Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
Editor's Choice
PULMONOLOGY / CLINICAL RESEARCH
Global, regional, and national burden of respiratory diseases and attributable risk factors in adolescents and young adults, 1990–2021: a Global Burden of Disease 2021 analysis
1
Department of Respiratory and Critical Care Medicine, West China Hospital, Sichuan University, Chengdu, Sichuan Province, China
2
State Key Laboratory of Respiratory Health and Multimorbidity, West China Hospital, Sichuan University, Chengdu, China
These authors had equal contribution to this work
Submission date: 2026-01-08
Final revision date: 2026-03-15
Acceptance date: 2026-04-05
Online publication date: 2026-04-27
Publication date: 2026-04-30
Corresponding author
Jian-Qing He
Department of Pulmonary and Critical Care Medicine West China Hospital Sichuan University Guo-xue-xiang 37# Wuhou District Chengdu 610041 Sichuan Province, China Phone: +86 28 18980602293.
Department of Pulmonary and Critical Care Medicine West China Hospital Sichuan University Guo-xue-xiang 37# Wuhou District Chengdu 610041 Sichuan Province, China Phone: +86 28 18980602293.
Arch Med Sci 2026;22(2):857-870
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Respiratory diseases impose a substantial global burden on adolescents and young adults (AYAs, aged 15–39 years), yet this population remains undercharacterized.
Material and methods:
Using Global Burden of Disease 2021 data, we assessed incidence, mortality, DALYs, and attributable risk factors for respiratory diseases among AYAs across 204 countries and territories. Estimates were stratified by age, sex, location, and sociodemographic index (SDI). Temporal trends were evaluated using estimated annual percentage change (EAPC), and associations with development were analyzed via LOESS regression (span = 0.5).
Results:
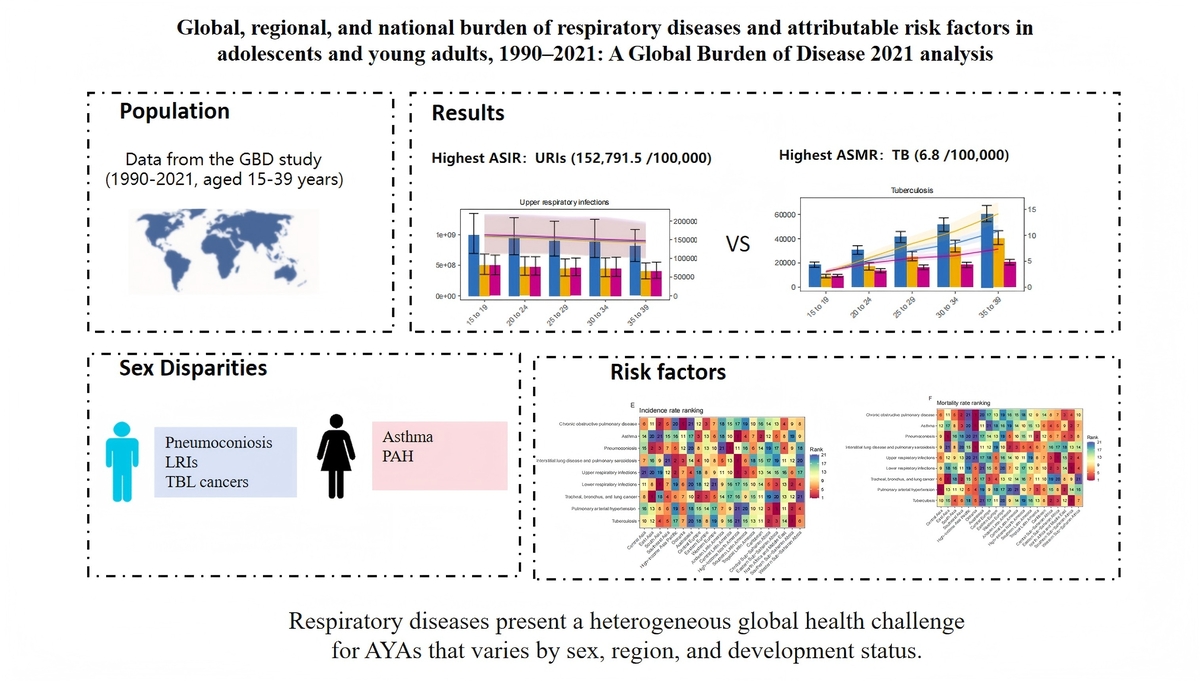
In 2021, upper respiratory infections had the highest age-standardized incidence rate (152,791.5/100,000), while tuberculosis caused the highest age-standardized mortality rate (6.8/100,000). Air pollution was the leading risk factor, contributing to 32.76 age-standardized DALYs per 100,000 for chronic obstructive pulmonary disease (COPD) and 62.37 for lower respiratory infections (LRIs). Sex-based disparities were evident: males had higher burdens of pneumoconiosis, LRIs, and tracheal/bronchus/lung cancers, whereas asthma and pulmonary arterial hypertension were more prevalent in females. Regionally, low-SDI areas bore the greatest burden for TB and LRIs, while high-SDI regions had higher rates of URIs and asthma. Smoking was the primary driver of COPD burden specifically in high-income countries.
Conclusions:
Respiratory diseases present a heterogeneous global health challenge for AYAs that varies by sex, region, and development status. These findings support targeted strategies: control of infectious disease and air quality improvement in low-SDI regions where TB and LRIs predominate, alongside enhanced asthma management and tobacco control in high-income areas where URIs and smoking-related COPD burden are more prevalent.
Respiratory diseases impose a substantial global burden on adolescents and young adults (AYAs, aged 15–39 years), yet this population remains undercharacterized.
Material and methods:
Using Global Burden of Disease 2021 data, we assessed incidence, mortality, DALYs, and attributable risk factors for respiratory diseases among AYAs across 204 countries and territories. Estimates were stratified by age, sex, location, and sociodemographic index (SDI). Temporal trends were evaluated using estimated annual percentage change (EAPC), and associations with development were analyzed via LOESS regression (span = 0.5).
Results:
In 2021, upper respiratory infections had the highest age-standardized incidence rate (152,791.5/100,000), while tuberculosis caused the highest age-standardized mortality rate (6.8/100,000). Air pollution was the leading risk factor, contributing to 32.76 age-standardized DALYs per 100,000 for chronic obstructive pulmonary disease (COPD) and 62.37 for lower respiratory infections (LRIs). Sex-based disparities were evident: males had higher burdens of pneumoconiosis, LRIs, and tracheal/bronchus/lung cancers, whereas asthma and pulmonary arterial hypertension were more prevalent in females. Regionally, low-SDI areas bore the greatest burden for TB and LRIs, while high-SDI regions had higher rates of URIs and asthma. Smoking was the primary driver of COPD burden specifically in high-income countries.
Conclusions:
Respiratory diseases present a heterogeneous global health challenge for AYAs that varies by sex, region, and development status. These findings support targeted strategies: control of infectious disease and air quality improvement in low-SDI regions where TB and LRIs predominate, alongside enhanced asthma management and tobacco control in high-income areas where URIs and smoking-related COPD burden are more prevalent.
REFERENCES (40)
1.
GBD 2021 Demographics Collaborators. Global age-sex-specific mortality, life expectancy, and population estimates in 204 countries and territories and 811 subnational locations, 1950-2021, and the impact of the COVID-19 pandemic: a comprehensive demographic analysis for the Global Burden of Disease Study 2021. Lancet 2024; 403: 1989-2056.
2.
GBD 2019 Chronic Respiratory Diseases Collaborators. Global burden of chronic respiratory diseases and risk factors, 1990-2019: an update from the Global Burden of Disease Study 2019. EClinicalMedicine 2023; 59: 101936.
3.
GBD 2021 Lower Respiratory Infections and Antimicrobial Resistance Collaborators. Global, regional, and national incidence and mortality burden of non-COVID-19 lower respiratory infections and aetiologies, 1990-2021: a systematic analysis from the Global Burden of Disease Study 2021. Lancet Infect Dis 2024; 24: 974-1002.
4.
Bae J, Lee HJ, Choi KY, et al. Risk factors of acute exacerbation and disease progression in young patients with COPD. BMJ Open Respir Res 2024; 11: e001740.
5.
Wang L, Chen J, Leung LT, et al. Characterization of respiratory symptoms among youth using heated tobacco products in Hong Kong. JAMA Netw Open 2021; 4: e2117055.
6.
Oyenuga VO, Mosler G, Addo-Yobo E, et al. Asthma symptoms, severity, and control with and without a clinical diagnosis of asthma in early adolescence in sub-Saharan Africa: a multi-country, school-based, cross-sectional study. Lancet Child Adolesc Health 2024; 8: 859-71.
7.
Lovie-Toon YG, Grimwood K, Byrnes CA, et al. Health-resource use and quality of life in children with bronchiectasis: a multi-center pilot cohort study. BMC Health Serv Res 2019; 19: 561.
8.
GBD 2019 Adolescent Mortality Collaborators. Global, regional, and national mortality among young people aged 10-24 years, 1950-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 2021; 398: 1593-618.
9.
Yu S, Yang L, Xu W, et al. Analysis of tracheal, bronchial, and lung cancer attributable to respiratory system-related risk factors in 204 countries and territories from 1990 to 2019. Arch Med Sci 2024; 20: 1495-503.
10.
GBD 2019 Diseases and Injuries Collaborators. Global burden of 369 diseases and injuries in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 2020; 396: 1204-22.
11.
GBD 2021 Risk Factors Collaborators. Global burden and strength of evidence for 88 risk factors in 204 countries and 811 subnational locations, 1990-2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet 2024; 403: 2162-203.
12.
Xie J, Wang M, Long Z, et al. Global burden of type 2 diabetes in adolescents and young adults, 1990-2019: systematic analysis of the Global Burden of Disease Study 2019. BMJ 2022; 379: e072385.
13.
GBD 2019 Risk Factors Collaborators. Global burden of 87 risk factors in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 2020; 396: 1223-49.
14.
GBD 2019 Demographics Collaborators. Global age-sex-specific fertility, mortality, healthy life expectancy (HALE), and population estimates in 204 countries and territories, 1950-2019: a comprehensive demographic analysis for the Global Burden of Disease Study 2019. Lancet 2020; 396: 1160-203.
15.
Gao S, Yang WS, Bray F, et al. Declining rates of hepatocellular carcinoma in urban Shanghai: incidence trends in 1976-2005. Eur J Epidemiol 2012; 27: 39-46.
16.
Lv B, Song G, Jing F, et al. Mortality from cerebrovascular diseases in China: Exploration of recent and future trends. Chin Med J (Engl) 2024; 137: 588-95.
17.
Tobin EH, Thomas M, Bomar PA. Upper Respiratory Tract Infections With Focus on The Common Cold. StatPearls. Treasure Island (FL): StatPearls Publishing Copyright © 2025, StatPearls Publishing LLC. 2025.
18.
Kutter JS, Spronken MI, Fraaij PL, et al. Transmission routes of respiratory viruses among humans. Curr Opin Virol 2018; 28: 142-51.
19.
Davies LRL, Wang C, Steigler P, et al. Age and sex influence antibody profiles associated with tuberculosis progression. Nat Microbiol 2024; 9: 1513-25.
20.
Dhakulkar S, Das M, Sutar N, et al. Treatment outcomes of children and adolescents receiving drug-resistant TB treatment in a routine TB programme, Mumbai, India. PLoS One 2021; 16: e0246639.
21.
Snow KJ, Sawyer SM, Denholm JT, et al. Explaining variation in the burden of child and adolescent tuberculosis. Eur Respir J 2019; 53: 1901007.
22.
Mathad JS, Gupta A. Tuberculosis in pregnant and postpartum women: epidemiology, management, and research gaps. Clin Infect Dis 2012; 55: 1532-49.
23.
Baumgartner KB, Samet JM, Stidley CA, et al. Cigarette smoking: a risk factor for idiopathic pulmonary fibrosis. Am J Respir Crit Care Med 1997; 155: 242-8.
24.
Poinen-Rughooputh S, Rughooputh MS, Guo Y, et al. Sex-related differences in the risk of silicosis among chinese pottery workers a cohort study. J Occup Environ Med 2021; 63: 74-9.
25.
Ridolo E, Incorvaia C, Martignago I, et al. Sex in respiratory and skin allergies. Clin Rev Allergy Immunol 2019; 56: 322-32.
26.
Ventetuolo CE, Praestgaard A, Palevsky HI, et al. Sex and haemodynamics in pulmonary arterial hypertension. Eur Respir J 2014; 43: 523-30.
27.
Zou J, Sun T, Song X, et al. Distributions and trends of the global burden of COPD attributable to risk factors by SDI, age, and sex from 1990 to 2019: a systematic analysis of GBD 2019 data. Respir Res 2022; 23: 90.
28.
Minelli C, van der Plaat DA, Leynaert B, et al. Age at puberty and risk of asthma: a Mendelian randomisation study. PLoS Med 2018; 15: e1002634.
29.
Wang Z, Li Y, Gao Y, et al. Global, regional, and national burden of asthma and its attributable risk factors from 1990 to 2019: a systematic analysis for the Global Burden of Disease Study 2019. Respir Res 2023; 24: 169.
30.
Bishwajit G, Tang S, Yaya S, et al. Burden of asthma, dyspnea, and chronic cough in South Asia. Int J Chron Obstruct Pulmon Dis 2017; 12: 1093-9.
31.
Ozoh OB, Aderibigbe SA, Ayuk AC, et al. The prevalence of asthma and allergic rhinitis in Nigeria: a nationwide survey among children, adolescents and adults. PLoS One 2019; 14: e0222281.
32.
Obaseki DO, Erhabor GE, Gnatiuc L, et al. Chronic airflow obstruction in a black african population: results of BOLD Study, Ile-Ife, Nigeria. Copd 2016; 13: 42-9.
33.
Ji W, Chen Y, Huang W, et al. Trends and regional disparities in the global burden of disease attributable to household air pollution in 204 countries and territories, 1990-2021: an analysis of the global burden of disease study. BMJ Open 2025; 15: e092162.
34.
Meghji J, Mortimer K, Agusti A, et al. Improving lung health in low-income and middle-income countries: from challenges to solutions. Lancet 2021; 397: 928-40.
35.
Jin X, Ren J, Li R, et al. Global burden of upper respiratory infections in 204 countries and territories, from 1990 to 2019. EClinicalMedicine 2021; 37: 100986.
36.
Stenius-Aarniala B, Poussa T, Kvarnström J, et al. Immediate and long term effects of weight reduction in obese people with asthma: randomised controlled study. BMJ 2000; 320: 827-32.
37.
Wu Y, Song P, Lin S, et al. Global burden of respiratory diseases attributable to ambient particulate matter pollution: findings from the Global Burden of Disease Study 2019. Front Public Health 2021; 9: 740800.
38.
Hystad P, Larkin A, Rangarajan S, et al. Associations of outdoor fine particulate air pollution and cardiovascular disease in 157 436 individuals from 21 high-income, middle-income, and low-income countries (PURE): a prospective cohort study. Lancet Planet Health 2020; 4: e235-45.
39.
WHO global report on trends in prevalence of tobacco smoking 2000-2025 [Available from: https://www.who.int/publicatio....
40.
WHO. Adolescent-friendly health services: What health workers can do [Available from: https://www.who.int/health-top....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.