Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
CLINICAL RESEARCH
Multifactorial analysis of postoperative pain following silicone breast augmentation: patient- and
procedure-related predictors
1
The Student Scientific Society, Poznan University of Medical Sciences, Poznan, Poland
2
Department of Practical Midwifery Education, Poznan University of Medical Science, Poznan, Poland
3
Zlotowska Plastic Surgery Clinic, Poznan, Poland
4
Department of Mother’s and Child’s Health, Poznan University of Medical Science, Poznan, Poland
Submission date: 2025-12-18
Final revision date: 2026-01-19
Acceptance date: 2026-02-26
Online publication date: 2026-04-22
Corresponding author
KEYWORDS
painVASimplantsbreastpostoperative painbreast augmentationvisual analogue scaleesthetic surgerypain predictors
TOPICS
ABSTRACT
Introduction:
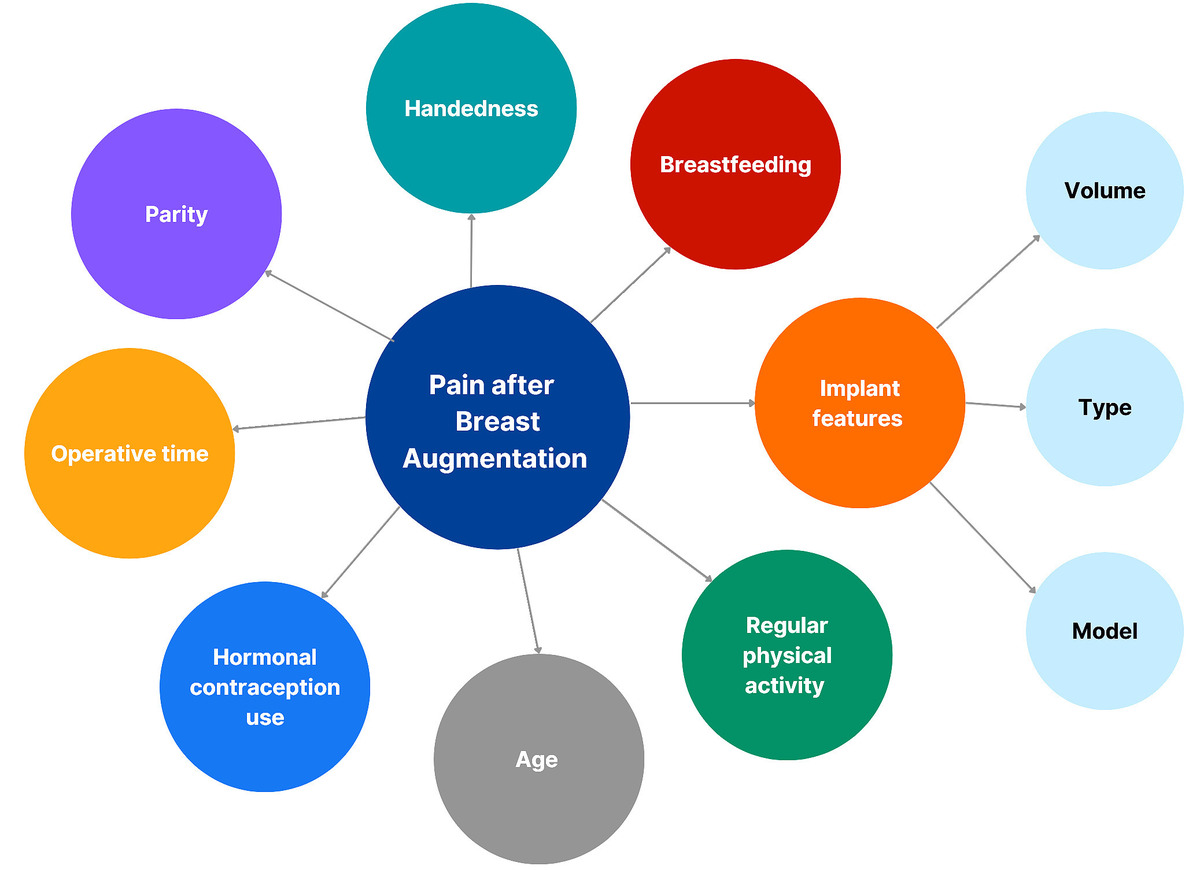
Postoperative pain after silicone breast augmentation is influenced by multiple patient- and procedure-related factors, yet limited research has directly evaluated these variables. Understanding predictors of pain may improve analgesic strategies and patient outcomes. The aim of this study was to identify patient- and procedure-related predictors of postoperative pain following elective silicone breast augmentation.
Material and methods:
This prospective study enrolled 35 women undergoing elective breast augmentation with silicone gel-filled implants; 28 completed the 14-day protocol. Preoperative questionnaires collected data on age, parity, breastfeeding duration, handedness, hormonal contraception use, satisfaction, and physical activity. Implant characteristics (type, shape, volume) and operative parameters were also analyzed. Patients recorded daily pain for each breast using a 10 cm visual analogue scale (VAS).
Results:
Mean VAS pain scores decreased from 79 mm on postoperative day 1 to below 15 mm by day 7, remaining near zero thereafter. Larger implant volume was associated with slightly lower pain on days 1–3. Age negatively correlated with pain on days 13–14. No significant associations were observed with parity, breastfeeding duration, hormonal contraception, physical activity (except day 11), surgical duration, or handedness. Anatomical implants were initially associated with higher early pain scores compared with round implants, but mean pain at day 14 did not differ according to implant type, shape, or height profile.
Conclusions:
Postoperative pain following breast augmentation is multifactorial. Most patient- and procedure-related variables, including implant type and model, had a limited long-term impact. Detailed pain monitoring may guide individualized analgesic strategies, optimize perioperative care, and support opioid-sparing approaches.
Postoperative pain after silicone breast augmentation is influenced by multiple patient- and procedure-related factors, yet limited research has directly evaluated these variables. Understanding predictors of pain may improve analgesic strategies and patient outcomes. The aim of this study was to identify patient- and procedure-related predictors of postoperative pain following elective silicone breast augmentation.
Material and methods:
This prospective study enrolled 35 women undergoing elective breast augmentation with silicone gel-filled implants; 28 completed the 14-day protocol. Preoperative questionnaires collected data on age, parity, breastfeeding duration, handedness, hormonal contraception use, satisfaction, and physical activity. Implant characteristics (type, shape, volume) and operative parameters were also analyzed. Patients recorded daily pain for each breast using a 10 cm visual analogue scale (VAS).
Results:
Mean VAS pain scores decreased from 79 mm on postoperative day 1 to below 15 mm by day 7, remaining near zero thereafter. Larger implant volume was associated with slightly lower pain on days 1–3. Age negatively correlated with pain on days 13–14. No significant associations were observed with parity, breastfeeding duration, hormonal contraception, physical activity (except day 11), surgical duration, or handedness. Anatomical implants were initially associated with higher early pain scores compared with round implants, but mean pain at day 14 did not differ according to implant type, shape, or height profile.
Conclusions:
Postoperative pain following breast augmentation is multifactorial. Most patient- and procedure-related variables, including implant type and model, had a limited long-term impact. Detailed pain monitoring may guide individualized analgesic strategies, optimize perioperative care, and support opioid-sparing approaches.
REFERENCES (59)
1.
Triana L, Palacios Huatuco RM, Campilgio G, Liscano E. Trends in surgical and nonsurgical aesthetic procedures: a 14-year analysis of the international society of aesthetic plastic surgery – ISAPS. Aesth Plast Surg 2024; 48: 4217-27.
2.
Kehlet H, Jensen TS, Woolf CJ. Persistent postsurgical pain: risk factors and prevention. Lancet 2006; 367: 1618-25.
3.
Rzymski P, Kubasik M, Gaca M, Opala T. Is the shear wave sonographic elastography correlated with pain after breast augmentation with silicone implants an indication of inflammatory activity? A preliminary report. Wideochir Inne Tech Maloinwazyjne 2011; 6: 217-25.
4.
Haas E, Christodoulou N, Secanho M, et al. Capsular contracture after breast augmentation: a systematic review and meta-analysis. Aesthet Surg J Open Forum 2025; 7: ojaf003.
5.
Jung E, Hösl V, von Fraunberg S, Jung F, Prantl L. Ultrasound elastography for the detection of capsular fibrosis in breast implants: First results. Clin Hemorheol Microcirc 2021; 77: 247-57.
6.
Hidalgo DA, Spector JA. Breast augmentation. Plast Reconstr Surg 2014; 133: 567e-83e.
7.
Pacik PT, Nelson CE, Werner C. Pain control in augmentation mammaplasty using indwelling catheters in 687 consecutive patients: data analysis. Aesthet Surg J 2008; 28: 631-41.
8.
Fillingim RB, King CD, Ribeiro-Dasilva MC, Rahim-Williams B, Riley JL. Sex, gender, and pain: a review of recent clinical and experimental findings. J Pain 2009; 10: 447-85.
9.
Nelson JA, Shamsunder MG, Vorstenbosch J, et al. Prepectoral and subpectoral tissue expander-based breast reconstruction: a propensity-matched analysis of 90-day clinical and health-related quality-of-life outcomes. Plast Reconstr Surg 2022; 149: 607e.
10.
Woodworth GE, Ivie RMJ, Nelson SM, Walker CM, Maniker RB. Perioperative breast analgesia: a qualitative review of anatomy and regional techniques. Reg Anesth Pain Med 2017; 42: 609-31.
11.
Vingan PS, Kim M, Boe LA, et al. One-year outcomes in prepectoral versus subpectoral alloplastic breast reconstruction. Plast Reconstr Surg 2025; 156: 631e.
12.
Myles PS, Myles DB, Galagher W, et al. Measuring acute postoperative pain using the visual analog scale: the minimal clinically important difference and patient acceptable symptom state. Br J Anaesth 2017; 118: 424-9.
13.
Okamoto A, Yamasaki M, Yokota I, et al. Classification of acute pain trajectory after breast cancer surgery identifies patients at risk for persistent pain: a prospective observational study. J Pain Res 2018; 11: 2197-206.
14.
Majumdar JR, Goodman P, Burke MB, Gilliland J, Jairath N. Distress, pain, and nausea on postoperative day one and fourteen in women recovering from breast conserving surgery: a repeated-measure study. Oncol Nurs Forum 2024; 51: 381-90.
15.
Rawal N, Gupta A, Helsing M, Grell K, Allvin R. Pain relief following breast augmentation surgery: a comparison between incisional patient-controlled regional analgesia and traditional oral analgesia. Eur J Anaesthesiol 2006; 23: 1010-7.
16.
Eryilmaz NC, Eryilmaz T. Pain levels following cosmetic breast surgery and an easy-to-use pain treatment algorithm for plastic surgeons. Aesth Plast Surg 2024; 48: 1-6.
17.
Alghadir AH, Anwer S, Iqbal A, Iqbal ZA. Test-retest reliability, validity, and minimum detectable change of visual analog, numerical rating, and verbal rating scales for measurement of osteoarthritic knee pain. J Pain Res 2018; 11: 851-6.
18.
Knop C, Oeser M, Bastian L, Lange U, Zdichavsky M, Blauth M. [Development and validation of the Visual Analogue Scale (VAS) Spine Score]. Unfallchirurg 2001; 104: 488-97.
19.
Boonstra AM, Schiphorst Preuper HR, Reneman MF, Posthumus JB, Stewart RE. Reliability and validity of the visual analogue scale for disability in patients with chronic musculoskeletal pain. Int J Rehabil Res 2008; 31: 165-9.
20.
Joos E, Peretz A, Beguin S, Famaey JP. Reliability and reproducibility of visual analogue scale and numeric rating scale for therapeutic evaluation of pain in rheumatic patients. J Rheumatol 1991; 18: 1269-70.
21.
Price DD, Bush FM, Long S, Harkins SW. A comparison of pain measurement characteristics of mechanical visual analogue and simple numerical rating scales. Pain 1994; 56: 217-26.
22.
Klukowska AM, Vandertop WP, Schröder ML, Staartjes VE. Calculation of the minimum clinically important difference (MCID) using different methodologies: case study and practical guide. Eur Spine J 2024; 33: 3388-400.
23.
Hartrick CT, Kovan JP, Shapiro S. The numeric rating scale for clinical pain measurement: a ratio measure? Pain Pract 2003; 3: 310-6.
24.
Nilsson H, Angerås U, Bock D, et al. Is preoperative physical activity related to post-surgery recovery? A cohort study of patients with breast cancer. BMJ Open 2016; 6: e007997.
25.
Lautenbacher S, Peters JH, Heesen M, Scheel J, Kunz M. Age changes in pain perception: A systematic-review and meta-analysis of age effects on pain and tolerance thresholds. Neurosci Biobehav Rev 2017; 75: 104-13.
26.
Hakim S, Jain A, Woolf CJ. Immune drivers of pain resolution and protection. Nat Immunol 2024; 25: 2200-8.
27.
Zhi Y, Zhang Y, Zhang Y, Zhang M, Kong Y. Age-associated changes in multimodal pain perception. Age Ageing 2024; 53: afae107.
28.
Kazankaya F, Ahsun Paker S, Demirel Bozkurt Ö. Breastfeeding after breast augmentation surgery: a scoping review. Florence Nightingale J Nurs 2024; 32: 99-109.
29.
Bompy L, Gerenton B, Cristofari S, et al. Impact on breastfeeding according to implant features in breast augmentation: a multicentric retrospective study. Ann Plast Surg 2019; 82: 11-4.
30.
Mao S, He J, Huang L, et al. A survey of breastfeeding among women with previous surgery for benign breast disease: a descriptive exploratory study. Int Breastfeed J 2024; 19: 41.
31.
Majumder S, Mishra S, Shinde N, et al. Divergent paths of mammary gland involution: unveiling the cellular dynamics in abruptly and gradually involuted mouse models. Breast Cancer Res 2025; 27: 1.
32.
Rzymski P, Skórzewska A, Opala T. Changes in ultrasound shear wave elastography properties of normal breast during menstrual cycle. Clin Exp Obstet Gynecol 2011; 38: 137-42.
33.
Akhtar N, Li W, Mironov A, Streuli CH. Rac1 controls both the secretory function of the mammary gland and its remodeling for successive gestations. Dev Cell 2016; 38: 522-35.
34.
Eiler Frydshou Bak E, Larsen A, Kongsmark Weltz T, et al. The prevalence and histological characteristics of the double capsule phenomenon in breast augmentation with implants. Aesthet Surg J 2025; 45: 34-43.
35.
Paczkowska K, Rzymski P, Kubasik M, Opala T. Sonoelastography in the evaluation of capsule formation after breast augmentation – preliminary results from a follow-up study. Arch Med Sci 2016; 12: 793-8.
36.
Lotter L, Zucal I, Brébant V, et al. Intraoperative 3D comparison of round and anatomical breast implants: dispelling a myth. J Clin Med 2021; 11: 149.
37.
Liu Y, Zhang X, Luan J. Breast morphological comparison between anatomic and round implant augmentation: a prospective study. Ann Plast Surg 2023; 90: 19-26.
38.
Heimburg T. The effect of stretching on nerve excitability. Hum Mov Sci 2022; 86: 103000.
39.
Kanda H, Noguchi K, Dai Y. Axonal membrane stretch suppresses neuronal excitability by activating mechanosensitive K2P channels at the node of Ranvier. Mol Brain 2023; 16: 8.
40.
Urits I, Lavin C, Patel M, et al. Chronic pain following cosmetic breast surgery: a comprehensive review. Pain Ther 2020; 9: 71-82.
41.
Liang Z, Xu Y. The efficacy of pectoral nerve block for pain control after breast augmentation: a meta-analysis of randomized controlled studies. Medicine (Baltimore) 2023; 102: e32863.
42.
Frieden TR, Houry D. Reducing the risks of relief – the CDC’s opioid-prescribing guideline. N Engl J Med 2016; 374: 1501-4.
43.
Cho J, Kim KH, Lee W, Go JY, Kim SH. Effectiveness of a novel temperature-responsive hydrogel (PF72) for postoperative pain relief in breast augmentation. J Clin Med 2023; 13: 110.
44.
Xia Z, Chen Y, Xie J, et al. Faster return to daily activities and better pain control: a prospective study of enhanced recovery after surgery protocol in breast augmentation. Aesth Plast Surg 2023; 47: 2261-7.
45.
Hart AM, Broecker JS, Kao L, Losken A. Opioid use following outpatient breast surgery: are physicians part of the problem? Plast Reconstr Surg 2018; 142: 611-20.
46.
Braden JB, Young A, Sullivan MD, Walitt B, Lacroix AZ, Martin L. Predictors of change in pain and physical functioning among post-menopausal women with recurrent pain conditions in the women’s health initiative observational cohort. J Pain 2012; 13: 64-72.
47.
Hina N, Fletcher D, Poindessous-Jazat F, Martinez V. Hyperalgesia induced by low-dose opioid treatment before orthopaedic surgery: an observational case-control study. Eur J Anaesthesiol 2015; 32: 255-61.
48.
Torabi R, Bourn L, Mundinger GS, et al. American Society of plastic surgeons member post-operative opioid prescribing patterns. Plast Reconstr Surg 2019; 7: e2125.
49.
Klifto KM, Elhelali A, Payne RM, Cooney CM, Manahan MA, Rosson GD. Perioperative systemic nonsteroidal anti-inflammatory drugs (NSAIDs) in women undergoing breast surgery. Cochrane Database Syst Rev 2021; 11: CD013290.
50.
Von Sperlingl ML, Høimyrl H, Finnerupl K, Jensenl TS, Finnerupl NB. Persistent pain and sensory changes following cosmetic breast augmentation. Eur J Pain 2011; 15: 328-32.
51.
Oh KS, Hwang C, Lee H-Y, et al. Preclinical studies of ropivacaine extended-release from a temperature responsive hydrogel for prolonged relief of pain at the surgical wound. Int J Pharm 2019; 558: 225-30.
52.
Qiu SS, Roque M, Chen Y-C. The role of local bupivacaine irrigation in postoperative pain control after augmentation mammoplasty: a systematic review and meta-analysis. Plast Surg (Oakv) 2017; 25: 32-9.
53.
Hidalgo DA, Pusic AL. The role of methocarbamol and intercostal nerve blocks for pain management in breast augmentation. Aesthet Surg J 2005; 25: 571-5.
54.
Kennedy GT, Hill CM, Huang Y, et al. Enhanced recovery after surgery (ERAS) protocol reduces perioperative narcotic requirement and length of stay in patients undergoing mastectomy with implant-based reconstruction. Am J Surg 2020; 220: 147-52.
55.
Temple-Oberle C, Shea-Budgell MA, Tan M, et al. Consensus review of optimal perioperative care in breast reconstruction: enhanced recovery after surgery (ERAS) society recommendations. Plast Reconstr Surg 2017; 139: 1056e.
56.
Mui J, Cheng E, Salindera S. Enhanced recovery after surgery for oncological breast surgery reduces length of stay in a resource limited setting. ANZ J Surg 2024; 94: 1096-101.
57.
Estler A, Zanderigo E, Wessling D, et al. Quantification of breast volume according to age and BMI: a three-dimensional MRI analysis of 400 women. Aesth Plast Surg 2023; 47: 1713-24.
58.
Mateja KL, Long AS, Hauc SC, et al. An online calculator for estimating breast implant volume from imaging. Plast Reconstr Surg Glob Open 2022; 10: e4273.
59.
Basile FV, Oliveira TS. Using machine learning to select breast implant volume. Plast Reconstr Surg 2024; 154: 470e-7e.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.