Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
CARDIOVASCULAR PREVENTION / RESEARCH PAPER
Exploring Prevalence and Determinants of Early Acute Coronary Syndrome in Kosovo: A Population Snapshot with Sex Differences
1
University of Prishtina, Kosovo
2
Medical Faculty, University of Prishtina, Kosovo
3
Department of Cardiology and Adult Congenital Heart Diseases, Polish Mother's Memorial Hospital Research Institute, Łódź, Poland, Poland
4
Imperial College London, United Kingdom
5
Medical Faculty, University of Pristina, Kosovo;
University Clinical Centre of Kosovo, Prishtina, Republic of Kosovo, Kosovo
Submission date: 2026-04-16
Final revision date: 2026-04-27
Acceptance date: 2026-04-29
Online publication date: 2026-04-29
KEYWORDS
Early-onset ACSKosovocardiovascular risk factorsbiochemical indicescross-sectionalretrospective study
TOPICS
ABSTRACT
Introduction:
Acute coronary syndrome (ACS) in young adults represents an important growing clinical challenge worldwide. This study aimed to evaluate the clinical characteristics and predictors of premature ACS, with particular emphasis on sex differences and cardiovascular risk factors.
Material and methods:
We retrospectively analyzed 2,909 patients with ACS treated at the University Clinical Centre of Kosovo. Of these, 587 had premature ACS (men <55 years; women <65 years). Data on CV risk factors, electrocardiographic, echocardiographic, angiographic findings and medications, were collected from medical records.
Results:
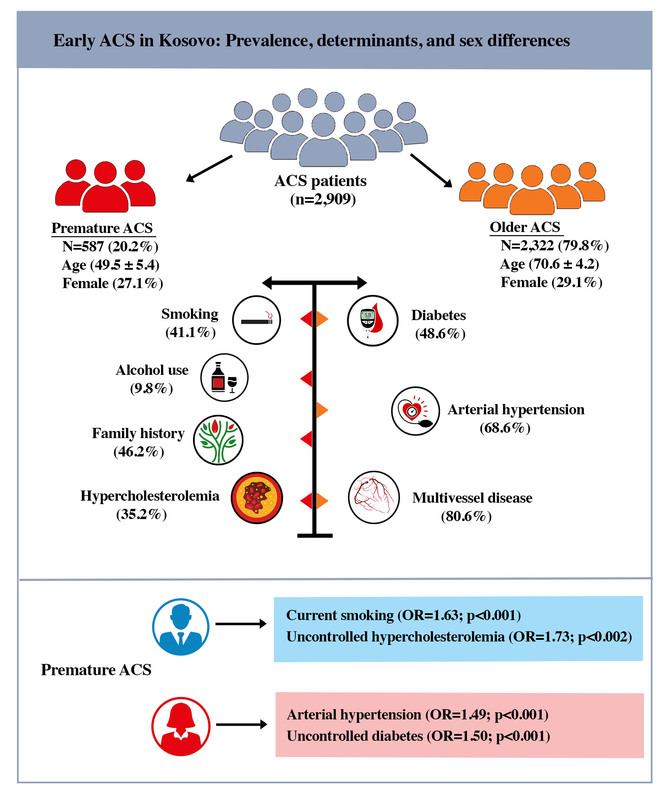
Patients with premature ACS had a higher prevalence of hypercholesterolemia (35.2 vs. 25.1%; p<0.001), uncontrolled hypercholesterolemia (40.4 vs. 26.9%; p<0.001), current smoking (41.1 vs. 22.9%; p<0.001) and family history of CAD (46.2 vs. 32.4%; p<0.001), but a lower prevalence of diabetes, hypertension, and uncontrolled diabetes (all p<0.001) compared with older patients. Among premature ACS patients, women had lower smoking, alcohol use, and uncontrolled hypercholesterolemia, but higher diabetes and hypertension than men. In multivariable analysis, smoking (OR 1.59), uncontrolled hypercholesterolemia (OR 1.71), and family history (OR 1.66) independently predicted premature ACS (all p<0.001). These associations were consistent across sexes: in women, uncontrolled diabetes (OR 1.51) and hypertension (OR 1.49) were additional predictors, whereas in men, smoking (OR 1.63) and uncontrolled hypercholesterolemia (OR 1.73) predominated.
Conclusions:
Premature ACS, diagnosed in every 5th patients in Kosovo, is mainly associated with uncontrolled hypercholesterolemia and smoking, while diabetes, hypertension, and hyperglycemia are less common than in older patients. Clear sex differences observed, with a more cardiometabolic profile in women and lifestyle-related risk factors in men.
Acute coronary syndrome (ACS) in young adults represents an important growing clinical challenge worldwide. This study aimed to evaluate the clinical characteristics and predictors of premature ACS, with particular emphasis on sex differences and cardiovascular risk factors.
Material and methods:
We retrospectively analyzed 2,909 patients with ACS treated at the University Clinical Centre of Kosovo. Of these, 587 had premature ACS (men <55 years; women <65 years). Data on CV risk factors, electrocardiographic, echocardiographic, angiographic findings and medications, were collected from medical records.
Results:
Patients with premature ACS had a higher prevalence of hypercholesterolemia (35.2 vs. 25.1%; p<0.001), uncontrolled hypercholesterolemia (40.4 vs. 26.9%; p<0.001), current smoking (41.1 vs. 22.9%; p<0.001) and family history of CAD (46.2 vs. 32.4%; p<0.001), but a lower prevalence of diabetes, hypertension, and uncontrolled diabetes (all p<0.001) compared with older patients. Among premature ACS patients, women had lower smoking, alcohol use, and uncontrolled hypercholesterolemia, but higher diabetes and hypertension than men. In multivariable analysis, smoking (OR 1.59), uncontrolled hypercholesterolemia (OR 1.71), and family history (OR 1.66) independently predicted premature ACS (all p<0.001). These associations were consistent across sexes: in women, uncontrolled diabetes (OR 1.51) and hypertension (OR 1.49) were additional predictors, whereas in men, smoking (OR 1.63) and uncontrolled hypercholesterolemia (OR 1.73) predominated.
Conclusions:
Premature ACS, diagnosed in every 5th patients in Kosovo, is mainly associated with uncontrolled hypercholesterolemia and smoking, while diabetes, hypertension, and hyperglycemia are less common than in older patients. Clear sex differences observed, with a more cardiometabolic profile in women and lifestyle-related risk factors in men.
REFERENCES (29)
1.
Roth GA, Mensah GA, Johnson CO, Addolorato G, Ammirati E, Baddour LM, et al. Global burden of cardiovascular diseases and risk factors, 1990–2019: update from the GBD 2019 study. J Am Coll Cardiol. 2020;76(25):2982–3021.
2.
Xu S, Zhang Y, Jiang W, Liu J, Li W, Sun L, et al. Global burden of atherosclerotic cardiovascular disease attributed to lifestyle and metabolic risks. Sci China Life Sci. 2025.
3.
Hoxha V, Dragusha E, Morina S, Dragusha E, Thaqi S, Henein MY et al. Sex-Related Differences in Predictors of Acute Coronary Syndrome in Kosovo: A Cross-Sectional Study. J Clin Med. 2025 Nov 11;14(22):8002.
4.
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study). Lancet. 2004; 364 (9438): 937-952.
5.
Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease. Circulation. 2019; 140: e596–e646.
6.
Virani SS, Alonso A, Aparicio HJ, Benjamin EJ, Bittencourt MS, Callaway CW, et al. Heart disease and stroke statistics—2021 update: a report from the American Heart Association. Circulation. 2021;143(8):e254–e743.
7.
Bredehorst M, Müller OJ, Katus HA, Sliwa K, Schulz-Menger J, Thiele H, et al. Recommendations for the primary prevention of atherosclerotic cardiovascular disease: a systematic guideline review. Front Med (Lausanne). 2024;11:1494234.
8.
Khot UN, Khot MB, Bajzer CT, Sapp SK, Ohman EM, Brener SJ, et al. Prevalence of conventional risk factors in patients with coronary heart disease. JAMA. 2003;290(7):898–904.
9.
Banach M, Surma S. Monitoring of traditional atherosclerosis cardiovascular disease risk factors - is it enough to prevent premature acute coronary syndrome? Lancet Reg Health Eur. 2024 Feb 13;38:100866.
10.
Bytyci I, Toth P, Bytyqi S, Henein M, Banach M. Worldwide patterns for premature atherosclerotic cardiovascular disease: a meta-analysis. Circulation. 2025;152(25).
11.
Vogel B, Acevedo M, Appelman Y, Merz CNB, Chieffo A, Figtree GA, et al. The Lancet women and cardiovascular disease Commission: reducing the global burden by 2030. Lancet. 2021;397(10292):2385–2438.
12.
Regitz-Zagrosek V, Oertelt-Prigione S, Prescott E, Franconi F, Gerdts E, Foryst-Ludwig A, et al. Gender in cardiovascular diseases: impact on clinical manifestations, management, and outcomes. Nat Rev Cardiol. 2016;13(9):516–528.
13.
Stringhini S, Carmeli C, Jokela M, Avendaño M, Muennig P, Guida F, et al. Socioeconomic status and the 25×25 risk factors as determinants of premature mortality: a multicohort study. Lancet. 2017;389(10075):1229–1237.
14.
Ebong IA, Goff DC, Rodriguez CJ, Chen H, Bertoni AG. The role of psychosocial stress in cardiovascular disease: implications for women. J Am Coll Cardiol. 2024.
15.
Davies MJ, Aroda VR, Collins BS, Gabbay RA, Green J, Maruthur NM, et al. Management of hyperglycaemia in type 2 diabetes, 2022. Diabetologia. 2022;65(12):1925–1966.
16.
McEvoy JW, McCarthy CP, Bruno RM, Brouwers S, Canavan MD, Ceconi C, et al. 2024 ESC Guidelines for the management of elevated blood pressure and hypertension. Eur Heart J. 2024;45(38):3912–4018.
17.
Visseren FLJ, Mach F, Smulders YM, Carballo D, Koskinas KC, Back M, et al. 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J. 2021;42(34):3227–3337.
18.
Dagenais GR, Leong DP, Rangarajan S, Lanas F, Lopez-Jaramillo P, Gupta R, et al.Variations in common diseases, hospital admissions, and deaths in middle-aged adults in 21 countries from five continents (PURE study): a prospective cohort study. Lancet. 2020;395:785–794.
19.
Meng X, Yuan J, Li W, Chen J, Wang H, Liu Z, et al. Predictive value of fasting plasma glucose for short-term prognosis in patients with type 2 diabetes mellitus after acute decompensated heart failure. Front Endocrinol (Lausanne). 2023; 14:1171583.
20.
Mitchell C, Rahko PS, Blauwet LA, Canaday B, Finstuen JA, Foster MC, et al. Guidelines for performing a comprehensive transthoracic echocardiographic examination in adults: recommendations from the American Society of Echocardiography. J Am Soc Echocardiogr. 2019;32(1):1–64.
21.
Kirkwood BR, Sterne JAC. Essential Medical Statistics. 2nd ed. Oxford: Blackwell Science; 2003.
22.
Joseph P, Leong D, McKee M, Anand SS, Schwalm JD, Teo K, et al. Reducing the global burden of cardiovascular disease, part 1: the epidemiology and risk factors. Circ Res. 2017;121(6):677–694.
23.
Todorovic J, Santric Milicevic MM, Terzic Z, Stevanovic A, Terzic-Supic Z, Stamenkovic Z, et al. Burden of alcohol use disorder in Balkan countries. Eur J Public Health. 2022;32: ckac130.190.
24.
Khera AV, Won HH, Peloso GM, O’Dushlaine C, Liu D, Stitziel NO, et al. Diagnostic yield and clinical utility of sequencing familial hypercholesterolemia genes in patients with severe hypercholesterolemia. J Am Coll Cardiol. 2016;67(22):2578–2589.
25.
Andersson C, Vasan RS. Epidemiology of cardiovascular disease in young individuals. Nat Rev Cardiol. 2018;15(4):230–240.
26.
Banach M, Fras Z, Gaita D, Pecin I, Bajraktari G, Bjelakovic B, et al. The European Program for Prevention (EPP) – implementing proven preventing measures now! Global Heart. 2025;20(1):103.
27.
Banach M, Mazidi M, Mikhailidis DP, Toth PP, Jozwiak J, Rysz J et al. Association between phenotypic familial hypercholesterolaemia and telomere length in US adults: results from a multi-ethnic survey. Eur Heart J. 2018 Oct 21;39(40):3635-3640.
28.
Maas AHEM, Appelman YEA. Gender differences in coronary heart disease. Neth Heart J. 2010;18(12):598–603.
29.
Baigent C, Keech A, Kearny PM, Blackwell L, Buck G, Pollicino C, et al. Cholesterol Treatment Trialists collaborators. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90.056 participants in 14 randomised trials of statins. Lancet. 2005; 366: 1267-78.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.