Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
CARDIOLOGY / CLINICAL RESEARCH
Sleep duration may not have any effect on the risk of stroke: insights from Mendelian randomization and prospective cohort studies
1
Clinical Trial Service Unit, Nuffield Department of Population Health, University of Oxford, UK
2
Department of Nutritional Sciences and Dietetics, International Hellenic University, Thessaloniki, Greece
3
School of Medicine, European University Cyprus, Nicosia, Cyprus
4
Faculty of Science, Liverpool Hope University, United Kingdom
5
Institute of Life Course and Medical Sciences, University of Liverpool, Liverpool, United Kingdom
6
Department of Clinical Medicine, Aalborg University, Aalborg, Denmark
7
Department of Cardiology, Lipidology and Internal Medicine with Intensive Coronary Care Unit, Medical University of Bialystok, Poland
8
Institute of Cardiovascular and Medical Sciences, University of Glasgow, United Kingdom
9
Department of Preventive Cardiology and Lipidology, Medical University of Lodz (MUL), Poland
10
Polish Mother’s Memorial Hospital Research Institute (PMMHRI), Lodz, Poland
Submission date: 2021-11-09
Final revision date: 2021-11-26
Acceptance date: 2021-11-27
Online publication date: 2021-11-27
Publication date: 2026-04-30
Corresponding author
Maciej Banach
Department of Preventive Cardiology and Lipidology Medical University of Lodz (MUL), Lodz Polish Mother’s Memorial Hospital Research Institute (PMMHRI) Lodz Poland
Department of Preventive Cardiology and Lipidology Medical University of Lodz (MUL), Lodz Polish Mother’s Memorial Hospital Research Institute (PMMHRI) Lodz Poland
Arch Med Sci 2026;22(2):721-734
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Due to contentious associations between sleep and stroke risk, we performed a meta-analysis of cohort studies and Mendelian randomization (MR) analysis.
Material and methods:
For the meta-analysis, we pooled prospective studies and reviewed the largest genome-wide association studies investigating self-reported or accelerometer-derived sleep duration in relation to stroke subtype: ischemic (IS), cardioembolic (CES), large artery (LAS), or small vessel (SVS). The inverse-variance weighted method (IVW), weighted median (WM)-based method, MR-Egger and MR-Pleiotropy RESidual Sum and Outlier (PRESSO) were performed. To determine the impact of single nucleotide polymorphisms (SNPs), the leave-one-out method was applied.
Results:
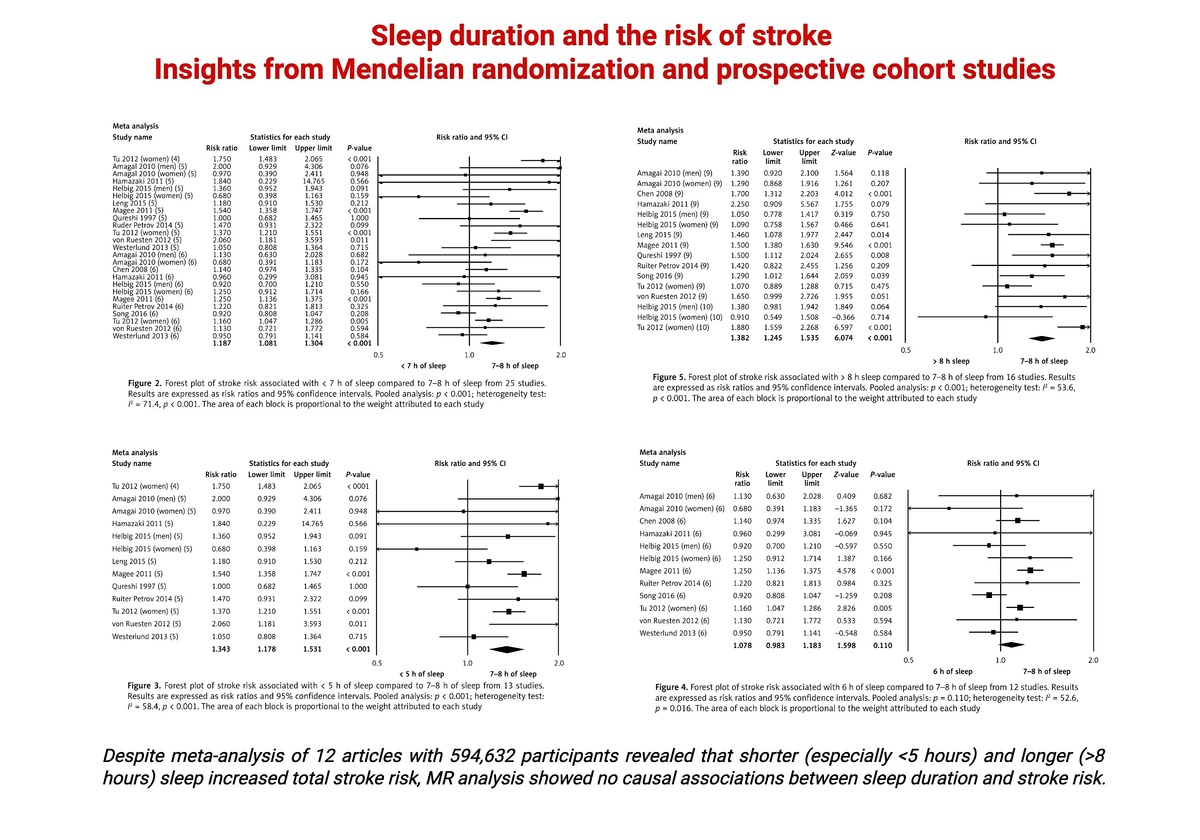
Pooled prospective studies demonstrated that both shorter (< 7 h) [n = 25 studies, I2 = 71.4, p < 0.001; risk ratio (RR) = 1.18, 95% CI: 1.08–1.30, p < 0.001] and longer (> 8 h) [n = 16 studies, I2 = 53.6, p < 0.001; RR = 1.38, 95% CI: 1.24–1.53, p < 0.001] sleep increased stroke risk (compared with 7–8 h), but were subject to high levels of heterogeneity. In MR, self-reported sleep duration had no significant effect on IS (IVW: beta = –0.031, p = 0.747), CES (IVW: beta = –0.039, p = 0.849), LAS (IVW: beta = –0.246, p = 0.328) or SVS (IVW: beta = –0.102, p = 0.667) risk. This was also observed for short and long accelerometer-derived sleep (all p > 0.126). Estimated associations had no significant heterogeneity, and MR-PRESSO revealed no outliers. There was low likelihood of pleiotropy (all estimations p > 0.539), and associations were not driven by single SNPs.
Conclusions:
Meta-analysis revealed that shorter and longer sleep increased total stroke risk, but with high heterogeneity. MR analysis showed no causal associations between sleep duration and stroke risk.
Due to contentious associations between sleep and stroke risk, we performed a meta-analysis of cohort studies and Mendelian randomization (MR) analysis.
Material and methods:
For the meta-analysis, we pooled prospective studies and reviewed the largest genome-wide association studies investigating self-reported or accelerometer-derived sleep duration in relation to stroke subtype: ischemic (IS), cardioembolic (CES), large artery (LAS), or small vessel (SVS). The inverse-variance weighted method (IVW), weighted median (WM)-based method, MR-Egger and MR-Pleiotropy RESidual Sum and Outlier (PRESSO) were performed. To determine the impact of single nucleotide polymorphisms (SNPs), the leave-one-out method was applied.
Results:
Pooled prospective studies demonstrated that both shorter (< 7 h) [n = 25 studies, I2 = 71.4, p < 0.001; risk ratio (RR) = 1.18, 95% CI: 1.08–1.30, p < 0.001] and longer (> 8 h) [n = 16 studies, I2 = 53.6, p < 0.001; RR = 1.38, 95% CI: 1.24–1.53, p < 0.001] sleep increased stroke risk (compared with 7–8 h), but were subject to high levels of heterogeneity. In MR, self-reported sleep duration had no significant effect on IS (IVW: beta = –0.031, p = 0.747), CES (IVW: beta = –0.039, p = 0.849), LAS (IVW: beta = –0.246, p = 0.328) or SVS (IVW: beta = –0.102, p = 0.667) risk. This was also observed for short and long accelerometer-derived sleep (all p > 0.126). Estimated associations had no significant heterogeneity, and MR-PRESSO revealed no outliers. There was low likelihood of pleiotropy (all estimations p > 0.539), and associations were not driven by single SNPs.
Conclusions:
Meta-analysis revealed that shorter and longer sleep increased total stroke risk, but with high heterogeneity. MR analysis showed no causal associations between sleep duration and stroke risk.
REFERENCES (65)
1.
Guidelines for medical treatment for stroke prevention. American College of Physicians. Ann Intern Med 1994; 121: 54-5.
2.
Kwok CS, Kontopantelis E, Kuligowski G, et al. Self-reported sleep duration and quality and cardiovascular disease and mortality: a dose-response meta-analysis. J Am Heart Assoc 2018; 7: e008552.
3.
Kripke DF, Garfinkel L, Wingard DL, Klauber MR, Marler MR. Mortality associated with sleep duration and insomnia. Arch General Psychiatry 2002; 59: 131-6.
4.
Ferrie JE, Shipley MJ, Cappuccio FP, et al. A prospective study of change in sleep duration: associations with mortality in the Whitehall II cohort. Sleep 2007; 30: 1659-66.
5.
Ayas NT, White DP, Manson JE, et al. A prospective study of sleep duration and coronary heart disease in women. Arch Internal Med 2003; 163: 205-9.
6.
Ayas NT, White DP, Al-Delaimy WK, et al. A prospective study of self-reported sleep duration and incident diabetes in women. Diabetes Care 2003; 26: 380-4.
7.
Cappuccio FP, Stranges S, Kandala NB, et al. Gender-specific associations of short sleep duration with prevalent and incident hypertension: the Whitehall II Study. Hypertension. 2007; 50: 693-700.
8.
Gangwisch JE, Heymsfield SB, Boden-Albala B, et al. Short sleep duration as a risk factor for hypertension: analyses of the first National Health and Nutrition Examination Survey. Hypertension 2006; 47: 833-9.
9.
Mazidi M, Shekoohi N, Katsiki N, Banach M. Longer sleep duration may negatively affect renal function. Int Urol Nephrol 2021; 53: 325-32.
10.
Cappuccio FP, Taggart FM, Kandala NB, et al. Meta-analysis of short sleep duration and obesity in children and adults. Sleep 2008; 31: 619-26.
11.
Cappuccio FP, D’Elia L, Strazzullo P, Miller MA. Sleep duration and all-cause mortality: a systematic review and meta-analysis of prospective studies. Sleep 2010; 33: 585-92.
12.
Cappuccio FP, Cooper D, D’elia L, Strazzullo P, Miller MA. Sleep duration predicts cardiovascular outcomes: a systematic review and meta-analysis of prospective studies. Eur Heart J 2011; 32: 1484-92.
13.
Jike M, Itani O, Watanabe N, Buysse DJ, Kaneita Y. Long sleep duration and health outcomes: a systematic review, meta-analysis and meta-regression. Sleep Med Rev 2018; 39: 25-36.
14.
Itani O, Jike M, Watanabe N, Kaneita Y. Short sleep duration and health outcomes: a systematic review, meta-analysis, and meta-regression. Sleep Med 2017; 32: 246-56.
15.
Meisinger C, Heier M, Löwel H, Schneider A, Döring A. Sleep duration and sleep complaints and risk of myocardial infarction in middle-aged men and women from the general population: the MONICA/KORA Augsburg cohort study. Sleep 2007; 30: 1121-7.
16.
Qureshi AI, Giles WH, Croft JB, Bliwise DL. Habitual sleep patterns and risk for stroke and coronary heart disease: a 10-year follow-up from NHANES I. Neurology 1997; 48: 904-10.
17.
Daghlas I, Dashti HS, Lane J, et al. Sleep duration and myocardial infarction. J Am Coll Cardiol 2019; 74: 1304-14.
18.
Ikehara S, Iso H, Date C, et al. Association of sleep duration with mortality from cardiovascular disease and other causes for Japanese men and women: the JACC study. Sleep 2009; 32: 295-301.
19.
Chen JC, Brunner RL, Ren H, et al. Sleep duration and risk of ischemic stroke in postmenopausal women. Stroke 2008; 39: 3185.
20.
Hamazaki Y, Morikawa Y, Nakamura K, et al. The effects of sleep duration on the incidence of cardiovascular events among middle-aged male workers in Japan. Scand J Work Environ Health 2011; 37: 411-7.
21.
Davies NM, Holmes MV, Davey Smith G. Reading Mendelian randomisation studies: a guide, glossary, and checklist for clinicians. BMJ 2018; 362: k601.
22.
Smith GD, Ebrahim S. ‘Mendelian randomization’: can genetic epidemiology contribute to understanding environmental determinants of disease? Int J Epidemiol 2003; 32: 1-22.
23.
Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 2000; 283: 2008-12.
24.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 2010; 25: 603-5.
25.
Ferretti G, Bacchetti T, Sahebkar A. Effect of statin therapy on paraoxonase-1 status: a systematic review and meta-analysis of 25 clinical trials. Progress Lipid Res 2015; 60: 50-73.
26.
Sahebkar A. Are curcuminoids effective C-reactive protein-lowering agents in clinical practice? Evidence from a meta-analysis. Phytother Res 2014; 28: 633-42.
27.
Sahebkar A, Serban MC, Mikhailidis DP, et al. Head-to-head comparison of statins versus fibrates in reducing plasma fibrinogen concentrations: a systematic review and meta-analysis. Pharmacol Res 2016; 103: 236-52.
28.
Duval S, Tweedie R. Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 2000; 56: 455-63.
29.
Borenstein M, Hedges L, Higgins J, Rothstein H. Comprehensive Metaanalysis (Vers. 2). Englewood Cliffs, NJ: Biostat. Inc; 2005.
30.
Bycroft C, Freeman C, Petkova D, et al. The UK Biobank resource with deep phenotyping and genomic data. Nature 2018; 562: 203-9.
31.
Dashti HS, Jones SE, Wood AR, et al. Genome-wide association study identifies genetic loci for self-reported habitual sleep duration supported by accelerometer-derived estimates. Nature Commun 2019; 10: 1100.
32.
Jones SE, van Hees VT, Mazzotti DR, et al. Genetic studies of accelerometer-based sleep measures yield new insights into human sleep behaviour. Nature Commun 2019; 10: 1585.
33.
Malik R, Chauhan G, Traylor M, et al. Multiancestry genome-wide association study of 520,000 subjects identifies 32 loci associated with stroke and stroke subtypes. Nat Genet 2018; 50: 524-37.
34.
Adams HP, Jr., Bendixen BH, Kappelle LJ, et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 1993; 24: 35-41.
35.
Bowden J, Davey Smith G, Haycock PC, Burgess S. Consistent estimation in mendelian randomization with some invalid instruments using a weighted median estimator. Genet Epidemiol 2016; 40: 304-14.
36.
Bowden J, Davey Smith G, Burgess S. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol 2015; 44: 512-25.
37.
Burgess S, Bowden J, Fall T, Ingelsson E, Thompson SG. Sensitivity analyses for robust causal inference from mendelian randomization analyses with multiple genetic variants. Epidemiology 2017; 28: 30-42.
38.
Bowden J, Del Greco MF, Minelli C, Davey Smith G, Sheehan N, Thompson J. A framework for the investigation of pleiotropy in two-sample summary data Mendelian randomization. Stat Med 2017; 36: 1783-802.
39.
Verbanck M, Chen CY, Neale B, Do R. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat Genet 2018; 50: 693-8.
40.
Song Q, Liu X, Zhou W, et al. Long sleep duration and risk of ischemic stroke and hemorrhagic stroke: the Kailuan Prospective Study. Sci Rep 2016; 6: 33664.
41.
Petrov MER, Letter AJ, Howard VJ, Kleindorfer D. Self-reported sleep duration in relation to incident stroke symptoms: nuances by body mass and race from the REGARDS study. J Stroke Cerebrovasc Dis 2014; 23: e123-e32.
42.
Leng Y, Cappuccio FP, Wainwright NW, et al. Sleep duration and risk of fatal and nonfatal stroke: a prospective study and meta-analysis. Neurology 2015; 84: 1072-9.
43.
Amagai Y, Ishikawa S, Gotoh T, Kayaba K, Nakamura Y, Kajii E. Sleep duration and incidence of cardiovascular events in a Japanese population: the Jichi Medical School cohort study. J Epidemiol 2010; 20: 106-10.
44.
Helbig AK, Stöckl D, Heier M, Ladwig KH, Meisinger C. Symptoms of insomnia and sleep duration and their association with incident strokes: findings from the population-based MONICA/KORA Augsburg Cohort Study. PLoS One 2015; 10: e0134480.
45.
Von Ruesten A, Weikert C, Fietze I, Boeing H. Association of sleep duration with chronic diseases in the European Prospective Investigation into Cancer and Nutrition (EPIC)-Potsdam study. PLoS One 2012; 7: e30972.
46.
Magee CA, Kritharides L, Attia J, McElduff P, Banks E. Short and long sleep duration are associated with prevalent cardiovascular disease in Australian adults. J Sleep Res 2012; 21: 441-7.
47.
Tu X, Cai H, Gao YT, et al. Sleep duration and its correlates in middle-aged and elderly Chinese women: the Shanghai Women’s Health Study. Sleep Med 2012; 13: 1138-45.
48.
Westerlund A, Bellocco R, Sundström J, Adami HO, Åkerstedt T, Lagerros YT. Sleep characteristics and cardiovascular events in a large Swedish cohort. Eur J Epidemiol 2013; 28: 463-73.
49.
Meng L, Zheng Y, Hui R. The relationship of sleep duration and insomnia to risk of hypertension incidence: a meta-analysis of prospective cohort studies. Hypertens Res 2013; 36: 985.
50.
Palomäki H, Berg A, Meririnne E, et al. Complaints of poststroke insomnia and its treatment with mianserin. Cerebrovasc Dis 2003; 15: 56-62.
51.
Stone KL, Ewing SK, Ancoli-Israel S, et al. Self-reported sleep and nap habits and risk of mortality in a large cohort of older women. J Am Geriatr Soc 2009; 57: 604-11.
52.
Cappuccio FP, D’Elia L, Strazzullo P, Miller MA. Quantity and quality of sleep and incidence of type 2 diabetes: a systematic review and meta-analysis. Diabetes Care 2010; 33: 414-20.
53.
Spiegal K, Tasali E, Penev P, Van Cauter E. Sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels and increased hunger and appetite. Ann Int Med 2004; 141: 846-50.
54.
Tsubono Y, Fukao A, Hisamichi S. Health practices and mortality in a rural Japanese population. Tohoku J Exp Med 1993; 171: 339-48.
55.
Copinschi G. Metabolic and endocrine effects of sleep deprivation. Essent Psychopharmacol 2005; 6: 341-7.
56.
Nakajima H, Kaneita Y, Yokoyama E, et al. Association between sleep duration and hemoglobin A1c level. Sleep Med 2008; 9: 745-52.
57.
Bjorvatn B, Sagen IM, Øyane N, et al. The association between sleep duration, body mass index and metabolic measures in the Hordaland Health Study. J Sleep Res 2007; 16: 66-76.
58.
Duss SB, Seiler A, Schmidt MH, et al. The role of sleep in recovery following ischemic stroke: a review of human and animal data. Neurobiol Sleep Circadian Rhythms 2017; 2: 94-105.
59.
Banach M, Toth PP, Bielecka-Dąbrowa A, Lewek J. Primary and secondary cardiovascular prevention: recent advances. Kardiol Pol 2024; 82: 1200-10.
60.
Banach M, Fogacci F, Atanasov AG, et al.; International Lipid Expert Panel (ILEP). A 360° perspective on cardiovascular prevention: the International Lipid Expert Panel SiMple tIps for the heaLthy hEart (ILEP-SMILE). Arch Med Sci 2025; 21: 711-8.
61.
Stranges S, Dorn JM, Shipley MJ, et al. Correlates of short and long sleep duration: a cross-cultural comparison between the United Kingdom and the United States: the Whitehall II Study and the Western New York Health Study. Am J Epidemiol 2008; 168: 1353-64.
62.
Krueger PM, Friedman EM. Sleep duration in the United States: a cross-sectional population-based study. Am J Epidemiol 2009; 169: 1052-63.
63.
Patel SR, Malhotra A, Gottlieb DJ, White DP, Hu FB. Correlates of long sleep duration. Sleep 2006; 29: 881-9.
64.
Sterr A, Kuhn M, Nissen C, et al. Post-stroke insomnia in community-dwelling patients with chronic motor stroke: physiological evidence and implications for stroke care. Sci Rep 2018; 8: 8409.
65.
Wu MP, Lin HJ, Weng SF, Ho CH, Wang JJ, Hsu YW. Insomnia subtypes and the subsequent risks of stroke: report from a nationally representative cohort. Stroke 2014; 45: 1349-54.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.