Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
CLINICAL RESEARCH
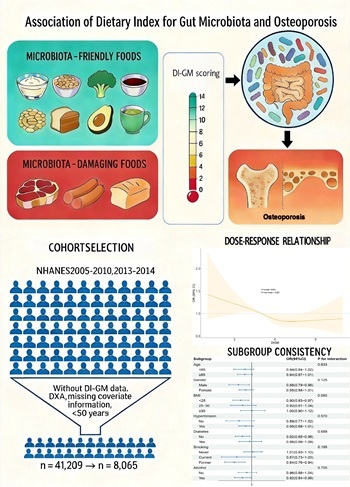
Association between the Dietary Index for Gut Microbiota and osteoporosis: a cross-sectional study from NHANES among individuals aged ≥ 50 years
1
Department of Basic Medicine, Qiannan Medical College for Nationalities, Duyun, China
2
Center for Tissue Engineering and Stem Cell Research, Guizhou Medical University, Guiyang, China
3
Department of Gastroenterology, Affiliated Hospital of Guizhou Medical University, Guiyang, China
4
Department of Medical Ultrasonics, The People’s Hospital of Qiannan, Qiannan, China
These authors had equal contribution to this work
Submission date: 2025-10-18
Final revision date: 2025-12-15
Acceptance date: 2025-12-22
Online publication date: 2026-04-10
Corresponding author
KEYWORDS
TOPICS
ABSTRACT
Introduction:
The gut microbiota serves as a critical interface between the host’s internal environment and external factors, influencing bone mass and quality by modulating immune homeostasis, mineral absorption, and the production of systemically active metabolites. In this context, the Dietary Index for Gut Microbiota (DI-GM) provides a valuable metric for quantifying diet quality in relation to microbiota health. Therefore, investigating the association between DI-GM and the risk of osteoporosis (OP) is important for developing evi-dence-based dietary prevention guidelines.
Material and methods:
This cross-sectional study leveraged data from the U.S. National Health and Nutrition Examination Survey (NHANES) in 2005–2010 and 2013–2014. Multivariable weighted logistic regression (WLR) models were employed to ascertain the association between DI-GM and the prevalence of OP. Restricted cubic splines (RCS) were leveraged to explore the dose-response relationship between DI-GM and OP. Subgroup analyses and interaction tests were performed to validate the reliability of the findings.
Results:
Our analysis included 8,065 U.S. adults aged ≥ 50 years. The multivariable WLR analysis revealed that the risk of OP significantly decreased with increasing DI-GM scores (OR = 0.929, 95% CI: 0.874–0.988, p = 0.021). Relative to the cohort with the lowest DI-GM scores, the highest DI-GM cohort exhibited a 36.1% lower risk of OP (OR = 0.639, 95% CI: 0.441–0.925, p = 0.019). RCS analysis indi-cated a negative linear correlation between DI-GM and OP (p non-linear = 0.281).
Conclusions:
Higher DI-GM scores were associated with lower risk of OP, indicating a protective role for diets that enhance GM diver-sity.
The gut microbiota serves as a critical interface between the host’s internal environment and external factors, influencing bone mass and quality by modulating immune homeostasis, mineral absorption, and the production of systemically active metabolites. In this context, the Dietary Index for Gut Microbiota (DI-GM) provides a valuable metric for quantifying diet quality in relation to microbiota health. Therefore, investigating the association between DI-GM and the risk of osteoporosis (OP) is important for developing evi-dence-based dietary prevention guidelines.
Material and methods:
This cross-sectional study leveraged data from the U.S. National Health and Nutrition Examination Survey (NHANES) in 2005–2010 and 2013–2014. Multivariable weighted logistic regression (WLR) models were employed to ascertain the association between DI-GM and the prevalence of OP. Restricted cubic splines (RCS) were leveraged to explore the dose-response relationship between DI-GM and OP. Subgroup analyses and interaction tests were performed to validate the reliability of the findings.
Results:
Our analysis included 8,065 U.S. adults aged ≥ 50 years. The multivariable WLR analysis revealed that the risk of OP significantly decreased with increasing DI-GM scores (OR = 0.929, 95% CI: 0.874–0.988, p = 0.021). Relative to the cohort with the lowest DI-GM scores, the highest DI-GM cohort exhibited a 36.1% lower risk of OP (OR = 0.639, 95% CI: 0.441–0.925, p = 0.019). RCS analysis indi-cated a negative linear correlation between DI-GM and OP (p non-linear = 0.281).
Conclusions:
Higher DI-GM scores were associated with lower risk of OP, indicating a protective role for diets that enhance GM diver-sity.
REFERENCES (26)
2.
Händel MN, Cardoso I, von Bülow C, et al. Fracture risk reduction and safety by osteoporosis treatment compared with placebo or active comparator in postmenopausal women: systematic review, network meta-analysis, and meta-regression analysis of randomised clinical trials. BMJ 2023; 381: e068033.
3.
Wright NC, Looker AC, Saag KG, et al. The recent prevalence of osteoporosis and low bone mass in the United States based on bone mineral density at the femoral neck or lumbar spine. J Bone Miner Res 2014; 29: 2520-6.
4.
LeBoff MS, Greenspan SL, Insogna KL, et al. The clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 2022; 33: 2049-102.
5.
Behera J, Ison J, Tyagi SC, Tyagi N. The role of gut microbiota in bone homeostasis. Bone 2020; 135: 115317.
6.
Hathaway-Schrader JD, Steinkamp HM, Chavez MB, et al. Antibiotic perturbation of gut microbiota dysregulates osteoimmune cross talk in postpubertal skeletal development. Am J Pathol 2019; 189: 370-390.
7.
Ross FC, Patangia D, Grimaud G, et al. The interplay between diet and the gut microbiome: implications for health and disease. Nat Rev Mi-crobiol 2024; 22: 671-86.
8.
Kase BE, Liese AD, Zhang J, Murphy EA, Zhao L, Steck SE. The development and evaluation of a literature-based Dietary Index for Gut Mi-crobiota. Nutrients 2024; 16: 1045-65.
9.
Johnson CL, Paulose-Ram R, Ogden CL, et al. National health and nutrition examination survey: analytic guidelines, 1999-2010. Vital Health Stat 2 2013; (161): 1-24.
10.
An S, Qin J, Gong X, et al. The mediating role of body mass index in the association between Dietary Index for Gut Microbiota and biological age: a study based on NHANES 2007-2018. Nutrients 2024; 16: 4164-79.
11.
Bress AP, Anderson TS, Flack JM, et al. The management of elevated blood pressure in the acute care setting: a scientific statement from the american heart association. Hypertension 2024; 81: e94-106.
12.
Xu F, Earp JE, Adami A, Weidauer L, Greene GW. The relationship of physical activity and dietary quality and diabetes prevalence in US adults: findings from NHANES 2011-2018. Nutrients 2022; 14: 3324-35.
13.
Karlamangla AS, Burnett-Bowie SM, Crandall CJ. Bone health during the menopause transition and beyond. Obstet Gynecol Clin North Am 2018; 45: 695-708.
14.
Yang C, Ren J, Li B, et al. Identification of gene biomarkers in patients with postmenopausal osteoporosis. Mol Med Rep 2019; 19: 1065-73.
15.
Wang M, Wang X, Cui W, et al. The association between hemoglobin level and osteoporosis in a Chinese population with environmental lead and cadmium exposure. Environ Geochem Health 2022; 44: 1673-82.
16.
Perna S, Avanzato I, Nichetti M, D’Antona G, Negro M, Rondanelli M. Association between Dietary Patterns of Meat and Fish Consumption with Bone Mineral Density or Fracture Risk: a systematic literature. Nutrients 2017; 9: 1029-49.
17.
Fan L, Xia Y, Wang Y, et al. Gut microbiota bridges dietary nutrients and host immunity. Sci China Life Sci 2023; 66: 2466-514.
18.
Zheng Y, Cheng S, Li H, et al. Lacticaseibacillus paracasei JM053 alleviates osteoporosis in rats by increasing the content of soy isoflavone aglycones in fermented soymilk. Food Funct 2024; 15: 12118-33.
19.
Ijaz MU, Ahmed MI, Zou X, et al. Beef, casein, and soy proteins differentially affect lipid metabolism, triglycerides accumulation and gut mi-crobiota of high-fat diet-fed C57BL/6J mice. Front Microbiol 2018; 9: 2200.
20.
Ghadiri M, Soltani M, Rajabzadeh-Dehkordi M, et al. The relation between dietary quality and healthy eating index with bone mineral densi-ty in osteoporosis: a case-control study. BMC Musculoskelet Disord 2023; 24: 584.
21.
Thomas RL, Jiang L, Adams JS, et al. Vitamin D metabolites and the gut microbiome in older men. Nat Commun 2020; 11: 5997.
22.
de Vos WM, Tilg H, Van Hul M, Cani PD. Gut microbiome and health: mechanistic insights. Gut 2022; 71: 1020-32.
23.
Zaky A, Glastras SJ, Wong MYW, Pollock CA, Saad S. The role of the gut microbiome in diabetes and obesity-related kidney disease. Int J Mol Sci 2021; 22: 9641-67.
24.
Yang Z, Wang Q, Liu Y, et al. Gut microbiota and hypertension: association, mechanisms and treatment. Clin Exp Hypertens 2023; 45: 2195135.
25.
Montagnani A, Gonnelli S, Alessandri M, Nuti R. Osteoporosis and risk of fracture in patients with diabetes: an update. Aging Clin Exp Res 2011; 23: 84-90.
26.
Xu R, Lian D, Xie Y, et al. Relationship between serum uric acid levels and osteoporosis. Endocr Connect 2023; 12: e230040.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.