Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
LIPID DISORDERS / CLINICAL RESEARCH
The association of low-density lipoprotein cholesterol with apolipoprotein B ratio and sarcopenia: a cross-sectional study
1
The First Affiliated Hospital of Shaoyang University, Changsha, Hunan, China
2
The First Hospital of Hunan University of Chinese Medicine, Changsha, Hunan, China
Submission date: 2025-08-21
Final revision date: 2025-11-04
Acceptance date: 2025-11-20
Online publication date: 2025-11-28
Publication date: 2026-04-12
Corresponding author
Arch Med Sci 2026;22(3)
KEYWORDS
TOPICS
ABSTRACT
Introduction:
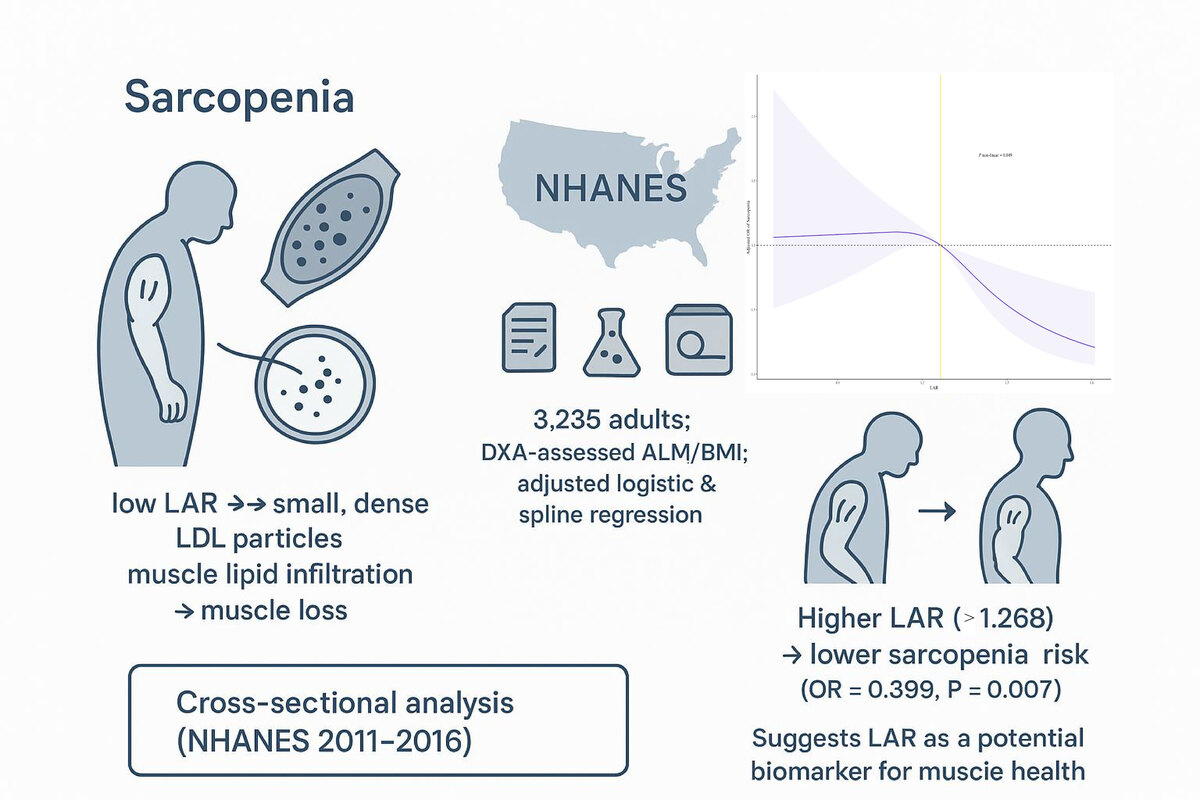
Sarcopenia is increasingly linked to metabolic dysregulation, including dyslipidemia. The low-density lipoprotein cholesterol with apolipoprotein B (LDL-C/ApoB) ratio (LAR), reflecting cholesterol content per atherogenic lipoprotein particle, may serve as a novel biomarker for sarcopenia risk. This study aimed to investigate the association between LAR and sarcopenia using data from the National Health and Nutrition Examination Survey (NHANES).
Material and methods:
Data from NHANES cycles 2011–2016 were analyzed between July 2024 and February 2025. Sarcopenia was defined using dual-energy X-ray absorptiometry (DXA)-derived appendicular lean mass (ALM) standardized to body mass index (BMI). Multivariable logistic regression, restricted cubic spline (RCS) regression analysis, subgroup analysis, and interaction tests were applied to evaluate the relationship between LAR and sarcopenia, adjusting for covariates.
Results:
A negative correlation between LAR and sarcopenia was observed in 3,235 participants included in the study (OR = 0.399, 95% CI: 0.224–0.712, p = 0.007), which was further confirmed to be non-linear via RCS regression analysis (pnon-linear = 0.037), with one significant inflection point identified, and participants with LAR ≥ 1.268 demonstrated a significantly reduced risk of sarcopenia. Subgroup analyses and interaction tests indicated that the association between LAR and sarcopenia remained consistent across different subgroups and was not modified by other covariates.
Conclusions:
Elevated LAR is significantly associated with lower sarcopenia risk, suggesting its potential role as a biomarker for muscle health. Further studies are needed to elucidate underlying mechanisms and validate these findings prospectively.
Sarcopenia is increasingly linked to metabolic dysregulation, including dyslipidemia. The low-density lipoprotein cholesterol with apolipoprotein B (LDL-C/ApoB) ratio (LAR), reflecting cholesterol content per atherogenic lipoprotein particle, may serve as a novel biomarker for sarcopenia risk. This study aimed to investigate the association between LAR and sarcopenia using data from the National Health and Nutrition Examination Survey (NHANES).
Material and methods:
Data from NHANES cycles 2011–2016 were analyzed between July 2024 and February 2025. Sarcopenia was defined using dual-energy X-ray absorptiometry (DXA)-derived appendicular lean mass (ALM) standardized to body mass index (BMI). Multivariable logistic regression, restricted cubic spline (RCS) regression analysis, subgroup analysis, and interaction tests were applied to evaluate the relationship between LAR and sarcopenia, adjusting for covariates.
Results:
A negative correlation between LAR and sarcopenia was observed in 3,235 participants included in the study (OR = 0.399, 95% CI: 0.224–0.712, p = 0.007), which was further confirmed to be non-linear via RCS regression analysis (pnon-linear = 0.037), with one significant inflection point identified, and participants with LAR ≥ 1.268 demonstrated a significantly reduced risk of sarcopenia. Subgroup analyses and interaction tests indicated that the association between LAR and sarcopenia remained consistent across different subgroups and was not modified by other covariates.
Conclusions:
Elevated LAR is significantly associated with lower sarcopenia risk, suggesting its potential role as a biomarker for muscle health. Further studies are needed to elucidate underlying mechanisms and validate these findings prospectively.
REFERENCES (26)
1.
Cruz-Jentoft AJ, Bahat G, Bauer J, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 2019; 48: 601.
2.
Beaudart C, Demonceau C, Reginster JY, et al. Sarcopenia and health-related quality of life: A systematic review and meta-analysis. J Cachexia Sarcopenia Muscle 2023; 14:1228-43.
4.
Petermann-Rocha F, Balntzi V, Gray SR, et al. Global prevalence of sarcopenia and severe sarcopenia: a systematic review and meta-analysis. J Cachexia Sarcopenia Muscle 2022; 13: 86-99.
5.
Nishikawa H, Asai A, Fukunishi S, Nishiguchi S, Higuchi K. Metabolic syndrome and sarcopenia. Nutrients 2021; 13: 3519.
6.
Al Saedi A, Debruin DA, Hayes A, Hamrick M. Lipid metabolism in sarcopenia. Bone 2022; 164: 116539.
7.
Bi B, Dong X, Yan M, et al. Dyslipidemia is associated with sarcopenia of the elderly: a meta-analysis. BMC Geriatr 2024; 24:181.
8.
Lin Y, Zhong S, Sun Z. Association between serum triglyceride to high-density lipoprotein cholesterol ratio and sarcopenia among elderly patients with diabetes: a secondary data analysis of the China Health and Retirement Longitudinal Study. BMJ Open 2023; 13: e075311.
9.
Kawamoto R, Kohara K, Katoh T, et al. Changes in oxidized low-density lipoprotein cholesterol are associated with changes in handgrip strength in Japanese community-dwelling persons. Endocrine 2015; 48: 871-7.
10.
Sousa-Victor P, Garcia-Prat L, Munoz-Canoves P. Control of satellite cell function in muscle regeneration and its disruption in ageing. Nat Rev Mol Cell Biol 2022; 23: 204-26.
11.
Sheng G, Liu D, Kuang M, Zhong Y, Zhang S, Zou Y. Utility of non-high-density lipoprotein cholesterol to high-density lipoprotein cholesterol ratio in evaluating incident diabetes risk. Diabetes Metab Syndr Obes 2022; 15: 1677-86.
12.
Kim SW, Jee JH, Kim HJ, et al. Non-HDL-cholesterol/HDL-cholesterol is a better predictor of metabolic syndrome and insulin resistance than apolipoprotein B/apolipoprotein A1. Int J Cardiol 2013; 168: 2678-83.
13.
Iannuzzi A, Giallauria F, Gentile M, et al. Association between Non-HDL-C/HDL-C ratio and carotid intima-media thickness in post-menopausal women. J Clin Med 2021; 11: 78.
14.
Zhao W, Gong W, Wu N, et al. Association of lipid profiles and the ratios with arterial stiffness in middle-aged and elderly Chinese. Lipids Health Dis 2014; 13: 37.
15.
Nishikawa H, Fukunishi S, Asai A, Yokohama K, Nishiguchi S, Higuchi K. Pathophysiology and mechanisms of primary sarcopenia (Review). Int J Mol Med 2021; 48: 156.
16.
Barrera G, Pizzimenti S, Daga M, et al. Lipid peroxidation-derived aldehydes, 4-hydroxynonenal and malondialdehyde in aging-related disorders. Antioxidants (Basel) 2018; 7: 102.
17.
Yang X, Zhong Z. The association between non-high-density lipoprotein cholesterol to high-density lipoprotein cholesterol ratio (NHHR) and sarcopenia: A cross-sectional study. Exp Gerontol 2025; 200: 112680.
18.
Lin W, Luo S, Li W, et al. Association between the non-HDL-cholesterol to HDL- cholesterol ratio and abdominal aortic aneurysm from a Chinese screening program. Lipids Health Dis 2023; 22: 187.
19.
Wang N, Chen M, Fang D. Relationship between serum triglyceride to high-density lipoprotein cholesterol ratio and sarcopenia occurrence rate in community-dwelling Chinese adults. Lipids Health Dis 2020; 19: 248.
20.
Navab M, Anantharamaiah GM, Reddy ST, Van Lenten BJ, Ansell BJ, Fogelman AM. Mechanisms of disease: proatherogenic HDL – an evolving field. Nat Clin Pract Endocrinol Metab 2006; 2: 504-11.
21.
Gong H, Liu Y, Lyu X, Dong L, Zhang X. Lipoprotein subfractions in patients with sarcopenia and their relevance to skeletal muscle mass and function. Exp Gerontol 2022; 159: 111668.
22.
Studenski SA, Peters KW, Alley DE, et al. The FNIH sarcopenia project: rationale, study description, conference recommendations, and final estimates. J Gerontol A Biol Sci Med Sci 2014; 69: 547-58.
23.
Hirano T, Ito Y, Yoshino G. Measurement of small dense low-density lipoprotein particles. J Atheroscler Thromb 2005; 12: 67-72.
24.
Kamanna VS, Kashyap ML. Mechanism of action of niacin. Am J Cardiol 2008; 101 (8A): 20B-6B.
25.
Sniderman A, Williams K, Cobbaert C. ApoB versus non-HDL-C: what to do when they disagree. Curr Atheroscler Rep 2009; 11: 358-63.
26.
Boren J, Chapman MJ, Krauss RM, et al. Low-density lipoproteins cause atherosclerotic cardiovascular disease: pathophysiological, genetic, and therapeutic insights: a consensus statement from the European Atherosclerosis Society Consensus Panel. Eur Heart J 2020; 41: 2313-30.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.