Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
Editor's Choice
CARDIO-ONCOLOGY / CLINICAL RESEARCH
Global co-occurrence patterns of cancer and cardiovascular disease: a comprehensive analysis based on the Global Burden of Disease Study 2021
1
Department of Cardiology, Shanghai Ninth People’s Hospital School of Medicine, Shanghai Jiaotong University, Shanghai, China
2
Department of Cardiology, The First Affiliated Hospital of USTC, Division of Life Sciences and Medicine, University of Science and Technology of China
Submission date: 2025-10-26
Final revision date: 2025-12-09
Acceptance date: 2026-01-05
Online publication date: 2026-04-03
Publication date: 2026-04-30
Corresponding author
Jun Gu
Department of Cardiology Shanghai Ninth People’s Hospital Shanghai Jiaotong University School of Medicine Shanghai, 200001, China
Department of Cardiology Shanghai Ninth People’s Hospital Shanghai Jiaotong University School of Medicine Shanghai, 200001, China
Arch Med Sci 2026;22(2):760-781
KEYWORDS
cardiovascular diseasesneoplasmsdisease burdendisability-adjusted life yearsrisk factorsepidemiological transition
TOPICS
ABSTRACT
Introduction:
Cardiovascular disease (CVD) and neoplasms are the two leading causes of death worldwide. Previous research has predominantly addressed these conditions separately or focused on specific regions. We aimed to characterize the global co-occurrence pattern of CVD and neoplasms from spatial and temporal perspectives and identify corresponding risk factors across different epidemiological contexts.
Material and methods:
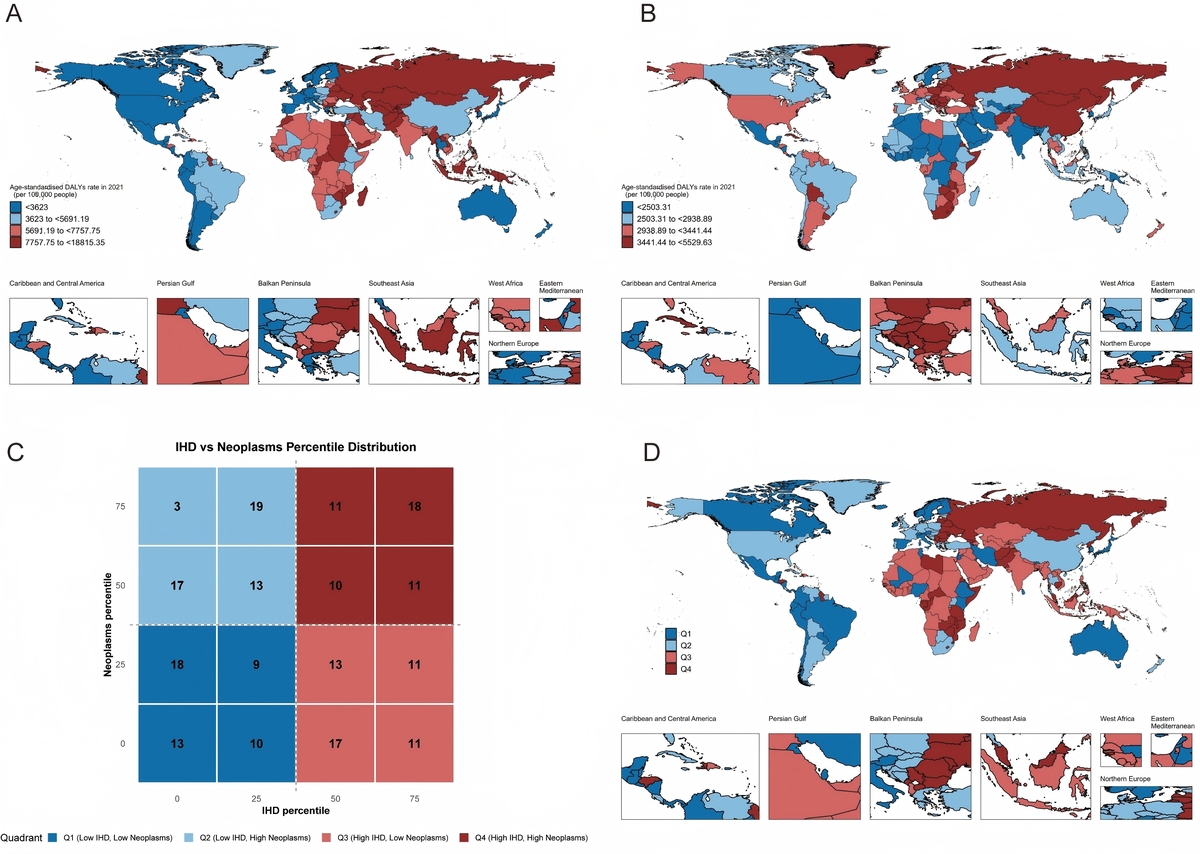
Using GBD 2021 data, we extracted age-standardized disability-adjusted life year (DALY) rates of CVD and neoplasms and modifiable risk factor exposure from 204 countries and territories (1990–2021). We identified four epidemiological patterns: low- burden, neoplasm-dominant, CVD-dominant, and dual-burden regions. We calculated population attributable fractions (PAF) and integrated machine learning with SHAP values to distinguish intervention priorities. Average annual percentage changes (AAPC) were used to evaluate temporal trends.
Results:
Each pattern comprised 50–52 countries. Spatial distribution overlapped with socioeconomic development stages and risk factor exposure. Temporal analysis revealed widening global inequality: low-burden regions achieved 3–4% annual reductions while dual-burden regions experienced an increasing burden, creating a 5.8 percentage point gap. High systolic blood pressure was the universal dominant CVD risk factor, accounting for 49.7% of the global burden (49.2–52.4% across patterns). For neoplasms, smoking contributed 18.5% globally but varied dramatically by pattern (10.4–23.4%). Modifiable risk factors’ specific combinations greatly influenced global disparities.
Conclusions:
The co-occurrence of CVD and neoplasms represents interconnected manifestations of different epidemiological transition stages, with concerning divergence between regions. Interventions targeting hypertension control and tobacco cessation, combined with pattern-specific strategies, can fundamentally reduce the global disease burden.
Cardiovascular disease (CVD) and neoplasms are the two leading causes of death worldwide. Previous research has predominantly addressed these conditions separately or focused on specific regions. We aimed to characterize the global co-occurrence pattern of CVD and neoplasms from spatial and temporal perspectives and identify corresponding risk factors across different epidemiological contexts.
Material and methods:
Using GBD 2021 data, we extracted age-standardized disability-adjusted life year (DALY) rates of CVD and neoplasms and modifiable risk factor exposure from 204 countries and territories (1990–2021). We identified four epidemiological patterns: low- burden, neoplasm-dominant, CVD-dominant, and dual-burden regions. We calculated population attributable fractions (PAF) and integrated machine learning with SHAP values to distinguish intervention priorities. Average annual percentage changes (AAPC) were used to evaluate temporal trends.
Results:
Each pattern comprised 50–52 countries. Spatial distribution overlapped with socioeconomic development stages and risk factor exposure. Temporal analysis revealed widening global inequality: low-burden regions achieved 3–4% annual reductions while dual-burden regions experienced an increasing burden, creating a 5.8 percentage point gap. High systolic blood pressure was the universal dominant CVD risk factor, accounting for 49.7% of the global burden (49.2–52.4% across patterns). For neoplasms, smoking contributed 18.5% globally but varied dramatically by pattern (10.4–23.4%). Modifiable risk factors’ specific combinations greatly influenced global disparities.
Conclusions:
The co-occurrence of CVD and neoplasms represents interconnected manifestations of different epidemiological transition stages, with concerning divergence between regions. Interventions targeting hypertension control and tobacco cessation, combined with pattern-specific strategies, can fundamentally reduce the global disease burden.
REFERENCES (59)
1.
Force LM, Kocarnik JM, May ML, et al. The Global, Regional, and National Burden of Cancer, 19902023, with Forecasts to 2050: a systematic analysis for the Global Burden of Disease Study 2023. Lancet 2025; 406: 1565-86.
2.
Weisz G, Olszynko-Gryn J. The theory of epidemiologic transition: the origins of a citation classic. J Hist Med Allied Sci 2010; 65: 287-326.
3.
Huicho L, Trelles M, Gonzales F, et al. Mortality profiles in a country facing epidemiological transition: an analysis of registered data. BMC Public Health 2009; 9: 47.
4.
Lippi G, Mattiuzzi C. The Global Burden of Pancreatic Cancer. Arch Med Sci 2020; 16: 820-4.
5.
Koene RJ, Prizment AE, Blaes A, et al. Shared risk factors in cardiovascular disease and cancer. Circulation 2016; 133: 1104-14.
6.
Vincent L, Leedy D, Masri SC, et al. Cardiovascular disease and cancer: is there increasing overlap? Curr Oncol Rep 2019; 21: 47.
7.
Kojic A, Moslehi J, Ky B, et al. Cardiometabolic disease and cardio-oncology: insights from iPSC models and tissue engineering. Cell Rep Med 2025; 6: 102261.
8.
Gue YX, Lau D, Shantsila A, et al. Cardiovascular and metabolic effects of ovarian suppression in combination with tamoxifen or an aromatase inhibitor as adjuvant therapy for early oestrogen receptor-positive breast cancer: a systematic review. Arch Med Sci 2024; 21: 577-87.
9.
Targher G, Byrne CD, Tilg H. MASLD: a systemic metabolic disorder with cardiovascular and malignant complications. Gut 2024; 73: 691-702.
10.
Wang T, Masedunskas A, Willett WC, et al. Vegetarian and vegan diets: benefits and drawbacks. Eur Heart J 2023; 44: 3423-39.
11.
Zhang S, Liu L, Shi S, et al. Bidirectional association between cardiovascular disease and lung cancer in a prospective cohort study. J Thorac Oncol 2024; 19: 80-93.
12.
Kuwabara M. The interplay between cancer and cardiovascular disease. Hypertens Res 2025; 48: 1192-4.
13.
Chong B, Jayabaskaran J, Jauhari SM, et al. Global Burden of Cardiovascular Diseases: projections from 2025 to 2050. Eur J Prev Cardiol 2025; 32: 1001-15.
14.
Wu Z, Xia F, Lin R. Global burden of cancer and associated risk factors in 204 countries and territories, 1980 -2021: a systematic analysis for the GBD 2021. J Hematol Oncol 2024; 17: 119.
15.
Waters WF. Globalization, socioeconomic restructuring, and community health. J Commun Health 2001; 26: 79-92.
16.
Meghji J, Mortimer K, Agusti A, et al. Improving lung health in low-income and middle-income countries: from challenges to solutions. Lancet 2021; 397: 928-40.
17.
Mendenhall E, Kohrt BA, Norris SA, et al. Non-communicable disease syndemics: poverty, depression, and diabetes among low-income populations. Lancet 2017; 389: 951-63.
18.
Ngiam KY, Khor IW. Big data and machine learning algorithms for health-care delivery. Lancet Oncol 2019; 20: e262-73.
19.
Si Z, Ying J, Zhou Y. A study on the global burden of non-melanoma skin cancer from 1990 to 2019. Arch Med Sci 2024; 20: 1902-8.
20.
Murray CJL. Findings from the Global Burden of Disease Study 2021. Lancet 2024; 403: 2259-62.
21.
Murray CJL. The Global Burden of Disease Study at 30 years. Nat Med 2022; 28: 2019-26.
22.
Rudd KE, Johnson SC, Agesa KM, et al. Global, regional, and national sepsis incidence and mortality, 1990-2017: analysis for the Global Burden of Disease Study. Lancet 2020; 395: 200-11.
23.
Roth GA, Mensah GA, Johnson CO, et al. Global burden of cardiovascular diseases and risk factors, 1990-2019: update from the GBD 2019 Study. J Am Coll Cardiol 2020; 76: 2982-3021.
24.
Bender RG, Sirota SB, Swetschinski LR, et al. Global, regional, and national incidence and mortality burden of non-Covid-19 lower respiratory infections and aetiologies, 1990-2021: a systematic analysis from the Global Burden of Disease Study 2021. Lancet Infect Dis 2024; 24: 974-1002.
25.
Liang D, Wang L, Zhong P, et al. Perspective: global burden of iodine deficiency: insights and projections to 2050 using XGBoost and SHAP. Adv Nutr 2025; 16: 100384.
26.
Qi X, Wang S, Fang C, et al. Machine learning and SHAP value interpretation for predicting comorbidity of cardiovascular disease and cancer with dietary antioxidants. Redox Biol 2025; 79: 103470.
27.
Su L, Liu S, Yang Y, et al. Positive fluid balance and poor outcomes after initial intensive care unit admission in sepsis resuscitation: a retrospective study. Arch Med Sci 2024; 20: 464-75.
28.
Wu Z, Xia F, Lin R. Global burden of cancer and associated risk factors in 204 countries and territories, 1980-2021: a systematic analysis for the GBD 2021. J Hematol Oncol 2024; 17: 119.
29.
Sturgeon KM, Deng L, Bluethmann SM, et al. A population-based study of cardiovascular disease mortality risk in US cancer patients. Eur Heart J 2019; 40: 3889-97.
30.
Nowakowska M, Płońska-Gościniak E, Szyszka A, et al. Cardiovascular risk factors among cancer patients qualified for systemic treatment. Analysis of a cardiovascular disease-free cohort from the Polish Multicentre Study ONCOECHO. Arch Med Sci 2020; 16: 1295-303.
31.
Roth GA, Mensah GA, Johnson CO, et al. Global burden of cardiovascular diseases and risk factors, 1990-2019. JACC 2020; 76: 2982-3021.
32.
GBD 2019 Respiratory Tract Cancers Collaborators. Global, regional, and national burden of respiratory tract cancers and associated risk factors from 1990 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet Respir Med 2021; 9: 1030-49.
33.
Global Burden of Disease 2019 Cancer Collaboration. Cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life years for 29 cancer groups from 2010 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. JAMA Oncol 2022; 8: 420-44.
34.
Lundberg FE, Andersson TML, Lambe M, et al. Trends in cancer survival in the nordic countries 1990-2016: the NORDCAN survival studies. Acta Oncol 2020; 59: 1266-74.
35.
Hardman R, Begg S, Spelten E. What impact do chronic disease self-management support interventions have on health inequity gaps related to socioeconomic status: a systematic review. BMC Health Serv Res 2020; 20: 150.
36.
Schultz WM, Kelli HM, Lisko JC, et al. Socioeconomic status and cardiovascular outcomes. Circulation 2018; 137: 2166-78.
37.
Vollset SE, Ababneh HS, Abate YH, et al. Burden of disease scenarios for 204 countries and territories, 2022-2050: a forecasting analysis for the Global Burden of Disease Study 2021. Lancet 2024; 403: 2204-56.
38.
Shippee TP, Akosionu O, Ng W, et al. COVID-19 pandemic: exacerbating racial/ethnic disparities in long-term services and supports. J Aging Soc Policy 2020; 32: 323-33.
39.
Perry BL, Aronson B, Pescosolido BA. Pandemic precarity: COVID-19 is exposing and exacerbating inequalities in the American Heartland. Proc Natl Acad Sci USA 2021; 118: e2020685118.
40.
Pazoki R, Dehghan A, Evangelou E, et al. Genetic predisposition to high blood pressure and lifestyle factors: associations with midlife blood pressure levels and cardiovascular events. Circulation 2018; 137: 653-61.
41.
Fuchs FD, Whelton PK. High blood pressure and cardiovascular disease. Hypertension 2020; 75: 285-92.
42.
Yusuf S, Joseph P, Rangarajan S, et al. Modifiable risk factors, cardiovascular disease, and mortality in 155 722 individuals from 21 high-income, middle-income, and low-income countries (PURE): a prospective cohort study. Lancet 2020; 395: 795-808.
43.
Lopez-Jaramillo P, Gomez-Arbelaez D, Martinez-Bello D, et al. Association of the triglyceride glucose index as a measure of insulin resistance with mortality and cardiovascular disease in populations from five continents (PURE Study): a prospective cohort study. Lancet Healthy Longev 2023; 4: e23-33.
44.
Raza SA, Salemi JL, Zoorob RJ. Historical perspectives on prevention paradox: when the population moves as a whole. J Family Med Prim Care 2018; 7: 1163-5.
45.
Yamamoto SS, Phalkey R, Malik AA. A systematic review of air pollution as a risk factor for cardiovascular disease in South Asia: limited evidence from India and Pakistan. Int J Hyg Environ Health 2014; 217: 133-44.
46.
Macchi C, Sirtori CR, Corsini A, et al. Pollution from fine particulate matter and atherosclerosis: a narrative review. Environ Int 2023; 175: 107923.
47.
Puzzolo E, Zerriffi H, Carter E, et al. Supply considerations for scaling up clean cooking fuels for household energy in low- and middle-income countries. Geohealth 2019; 3: 370-90.
48.
Thun M, Peto R, Boreham J, et al. Stages of the cigarette epidemic on entering its second century. Tob Control 2012; 21: 96-101.
49.
Kulhánová I, Forman D, Vignat J, et al. Tobacco-related cancers in Europe: the scale of the epidemic in 2018. Eur J Cancer 2020; 139: 27-36.
50.
Jiang X, Jackson LJ, Syed MA, et al. Economic evaluations of tobacco control interventions in low- and middle-income countries: a systematic review. Addiction 2022; 117: 2374-92.
51.
Simmons VN, Gray JE. From success to sustained action: tobacco control must remain a priority. CA Cancer J Clin 2025; 75: 180-2.
52.
Adolph TE, Tilg H. Western diets and chronic diseases. Nat Med 2024; 30: 2133-47.
53.
Haas AD, Radin E, Hakim AJ, et al. Prevalence of nonsuppressed viral load and associated factors among HIV-positive adults receiving antiretroviral therapy in Eswatini, Lesotho, Malawi, Zambia and Zimbabwe (2015 to 2017): results from population-based nationally representative surveys. J Int AIDS Soc 2020; 23: e25631.
54.
Teasdale CA, Zimba R, Abrams EJ, et al. Estimates of the prevalence of undiagnosed HIV among children living with HIV in Eswatini, Lesotho, Malawi, Namibia, Tanzania, Zambia, and Zimbabwe from 2015 to 2017: an analysis of data from the cross-sectional population-based HIV impact assessment surveys. Lancet HIV 2022; 9: e91-101.
55.
Teasdale CA, Zimba R, Low A, et al. Evidence from two rounds of population hiv impact assessments of progress towards HIV epidemic control in adolescents aged 15-19 years in Eswatini, Lesotho, Malawi, and Zimbabwe: a cross-sectional study. Lancet Glob Health 2025; 13: e1221-9.
56.
GBD 2017 Diet Collaborators. Health effects of dietary risks in 195 countries, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 2019; 393: 1958-72.
57.
Lyon AR, López-Fernández T, Couch LS, et al. 2022 ESC Guidelines on Cardio-Oncology Developed in Collaboration with the European Hematology Association (EHA), the European Society for Therapeutic Radiology and Oncology (ESTRO) and the International Cardio-Oncology Society (IC-OS). Eur Heart J 2022; 43: 4229-361.
58.
Hosseinpoor AR, Victora CG, Bergen N, et al. Towards universal health coverage: the role of within-country wealth-related inequality in 28 countries in Sub-Saharan Africa. Bull World Health Organ 2011; 89: 881-90.
59.
Bendavid E, Littleton AKS, Mejía-Guevara I, et al. A global analysis of within- country health inequalities. JAMA Health Forum 2025; 6: e253611.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.