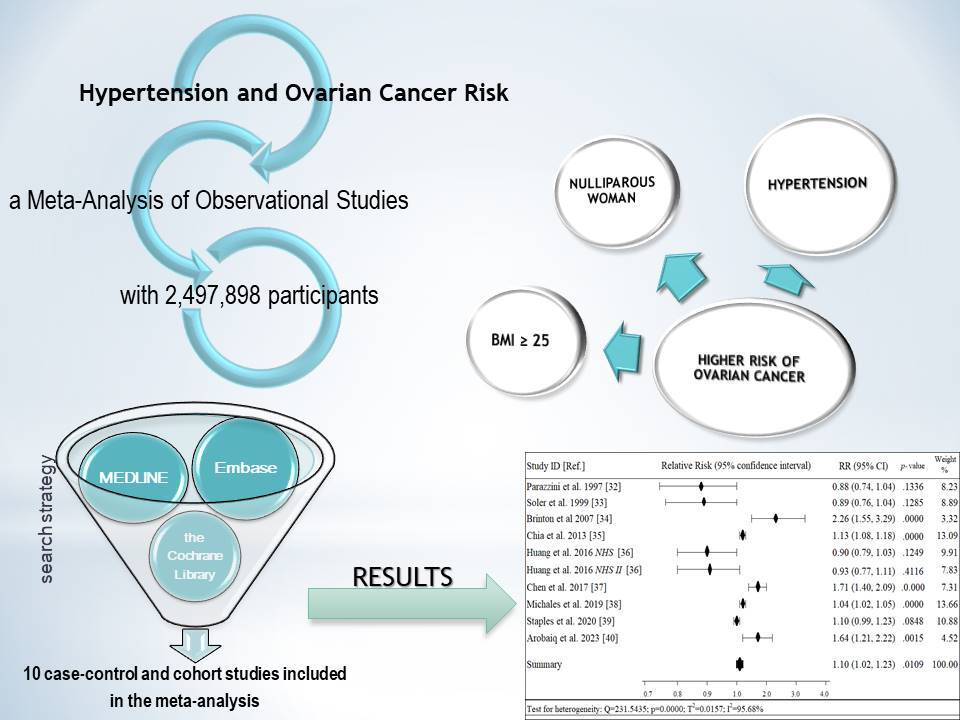
Hypertension and Ovarian Cancer Risk: a Meta-Analysis of Observational Studies
with 2,497,898 participants
1
Chair of Preclinical Science, Department of Medical Informatics and Statistics with e-Health Lab, Medical University of Lublin, Poland,, Poland
2
University Clinical Hospital No. 4 in Lublin, Poland, Poland
3
Gynecology Unit, Specialistic Medical Center Czechow, Lublin, Poland, Poland
4
University Clinical Hospital No. 1 in Lublin, Poland, Poland
5
School of Public Health, Centre of Postgraduate Medical Education of Warsaw, Warsaw, Poland, Poland
Submission date: 2025-03-11
Final revision date: 2025-08-22
Acceptance date: 2025-09-05
Online publication date: 2025-11-28
Publication date: 2026-04-12
Corresponding author
Agnieszka Drab
Chair of Preclinical Science, Department of Medical Informatics and Statistics with e-Health Lab, Medical University of Lublin, Poland,, Lublin, Poland
Chair of Preclinical Science, Department of Medical Informatics and Statistics with e-Health Lab, Medical University of Lublin, Poland,, Lublin, Poland
Arch Med Sci 2026;22(3)
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Ovarian cancer is the eighth most common cancer in women, and is an important source of cancer-related mortality, particularly in developed countries. Scientific studies show that hypertension may play a significant role in the initiation of cancer. Therefore, we carried out the first meta-analysis to comprehensively examine the association between hypertension and ovarian cancer risk.
Material and methods:
We performed a literature search of all of the observational studies published as original articles from inception to July 2024 and we searched the following databases: PubMed, EMBASE and Cochrane Library. Finally, we included ten full-text cohort and case-control studies addressing the effect of hypertension on ovarian cancer in this meta-analysis. The our study was preregistered with the PROSPERO:CRD42024565574 and followed the PRISMA statement. Effect size was presented as risk ratios(RRs). Heterogeneity test evaluation was performed using Cochran’s Q test and I2 statistics.
Results:
The meta-analysis included a total of 2,497,898 women. There was a statistically significant association (RR=1.10,1.02–1.23, p<0.011) between hypertension and ovarian cancer risk. Subgroup analysis showed that parity may significantly reduce the ovarian cancer risk, which was higher among woman who had never given birth (RR=1.43,p<0.002), while a body mass index >25 increased the risk of ovarian cancer (RR=1.12,p<0.001).
Conclusions:
Findings of this comprehensive review and meta-analysis indicate that hypertension is associated with higher overall risk of ovarian cancer. The data presented in our study are novel, but from a future perspective, we hope that this meta-analysis will encourage researchers to conduct further studies to assess the effect of hypertension on ovarian cancer.
Ovarian cancer is the eighth most common cancer in women, and is an important source of cancer-related mortality, particularly in developed countries. Scientific studies show that hypertension may play a significant role in the initiation of cancer. Therefore, we carried out the first meta-analysis to comprehensively examine the association between hypertension and ovarian cancer risk.
Material and methods:
We performed a literature search of all of the observational studies published as original articles from inception to July 2024 and we searched the following databases: PubMed, EMBASE and Cochrane Library. Finally, we included ten full-text cohort and case-control studies addressing the effect of hypertension on ovarian cancer in this meta-analysis. The our study was preregistered with the PROSPERO:CRD42024565574 and followed the PRISMA statement. Effect size was presented as risk ratios(RRs). Heterogeneity test evaluation was performed using Cochran’s Q test and I2 statistics.
Results:
The meta-analysis included a total of 2,497,898 women. There was a statistically significant association (RR=1.10,1.02–1.23, p<0.011) between hypertension and ovarian cancer risk. Subgroup analysis showed that parity may significantly reduce the ovarian cancer risk, which was higher among woman who had never given birth (RR=1.43,p<0.002), while a body mass index >25 increased the risk of ovarian cancer (RR=1.12,p<0.001).
Conclusions:
Findings of this comprehensive review and meta-analysis indicate that hypertension is associated with higher overall risk of ovarian cancer. The data presented in our study are novel, but from a future perspective, we hope that this meta-analysis will encourage researchers to conduct further studies to assess the effect of hypertension on ovarian cancer.
REFERENCES (82)
1.
Webb PM, Jordan SJ. Global epidemiology of epithelial ovarian cancer. Nat Rev Clin Oncol. 2024;21(5):389-400.
2.
Siegel RL, Giaquinto AN, Jemal A. Cancer statistics, 2024 [published correction appears in CA Cancer J Clin. 2024;74(2):203. CA Cancer J Clin. 2024;74(1):12-49.
3.
Ali AT, Al-Ani O, Al-Ani F. Epidemiology and risk factors for ovarian cancer. Menopause Review 2023;22(2):93-104.
4.
Feeney L, Harley IJ, McCluggage WG, et al. Liquid biopsy in ovarian cancer: Catching the silent killer before it strikes. World J Clin Oncol. 2020;11(11):868-889.
5.
Coburn SB, Bray F, Sherman ME, et al. International patterns and trends in ovarian cancer incidence, overall and by histologic subtype. Int J Cancer. 2017;140(11):2451-2460.
6.
Ali AT. Towards Prevention of Ovarian Cancer. Curr Cancer Drug Targets. 2018;18(6):522-537.
7.
Köbel M, Kang EY. The Evolution of Ovarian Carcinoma Subclassification. Cancers (Basel) 2022;14(2):416.
8.
Köbel M, Kalloger SE, Lee S, et al. Biomarker-based ovarian carcinoma typing: a histologic investigation in the ovarian tumor tissue analysis consortium. Cancer Epidemiol Biomarkers Prev. 2013;22(10):1677-1686.
9.
Sideris M, Menon U, Manchanda R. Screening and prevention of ovarian cancer. Med J Aust. 2024;220(5):264-274.
10.
Pavlik EJ, van Nagell JR Jr, Dietrich CS 3rd, et al. Compelling Story of Ovarian Cancer Screening. J Clin Oncol. 2024;42(10):1091-1094.
11.
Whelan E, Kalliala I, Semertzidou A, et al. Risk Factors for Ovarian Cancer: An Umbrella Review of the Literature. Cancers (Basel). 2022;14(11):2708.
12.
Bandera EV, Lee VS, Rodriguez-Rodriguez L, et al. Racial/ethnic disparities in ovarian cancer treatment and survival. Clin Cancer Res 2016; 22:5909-5914.
13.
Kuchenbaecker KB, Hopper JL, Barnes DR, et al. Risks of breast, ovarian, and contralateral breast cancer for BRCA1 and BRCA2 mutation carriers. JAMA 2017; 317:2402-2416.
14.
Lee AW, Ness RB, Roman LD, et al. Ovarian Cancer Association Consortium. Association between menopausal estrogen-only therapy and ovarian carcinoma risk. Obstet Gynecol 2016; 127: 828-836.
15.
Gaitskell K, Green J, Pirie K, et al.. Histological subtypes of ovarian cancer associated with parity and breastfeeding in the prospective Million Women Study. Int J Cancer 2018; 142: 281-9.
16.
Wang T, Read SH, Moino D, et al. Tobacco Smoking and Survival Following a Diagnosis with Ovarian Cancer. Cancer Epidemiol Biomarkers Prev. 2022;31(7):1376-1382.
17.
Bakken K, Alsaker E, Eggen AE, Lund E. Hormone replacement therapy and incidence of hormone-dependent cancers in the Norwegian Women and Cancer study. Int J Cancer. 2004; 112(1):130-4.
18.
Xiang H, Wang L, Sun L, Xu S. The risk of ovarian cancer in hormone replacement therapy users: a systematic review and meta-analysis. Front Endocrinol (Lausanne). 2024; 15:1414968.
19.
Garg PP, Kerlikowske K, Subak L, et al. Hormone replacement therapy and the risk of epithelial ovarian carcinoma: a meta-analysis. Obstet Gynecol. 1998, 92:472–9.
20.
Coughlin SS, Giustozzi A, Smith SJ, Lee NC. A meta-analysis of estrogen replacement therapy and risk of epithelial ovarian cancer. J Clin Epidemiol. 2000, 53:367–75.
21.
Husby A, Wohlfahrt J, Melbye M. Pregnancy duration and ovarian cancer risk: A 50-year nationwide cohort study. Int J Cancer. 2022;151(10):1717-1725.
22.
Babic A, Sasamoto N, Rosner BA, et al. Association Between Breastfeeding and Ovarian Cancer Risk. JAMA Oncol. 2020; 6(6):e200421.
23.
Avramenko, A.S., Flanagan, J.M. An epigenetic hypothesis for ovarian cancer prevention by oral contraceptive pill use. Clin Epigenet 2023, 15, 165.
24.
Connaughton M, Dabagh M. Association of Hypertension and Organ-Specific Cancer: A Meta-Analysis. Healthcare 2022;10(6):1074.
25.
European Comission, EuroStat Data. 22% of people in the EU have high blood pressure. ec.europa.eu. [available online: https://ec.europa.eu/eurostat/..., 13.01.2025).
26.
Drab A, Kanadys W, Malm M, Wdowiak K, Dolar-Szczasny J, Barczyński B. Association of endometrial cancer risk with hypertension- an updated meta-analysis of observational studies. Sci Rep. 2024, 22;14(1):24884.
27.
Gkretsi V, Stylianopoulos T. Cell Adhesion and Matrix Stiffness: Coordinating Cancer Cell Invasion and Metastasis. Front Oncol. 2018;8:145.
28.
Yang P, Elhalawani H, Shi Y, et al. A large-scale retrospective study of the overall survival outcome in nasopharyngeal carcinoma with hypertension in Chinese population. Oncotarget. 2017;8:75577–75586.
29.
Deckers IA, van den Brandt PA, van Engeland M, et al. Polymorphisms in genes of the renin-angiotensin-aldosterone system and renal cell cancer risk: Interplay with hypertension and intakes of sodium, potassium and fluid: RAAS Polymorphisms and RCC Risk: Interplay with Hypertension and Diet. Int. J. Cancer. 2015;136:1104–1116.
30.
Sobczuk P, Szczylik C, Porta C, et al. Renin angiotensin system deregulation as renal cancer risk factor. Oncol. Lett. 2017;14:5059–5068. doi: 10.3892/ol.2017.6826.
31.
Jabłońska-Trypuć A, Matejczyk M, Rosochnowlei S. Matrix metalloproteinases (MMPs), the main extracellular matrix (ECM) enzymes in collagen degradation, as a target for anticancer drugs. J. Enzyme Inhib. Med. Chem. 2016;31:177–183.
32.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 2021;372:n71.
33.
Ottawa Hospital Research Institute. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses, (Online). 2011; (cited 31 July 2024; available from: URL http://www.ohri.ca/programs/cl...).
34.
DerSimonian R, Laird N. Meta-analysis in clinical trials revisited. Contemp. Clin. Trials 2015, 45, 139–145.
35.
Higgins J, Thomas J. Cochrane Handbook for Systematic Reviews of Interventions, 2nd ed.; John Wiley and Sons, Ltd.: Chichester, UK, 2019; pp. 143–176.
36.
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat. Med. 2002, 21, 1539–1558.
37.
Egger M, Smith GD, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315: 629–634.
38.
Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics 1994, 50: 1088–1101.
39.
Hayden JA, van der Windt DA, Cartwright JL P, et al. Assessing bias in studies of prognostic factors. Ann. Intern. Med. 2013, 158: 280-286.
40.
Parazzini F, Moron, S, La Vecchia C, et al. Ovarian cancer risk and history of selected medical conditions linked with female hormones. European Journal of Cancer 1997, 33(10): 1634–1637.
41.
Soler M, Chatenoud L, Negri E, et al. Hypertension and Hormone-Related Neoplasms in Women. Hypertension 1999, 34(2): 320–325.
42.
Brinton LA, Sakoda LC, Frederiksen K, et al. Relationships of uterine and ovarian tumors to pre-existing chronic conditions. Gynecol Oncol. 2007;107(3):487-94.
43.
Chia VM, O'Malley CD, Danese MD, et al. Prevalence and incidence of comorbidities in elderly women with ovarian cancer. Gynecol Oncol. 2013;129(2):346-52.
44.
Huang T, Poole EM, Eliassen AH, Okereke OI, Kubzansky LD, Sood AK, Forman JP, Tworoger SS. Hypertension, use of antihypertensive medications, and risk of epithelial ovarian cancer. Int J Cancer. 2016;139(2):291-9.
45.
Chen Y, Zhang L, Liu W, Wang K. Case-control study of metabolic syndrome and ovarian cancer in Chinese population. Nutr Metab (Lond). 2017:14:21.
46.
Michels KA, McNeel TS, Trabert B. Metabolic syndrome and risk of ovarian and fallopian tube cancer in the United States: An analysis of linked SEER-Medicare data. Gynecol Oncol. 2019;155(2):294-300.
47.
Staples JN, Peres LC, Camacho F, et al. Cardiometabolic comorbidities and epithelial ovarian cancer risk among African-American women in the African-American Cancer Epidemiology Study (AACES). Gynecol Oncol. 2020;158(1):123-129.
48.
Alrobaiq BM, Alharbi RS, Alhoshan FS, Alnasyan MA, Alahideb A, Omair A. Hypertension and Ovarian Cancer: A Case-Control Study in Saudi Arabia. Cureus. 2023; 15(2):e35294.
49.
Carlos-Escalante JA, de Jesús-Sánchez M, Rivas-Castro A, et al. The Use of Antihypertensive Drugs as Coadjuvant Therapy in Cancer. Front Oncol. 2021;11:660943.
50.
Mravec B, Horvathova L, Hunakova L. Neurobiology of Cancer: The Role of β-Adrenergic Receptor Signaling in Various Tumor Environments. Int J Mol Sci, 2020, 21(21):1–24.
51.
Wegman-Ostrosky T, Soto-Reyes E, Vidal-Millán S, Sánchez-Corona J. The Renin-Angiotensin System Meets the Hallmarks of Cancer. JRAAS - J Renin-Angiotensin-Aldosterone Syst 2015, 16(2):227–33.
52.
Stocks T, Van Hemelrijck ., Manjer J, et al. Blood pressure and risk of cancer incidence and mortality in the Metabolic Syndrome and Cancer Project. Hypertension. 2012;59:802–810.
53.
Lindgren AM, Nissinen AM, Tuomilehto JO,et al. Cancer pattern among hypertensive patients in North Karelia, Finland. J. Hum. Hypertens. 2005;19:373–379.
54.
Behrens I, Basit S, Jensen A, Lykke JA, et al. Hypertensive disorders of pregnancy and subsequent risk of solid cancer—A nationwide cohort study: Hypertensive disorders of pregnancy and solid cancer. Int. J. Cancer. 2016;139:58–64.
55.
Lofterød T, Frydenberg H, Flote V, et al. Exploring the effects of lifestyle on breast cancer risk, age at diagnosis, and survival: The EBBA-Life study. Breast Cancer Res. Treat. 2020;182:215–227.
56.
Sun L-M, Kuo H-T, Jeng L-B, et al. Hypertension and subsequent genitourinary and gynecologic cancers risk: A population-based cohort study. Medicine 2015;94:e753.
57.
Yassin S, Younis M, Abuzerr S, et al. Extrinsic risk factors for women breast cancer in Gaza strip, Palestine: Associations and interactions in a case-control study. Adv. Breast Cancer Res. 2019;08:11–30.
58.
Pereira A, Garmendia ML, Alvarado M., et al. Hypertension and the risk of breast cancer in Chilean women: A case-control study. Asian Pac. J. Cancer Prev. 2012;13:5829–5834.
59.
Chuang S-C, Wu G-J, Lu Y-S, et al. Associations between medical conditions and breast cancer risk in Asians: A nationwide population-based study in Taiwan. PLoS ONE. 2015;10:e0143410.
60.
Beji NK, Reis N. Risk factors for breast cancer in Turkish women: A hospital-based case-control study. Eur. J. Cancer Care. 2007;16:178–184.
61.
Jung SJ, Song ., Choi J-Y, Song N, et al. Association of selected medical conditions with breast cancer risk in Korea. J. Prev. Med. Public Health. 2013;46:346–352.
62.
Lee SH, Lee HA, Lee SS, et al. Clinical impact of pre-hypertension on the risk of cancer in male and female subjects. Sci. Rep. 2020;10:9974.
63.
Ko S, Yoon S-J, Kim D, et al. Metabolic risk profile and cancer in Korean men and women. J. Prev. Med. Public Health. 2016;49:143–152.
64.
Hirai HW, Ching JYL, Wu JCY, et al. Risk factors for advanced colorectal neoplasms in the proximal colon in 6218 subjects undergoing complete colonoscopy: Risk factor of proximal colonic lesions. J. Gastroenterol. Hepatol. 2019;34:113–119.
65.
Samarakoon YM, Gunawardena NS, Pathirana A. Behavioral, familial and comorbid illness risk factors of colorectal cancer: A case control study. Ceylon Med. J. 2018;63:113–118.
66.
Dickerman BA, Torfadottir JE, Valdimarsdottir UA, et al. Midlife metabolic factors and prostate cancer risk in later life. Int. J. Cancer. 2018;142:1166–1173.
67.
Teleka S, Jochems SHJ, Häggström C, et al. Association between blood pressure and BMI with bladder cancer risk and mortality in 340,000 men in three Swedish cohorts. Cancer Med. 2021;10:1431–1438.
68.
Peeters PH, van Noord PAHoes AW, Grobbee DE. Hypertension, antihypertensive drugs, and mortality from cancer among women. J. Hypertens. 1998;16:941–947.
69.
Navin S, Ioffe V. The association between hypertension and prostate cancer. Rev. Urol. 2017;19:113–118.
70.
Azzam N, AlRuthia Y, Alharbi O, et al. Predictors of survival among colorectal cancer patients in a low incidence area. Cancer Manag. Res. 2020;12:451–459.
71.
Dibaba D, Ogunsina K, Braithwaite D, et al. Metabolic syndrome and risk of breast cancer mortality by menopause, obesity, and subtype. Breast Cancer Res. Treat. 2019;174:209–218.
72.
Tini G, Sarocchi M, Tocci G, et al. Arterial hypertension in cancer: The elephant in the room. Int. J. Cardiol. 2019;281:133–139.
73.
Harding JL, Sooriyakumaran M, Anstey KJ, et al. Hypertension, antihypertensive treatment and cancer incidence and mortality: A pooled collaborative analysis of 12 Australian and New Zealand cohorts. J. Hypertens. 2016;34:149–155.
74.
Emaus A, Veierød MB, Tretli S, Finstad S.E., Selmer R., Furberg A.-S., Bernstein L., Schlichting E., Thune I. Metabolic profile, physical activity, and mortality in breast cancer patients. Breast Cancer Res. Treat. 2010;121:651–660.
75.
Hu D, Jia R, Zhang X, et al. Identification of optimal baseline blood pressure predicting postoperative digestive tract cancer-specific mortality in the FIESTA cohort involving 6865 patients. J. Cancer. 2019;10:1794–1799.
76.
Mumby S, Perros F, Hui C, et al. Extracellular matrix degradation pathways and fatty acid metabolism regulate distinct pulmonary vascular cell types in pulmonary arterial hypertension. Pulm Circ. 2021;11(1):2045894021996190.
77.
Duco MR, Murdock JL, Reeves DJ. Vascular endothelial growth factor inhibitor induced hypertension: Retrospective analysis of the impact of blood pressure elevations on outcomes. J Oncol Pharm Pract. 2022;28(2):265-273.
78.
Li F, Du H, Li S, Liu J. The Association Between Metabolic Syndrome and Gastric Cancer in Chinese. Front Oncol. 2018;8:326.
79.
Gobin E, Bagwell K, Wagner J, et al. A pan-cancer perspective of matrix metalloproteases (MMP) gene expression profile and their diagnostic/prognostic potential. BMC Cancer. 2019;19(1):581.
80.
Belo VA, Guimarães DA, Castro MM. Matrix Metalloproteinase 2 as a Potential Mediator of Vascular Smooth Muscle Cell Migration and Chronic Vascular Remodeling in Hypertension. J Vasc Res. 2015;52(4):221-231.
81.
Minlikeeva AN, Freudenheim JL, Cannioto RA, et al. History of hypertension, heart disease, and diabetes and ovarian cancer patient survival: evidence from the ovarian cancer association consortium. Cancer Causes Control. 2017;28(5):469-486.
82.
Wentzensen N, Poole EM, Trabert B, et al. Ovarian Cancer Risk Factors by Histologic Subtype: An Analysis From the Ovarian Cancer Cohort Consortium. J Clin Oncol. 2016;34(24):2888-2898.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.