Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
NEUROLOGY / RESEARCH PAPER
Deciphering the Interplay Between Inflammatory Factors and Brain Structural Features in Epilepsy
1
he Third People's Hospital of Chengdu, China
Submission date: 2025-07-19
Final revision date: 2025-12-28
Acceptance date: 2026-01-21
Online publication date: 2026-05-01
KEYWORDS
EpilepsyInflammatory factorsMendelian randomizationBrain structural featuresUnsupervised Deep Learning-derived Imaging Phenotypes
TOPICS
ABSTRACT
Introduction:
To evaluate potential causal links among circulating inflammatory factors, deep learning–derived brain structural phenotypes (unimodal deep imaging phenotypes, UDIPs), and epilepsy using Mendelian randomization (MR).
Material and methods:
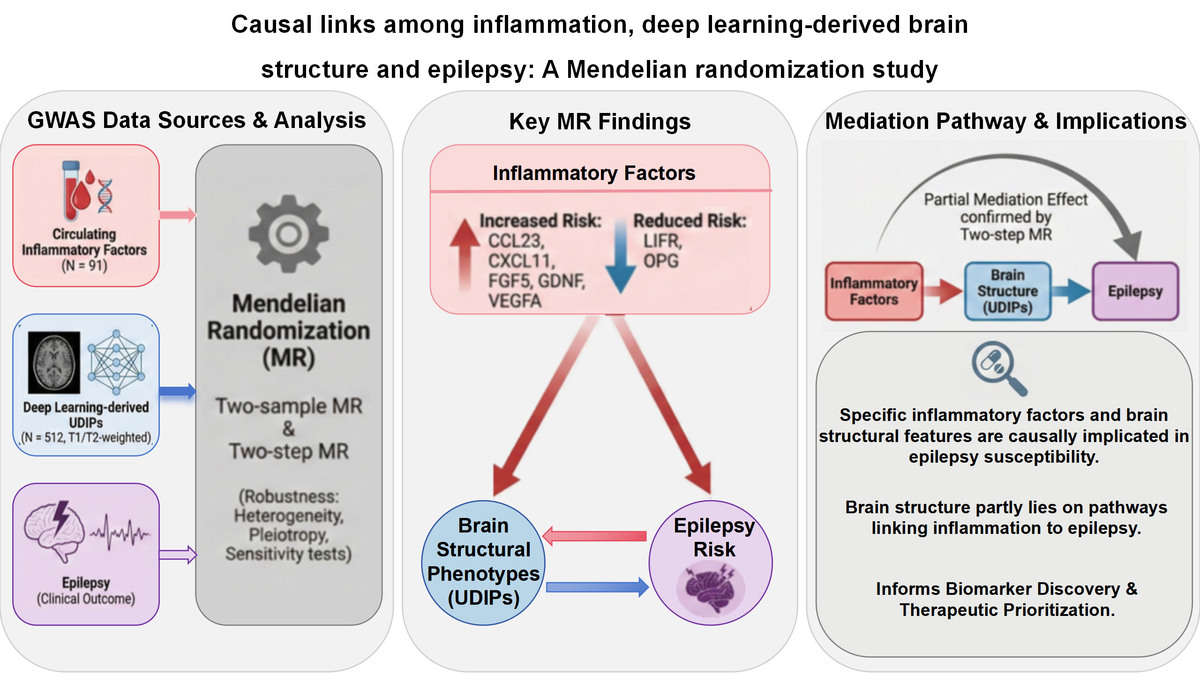
We leveraged genome-wide association study (GWAS) summary statistics for 512 UDIPs derived from whole-brain MRI, 91 circulating inflammatory factors, and epilepsy. Two-sample MR was used to systematically estimate: (i) the effects of inflammatory factors on epilepsy, (ii) the effects of inflammatory factors on UDIPs, and (iii) the effects of UDIPs on epilepsy. We further applied two-step MR to explore whether UDIPs may mediate the effects of inflammatory factors on epilepsy. Robustness was assessed using heterogeneity tests, pleiotropy evaluation, and sensitivity analyses.
Results:
Several inflammatory factors showed significant associations with epilepsy risk. Genetically predicted higher levels of CCL23, CXCL11, FGF5, GDNF, and VEGFA were associated with increased epilepsy risk, whereas higher LIFR and OPG were associated with reduced risk. MR analyses also identified multiple T1- and T2-weighted UDIP dimensions associated with epilepsy in opposite directions, indicating heterogeneous structural signatures linked to epilepsy liability (e.g., T1 dimension 76 showed a positive association, while other dimensions were inversely associated). Two-step MR suggested that, for selected pathways, UDIPs may account for part of the association between inflammatory factors and epilepsy, consistent with partial mediation. These findings were broadly consistent across heterogeneity, pleiotropy, and sensitivity analyses.
Conclusions:
These findings implicate specific inflammatory factors and MRI-derived structural phenotypes in epilepsy susceptibility and suggest that brain structural features may partly lie on pathways linking inflammation to epilepsy, informing biomarker discovery and therapeutic prioritization.
To evaluate potential causal links among circulating inflammatory factors, deep learning–derived brain structural phenotypes (unimodal deep imaging phenotypes, UDIPs), and epilepsy using Mendelian randomization (MR).
Material and methods:
We leveraged genome-wide association study (GWAS) summary statistics for 512 UDIPs derived from whole-brain MRI, 91 circulating inflammatory factors, and epilepsy. Two-sample MR was used to systematically estimate: (i) the effects of inflammatory factors on epilepsy, (ii) the effects of inflammatory factors on UDIPs, and (iii) the effects of UDIPs on epilepsy. We further applied two-step MR to explore whether UDIPs may mediate the effects of inflammatory factors on epilepsy. Robustness was assessed using heterogeneity tests, pleiotropy evaluation, and sensitivity analyses.
Results:
Several inflammatory factors showed significant associations with epilepsy risk. Genetically predicted higher levels of CCL23, CXCL11, FGF5, GDNF, and VEGFA were associated with increased epilepsy risk, whereas higher LIFR and OPG were associated with reduced risk. MR analyses also identified multiple T1- and T2-weighted UDIP dimensions associated with epilepsy in opposite directions, indicating heterogeneous structural signatures linked to epilepsy liability (e.g., T1 dimension 76 showed a positive association, while other dimensions were inversely associated). Two-step MR suggested that, for selected pathways, UDIPs may account for part of the association between inflammatory factors and epilepsy, consistent with partial mediation. These findings were broadly consistent across heterogeneity, pleiotropy, and sensitivity analyses.
Conclusions:
These findings implicate specific inflammatory factors and MRI-derived structural phenotypes in epilepsy susceptibility and suggest that brain structural features may partly lie on pathways linking inflammation to epilepsy, informing biomarker discovery and therapeutic prioritization.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.