Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
PULMONOLOGY / CLINICAL RESEARCH
Simvastatin reduces growth differentiation factor-15 in patients with chronic obstructive pulmonary disease
1
Center for Transplantology and Interstitial Lung Diseases, Jagiellonian University Medical College, Krakow, Poland
2
Department of Pulmonology, St. John Paul II Hospital, Krakow, Poland
3
Faculty of Health Sciences, Andrzej Frycz Modrzewski Krakow University, Krakow, Poland
4
Doctoral School of Medical and Health Sciences, Jagiellonian University Medical College, Krakow, Poland
5
Department of Thromboembolic Disorders, Institute of Cardiology, Jagiellonian University Medical College, Krakow, Poland
6
Krakow Center for Medical Research and Technologies, St. John Paul II Hospital, Krakow, Poland
Submission date: 2025-11-26
Final revision date: 2026-02-25
Acceptance date: 2026-03-20
Online publication date: 2026-04-17
Publication date: 2026-04-30
Corresponding author
Michał Ząbczyk
Department of Thromboembolic Disorders Institute of Cardiology Jagiellonian University Medical College 80 Pradnicka St 31-202 Krakow, Poland Phone: +48126142108 Fax: +48126142120
Department of Thromboembolic Disorders Institute of Cardiology Jagiellonian University Medical College 80 Pradnicka St 31-202 Krakow, Poland Phone: +48126142108 Fax: +48126142120
Arch Med Sci 2026;22(2):848-856
KEYWORDS
chronic obstructive pulmonary diseasegrowth differentiation factor-15statinplasminogen activator inhibitor type 1
TOPICS
ABSTRACT
Introduction:
In patients with chronic obstructive pulmonary disease (COPD), statins may improve lung function and reduce exacerbations. In COPD, growth differentiation factor-15 (GDF-15) has been shown to correlate with increasing age, current smoking, and greater comorbidity, and to predict disease outcomes; however, the effect of statins on GDF-15 is not known.
Material and methods:
This study was designed as a post-hoc analysis of GDF-15 levels in serum samples obtained from 54 patients with COPD (49 men; 90.7%), who had a 1-second forced expiratory volume (FEV1) to forced vital capacity (FVC) ratio < 0.7. Patients assigned (1 : 1) to receive simvastatin (40 mg/day) or to remain without such treatment were followed for 3 months. Lung function and laboratory parameters, including C-reactive protein, tumor necrosis factor-a (TNF-a), interleukin-6, and plasminogen activator inhibitor type 1 (PAI-1), were also assessed.
Results:
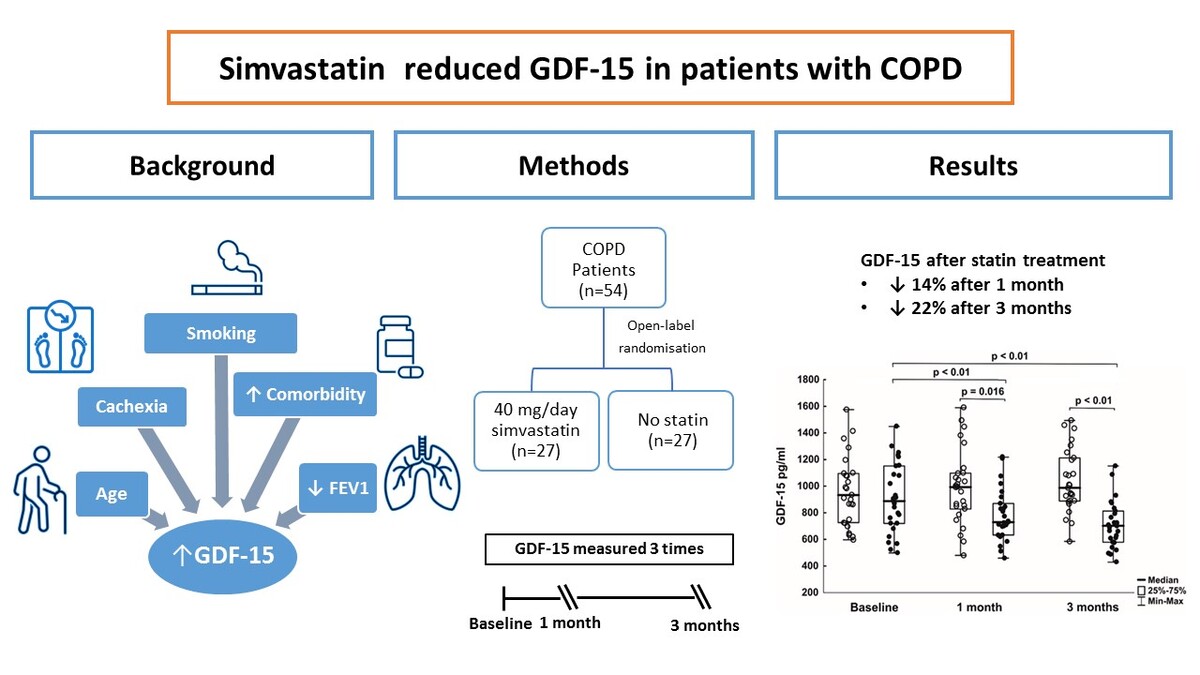
Baseline GDF-15 concentrations (median: 907.5 pg/ml, interquartile range: 720–1095 pg/ml) correlated negatively with FEV1 (r = –0.38, p < 0.01) and positively with age (r = 0.32, p = 0.017), TNF-a (r = 0.31, p = 0.031), and PAI-1 (r = 0.40, p < 0.01), but not with lipid profile or other variables. Simvastatin reduced GDF-15 by 23% at 3 months compared to baseline (p < 0.01), independently of changes in lipid variables or inflammatory markers. At both 1 and 3 months, GDF-15 levels in the statin-treated group were 14% and 22% lower compared to the untreated control group (both p < 0.05).
Conclusions:
Our study suggests that statin treatment can reduce circulating GDF-15 levels associated with COPD severity, which may be an additional benefit of such treatment beyond lipid-lowering or anti-inflammatory effects.
In patients with chronic obstructive pulmonary disease (COPD), statins may improve lung function and reduce exacerbations. In COPD, growth differentiation factor-15 (GDF-15) has been shown to correlate with increasing age, current smoking, and greater comorbidity, and to predict disease outcomes; however, the effect of statins on GDF-15 is not known.
Material and methods:
This study was designed as a post-hoc analysis of GDF-15 levels in serum samples obtained from 54 patients with COPD (49 men; 90.7%), who had a 1-second forced expiratory volume (FEV1) to forced vital capacity (FVC) ratio < 0.7. Patients assigned (1 : 1) to receive simvastatin (40 mg/day) or to remain without such treatment were followed for 3 months. Lung function and laboratory parameters, including C-reactive protein, tumor necrosis factor-a (TNF-a), interleukin-6, and plasminogen activator inhibitor type 1 (PAI-1), were also assessed.
Results:
Baseline GDF-15 concentrations (median: 907.5 pg/ml, interquartile range: 720–1095 pg/ml) correlated negatively with FEV1 (r = –0.38, p < 0.01) and positively with age (r = 0.32, p = 0.017), TNF-a (r = 0.31, p = 0.031), and PAI-1 (r = 0.40, p < 0.01), but not with lipid profile or other variables. Simvastatin reduced GDF-15 by 23% at 3 months compared to baseline (p < 0.01), independently of changes in lipid variables or inflammatory markers. At both 1 and 3 months, GDF-15 levels in the statin-treated group were 14% and 22% lower compared to the untreated control group (both p < 0.05).
Conclusions:
Our study suggests that statin treatment can reduce circulating GDF-15 levels associated with COPD severity, which may be an additional benefit of such treatment beyond lipid-lowering or anti-inflammatory effects.
REFERENCES (37)
1.
Halpin DMG. Mortality of patients with COPD. Expert Rev Respir Med 2024; 18: 381-95.
2.
Kruk A, Czerwińska C, Dolna-Michno J, Broniatowska E, Kolanko E. Effectiveness of a smoking cessation program during the COVID-19 pandemic. Healthcare (Basel) 2023; 11: 1536.
3.
Li CL, Liu SF. Exploring molecular mechanisms and biomarkers in COPD: an overview of current advancements and perspectives. Int J Mol Sci 2024; 25: 7347.
4.
Wan Y, Fu J. GDF15 as a key disease target and biomarker: linking chronic lung diseases and ageing. Mol Cell Biochem 2024; 479: 453-66.
5.
Wu Q, Jiang D, Matsuda JL, Ternyak K, Zhang B, Chu HW. Cigarette smoke induces human airway epithelial senescence via growth differentiation factor 15 production. Am J Respir Cell Mol Biol 2016; 55: 429-38.
6.
Wu Q, Jiang D, Schaefer NR, et al. Overproduction of growth differentiation factor 15 promotes human rhinovirus infection and virus-induced inflammation in the lung. Am J Physiol Lung Cell Mol Physiol 2018; 314: L514-27.
7.
Lv Z, Liang G, Cheng M. Predictive value of GDF-15 and sST2 for pulmonary hypertension in acute exacerbation of chronic obstructive pulmonary disease. Int J Chron Obstruct Pulmon Dis 2023; 18: 2431-8.
8.
Husebø GR, Grønseth R, Lerner L, et al. Growth differentiation factor-15 is a predictor of important disease outcomes in patients with COPD. Eur Respir J 2017; 49: 1601298.
9.
Sivapalan P, Ackermann DA, Vognsen AK, et al. Plasma growth differentiation factor-15 is associated with cardiovascular events in patients hospitalized for acute exacerbation of COPD. Sci Rep 2026; 16: 898.
10.
Takahashi S, Nakamura H, Seki M, et al. Reversal of elastase-induced pulmonary emphysema and promotion of alveolar epithelial cell proliferation by simvastatin in mice. Am J Physiol Lung Cell Mol Physiol 2008; 294: L882-90.
11.
Ajmera M, Shen C, Sambamoorthi U. Association between statin medications and COPD-specific outcomes: a real-world observational study. Drugs Real World Outcomes 2017; 4: 9-19.
12.
Baigent C, Keech A, Kearney PM, et al. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet 2005; 366: 1267-78.
13.
Keddissi JI, Younis WG, Chbeir EA, Daher NN, Dernaika TA, Kinasewitz GT. The use of statins and lung function in current and former smokers. Chest 2007; 132: 1764-71.
14.
Lee T, Lin M, Chang N. Usefulness of C-reactive protein and interleukin-6 as predictors of outcomes in patients with chronic obstructive pulmonary disease receiving pravastatin. Am J Cardiol 2008; 101: 530-5.
15.
Blamoun AI, Batty GN, DeBari VA, Rashid AO, Sheikh M, Khan MA. Statins may reduce episodes of exacerbation and the requirement for intubation in patients with COPD: evidence from a retrospective cohort study. Int J Clin Pract 2008; 62: 1373-8.
16.
Wang MT, Lo YW, Tsai CL, et al. Statin use and risk of COPD exacerbation requiring hospitalization. Am J Med 2013; 126: 598-606.e2.
17.
Frost FJ, Petersen H, Tollestrup K, Skipper B. Influenza and COPD mortality protection as pleiotropic, dose-dependent effects of statins. Chest 2007; 131: 1006-12.
18.
Tentzeris I, Farhan S, Freynhofer MK, et al. Usefulness of elevated levels of growth differentiation factor-15 to classify patients with acute coronary syndrome having percutaneous coronary intervention who would benefit from high-dose statin therapy. Am J Cardiol 2017; 120: 747-52.
19.
Bonaca MP, Morrow DA, Braunwald E, et al. Growth differentiation factor-15 and risk of recurrent events in patients stabilized after acute coronary syndrome: observations from PROVE IT-TIMI 22. Arterioscler Thromb Vasc Biol 2011; 31: 203-10.
20.
Kim JM, Back MK, Yi HS, Joung KH, Kim HJ, Ku BJ. Effect of atorvastatin on growth differentiation factor-15 in patients with type 2 diabetes mellitus and dyslipidemia. Diabetes Metab J 2016; 40: 70-8.
21.
Rabe KF, Hurd S, Anzueto A, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med 2007; 176: 532-55.
22.
Undas A, Kaczmarek P, Sladek K, et al. Fibrin clot properties are altered in patients with chronic obstructive pulmonary disease: beneficial effects of simvastatin treatment. Thromb Haemost 2009; 102: 1176-82.
23.
Kruk A, Ząbczyk M, Natorska J, Undas A. Statin treatment reduces protein carbonylation in patients with COPD: a randomized controlled study. Eur J Clin Invest 2025; 55: e70009.
24.
R Core Team. R: A language and environment for statistical computing [computer program]. Vienna (Austria): R Foundation for Statistical Computing; 2021. Available from: https://www.R-project.org/.
25.
Devulder JV. Unveiling mechanisms of lung aging in COPD: a promising target for therapeutics development. Chin Med J Pulm Crit Care Med 2024; 2: 133-41.
26.
Mueller T, Leitner I, Egger M, Haltmayer M, Dieplinger B. Association of the biomarkers soluble ST2, galectin-3 and growth differentiation factor-15 with heart failure and other non-cardiac diseases. Clin Chim Acta 2015; 445: 155-60.
27.
Tang Y, Liu T, Sun S, et al. Role and mechanism of growth differentiation factor 15 in chronic kidney disease J Inflamm Res 2024; 17: 2861-71.
28.
Reyes J, Yap GS. Emerging roles of growth differentiation factor 15 in immunoregulation and pathogenesis. J Immunol 2023; 210: 5-11.
29.
Bootcov M, Bauskin A, Valenzuela S, et al. MIC-1, a novel macrophage inhibitory cytokine, is a divergent member of the TGF-beta superfamily. Proc Natl Acad Sci USA 1997; 94: 11514-9.
30.
Schenk P, Spiel AO, Hüttinger F, et al. Can simvastatin reduce COPD exacerbations? A randomised double-blind controlled study. Eur Respir J 2021; 58: 2001798.
31.
Nopp S, Moik F, Kraler S, et al. Growth differentiation factor-15 and prediction of cancer-associated thrombosis and mortality: a prospective cohort study. J Thromb Haemost 2023; 21: 2461-72.
32.
Abe M, Harpel JG, Metz CN, Nunes I, Loskutoff DJ, Rifkin DB. An assay for transforming growth factor-b using cells transfected with a plasminogen activator inhibitor-1 promoter-luciferase construct. Anal Biochem 1994; 216: 276-84.
33.
Li YL, Chang JT, Lee LY, et al. GDF15 contributes to radioresistance and cancer stemness of head and neck cancer by regulating cellular reactive oxygen species via a SMAD-associated signaling pathway. Oncotarget 2017; 8: 1508-28.
34.
Mach F, Baigent C, Catapano AL, et al.; ESC Scientific Document Group. 2019 ESC/EAS guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk. Eur Heart J 2020; 41: 111-88.
35.
Solnica B, Sygitowicz G, Sitkiewicz D, et al. 2024 Guidelines of the Polish Society of Laboratory Diagnostics and the Polish Lipid Association on laboratory diagnostics of lipid metabolism disorders. Arch Med Sci 2024; 20: 357-74.
36.
Banach M, Fronczek M, Osadnik T, et al. Risk of adverse cardiovascular events based on common genetic variants in 8-year follow-up of the LIPIDOGEN2015 population using the polygenic risk score (PRS): study design and methodology. Arch Med Sci 2024; 20: 1452-60.
37.
Dąbrowiecki P, Chciałowski A, Dąbrowiecka A, Piórkowska A, Badyda A. Air pollution and long-term risk of hospital admission due to chronic obstructive pulmonary disease exacerbations in Poland: a time-stratified, case-crossover study. Pol Arch Intern Med 2023; 133: 16444.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.