Current issue
Archive
Manuscripts accepted
About the Journal
Editorial office
Editorial board
Section Editors
Abstracting and indexing
Subscription
Contact
Ethical standards and procedures
Most read articles
Instructions for authors
Article Processing Charge (APC)
Regulations of paying article processing charge (APC)
HEPATOLOGY / CLINICAL RESEARCH
Assessing hepatosteatosis in endogenous Cushing’s syndrome: the hepatic steatosis index as a reliable diagnostic tool
1
Endocrinology and Metabolism, Ankara City Hospital, Ankara, Turkey
2
Endocrinology and Metabolism, Faculty of Medicine, Ankara Yildirim Beyazit University, Ankara, Turkey
Submission date: 2025-01-06
Final revision date: 2025-04-13
Acceptance date: 2025-04-19
Online publication date: 2025-06-08
Publication date: 2026-04-30
Corresponding author
Arch Med Sci 2026;22(2):796-803
KEYWORDS
hepatosteatosisCushing’s syndromenon-alcoholic fatty liver diseasemetabolic dysfunction-associated steatotic liver disease
TOPICS
ABSTRACT
Introduction:
Non-alcoholic fatty liver disease, now termed metabolic dysfunction-associated steatotic liver disease (MASLD), represents a significant health burden worldwide. Patients with Cushing’s syndrome (CS), a condition characterized by excessive cortisol production, may be at an elevated risk for MASLD due to associated metabolic disturbances.
Material and methods:
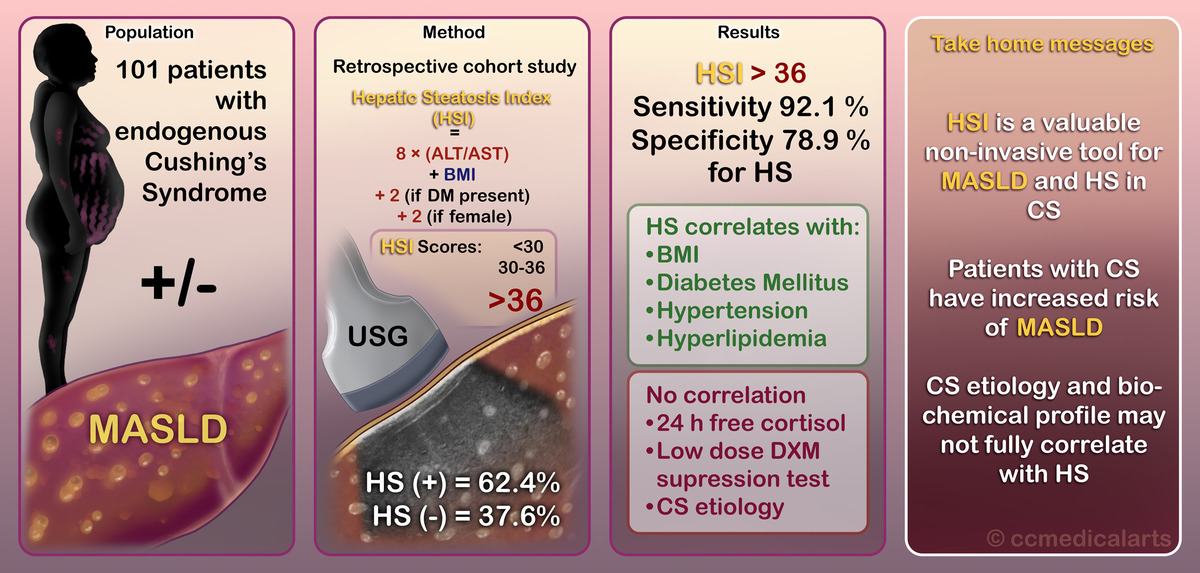
This study aimed to evaluate the predictive value of the hepatic steatosis index (HSI) in diagnosing MASLD in patients with CS. 101 endogenous CS patients were included, and hepatosteatosis was assessed using ultrasonography. HSI scores were calculated, and associations with clinical and biochemical parameters were analyzed.
Results:
Hepatosteatosis was observed in 62.4% of CS patients, with all these individuals meeting the criteria for MASLD. The HSI demonstrated hepatosteatosis with high sensitivity (92.1%) and specificity (78.9%) compared to ultrasonography. Factors significantly correlated with hepatosteatosis included higher body mass index, diabetes, hypertension, and hyperlipidemia. There was no correlation with basal morning cortisol, 24-hour urinary free cortisol, low-dose dexamethasone suppression tests, or the etiology of CS.
Conclusions:
Our study represents a pioneering effort to explore MASLD in patients with endogenous CS by evaluating the HSI as a diagnostic tool. Using the HSI, we demonstrated high sensitivity and specificity in diagnosing hepatosteatosis, emphasizing its potential as a valuable non-invasive tool in this population. Furthermore, our study fills a significant gap in the literature by being the first to investigate the predictive power of HSI for MASLD diagnosis, specifically in CS patients. Integrating these findings into clinical practice could enhance the early detection and management of MASLD in endogenous CS, ultimately improving patient outcomes.
Non-alcoholic fatty liver disease, now termed metabolic dysfunction-associated steatotic liver disease (MASLD), represents a significant health burden worldwide. Patients with Cushing’s syndrome (CS), a condition characterized by excessive cortisol production, may be at an elevated risk for MASLD due to associated metabolic disturbances.
Material and methods:
This study aimed to evaluate the predictive value of the hepatic steatosis index (HSI) in diagnosing MASLD in patients with CS. 101 endogenous CS patients were included, and hepatosteatosis was assessed using ultrasonography. HSI scores were calculated, and associations with clinical and biochemical parameters were analyzed.
Results:
Hepatosteatosis was observed in 62.4% of CS patients, with all these individuals meeting the criteria for MASLD. The HSI demonstrated hepatosteatosis with high sensitivity (92.1%) and specificity (78.9%) compared to ultrasonography. Factors significantly correlated with hepatosteatosis included higher body mass index, diabetes, hypertension, and hyperlipidemia. There was no correlation with basal morning cortisol, 24-hour urinary free cortisol, low-dose dexamethasone suppression tests, or the etiology of CS.
Conclusions:
Our study represents a pioneering effort to explore MASLD in patients with endogenous CS by evaluating the HSI as a diagnostic tool. Using the HSI, we demonstrated high sensitivity and specificity in diagnosing hepatosteatosis, emphasizing its potential as a valuable non-invasive tool in this population. Furthermore, our study fills a significant gap in the literature by being the first to investigate the predictive power of HSI for MASLD diagnosis, specifically in CS patients. Integrating these findings into clinical practice could enhance the early detection and management of MASLD in endogenous CS, ultimately improving patient outcomes.
REFERENCES (27)
1.
Mitrovic B, Gluvic Z, Obradovic MM, et al. Non-alcoholic fatty liver disease, metabolic syndrome, and type 2 diabetes mellitus: where do we stand today? Arch Med Sci 2023; 19: 884-94.
2.
Ahmed A, Wong RJ, Harrison SA. Nonalcoholic fatty liver disease review: diagnosis, treatment, and outcomes. Clin Gastroenterol Hepatol 2015; 13: 2062-70.
3.
Leung C, Yeoh SW, Patrick D, et al. Characteristics of hepatocellular carcinoma in cirrhotic and non-cirrhotic non-alcoholic fatty liver disease. World J Gastroenterol 2015; 21: 1189-96.
4.
Mohamad B, Shah V, Onyshchenko M, et al. Characterization of hepatocellular carcinoma (HCC) in non-alcoholic fatty liver disease (NAFLD) patients without cirrhosis. Hepatol Int 2016; 10: 632-9.
5.
Chan WK, Chuah KH, Rajaram RB, Lim LL, Ratnasingam J, Vethakkan SR. Metabolic dysfunction-associated steatotic liver disease (MASLD): a state-of-the-art review. J Obes Metab Syndr 2023; 32: 197-213.
6.
Hazlehurst JM, Gathercole LL, Nasiri M, et al. Glucocorticoids fail to cause insulin resistance in human subcutaneous adipose tissue in vivo. J Clin Endocrinol Metab 2013; 98: 1631-40.
7.
Baid SK, Rubino D, Sinaii N, Ramsey S, Frank A, Nieman LK. Specificity of screening tests for Cushing’s syndrome in an overweight and obese population. J Clin Endocrinol Metab 2009; 94: 3857-64.
8.
Matthew Morris E, Fletcher JA, Thyfault JP, Rector RS. The role of angiotensin II in nonalcoholic steatohepatitis. Mol Cell Endocrinol 2013; 378: 29-40.
9.
European Association for the Study of the Liver (EASL); European Association for the Study of Diabetes (EASD); European Association for the Study of Obesity (EASO). EASL-EASD-EASO Clinical Practice Guidelines on the Management of Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD). Obes Facts 2024; 17: 374-444.
10.
Hernaez R, Lazo M, Bonekamp S, et al. Diagnostic accuracy and reliability of ultrasonography for the detection of fatty liver: a meta-analysis. Hepatology 2011; 54: 1082-90.
11.
Petzold G. Role of ultrasound methods for the assessment of NAFLD. J Clin Med 2022; 11: 4581.
12.
Tarantino G, Finelli C. Pathogenesis of hepatic steatosis: the link between hypercortisolism and non-alcoholic fatty liver disease. World J Gastroenterol 2013; 19: 6735-43.
13.
Ferraioli G, Soares Monteiro LB. Ultrasound-based techniques for the diagnosis of liver steatosis. World J Gastroenterol 2019; 25: 6053-62.
14.
Kim D, Manikat R, Cholankeril G, Ahmed A. Endogenous sex hormones and nonalcoholic fatty liver disease in US adults. Liver Int 2024; 44: 460-71.
15.
Wu Z, Ouyang T, Liu H, Cao L, Chen W. Perfluoroalkyl substance (PFAS) exposure and risk of nonalcoholic fatty liver disease in the elderly: results from NHANES 2003-2014. Environ Sci Pollut Res Int 2023; 30: 64342-51.
16.
Gür-Altunay D, Yürük-Atasoy P. How successful are APRI and FIB-4 scores in predicting liver fibrosis in chronic hepatitis B patients? Infect Dis Clin Microbiol 2023; 5: 332-40.
17.
The Modification of Diet in Renal Disease Study: design, methods, and results from the feasibility study. Am J Kidney Dis 1992; 20: 18-33.
18.
Lei F, Qin JJ, Song X, et al. The prevalence of MAFLD and its association with atrial fibrillation in a nationwide health check-up population in China. Front Endocrinol 2022; 13: 1007171.
19.
Lim GEH, Tang A, Ng CH, et al. An observational data meta-analysis on the differences in prevalence and risk factors between MAFLD vs NAFLD. Clin Gastroenterol Hepatol 2023; 21: 619-29.e7.
20.
Rockall AG, Sohaib SA, Evans D, et al. Hepatic steatosis in Cushing’s syndrome: a radiological assessment using computed tomography. Eur J Endocrinol 2003; 149: 543-8.
21.
Zhou J, Zhang M, Bai X, et al. Demographic characteristics, etiology, and comorbidities of patients with Cushing’s syndrome: a 10-year retrospective study at a large general hospital in China. Int J Endocrinol 2019; 2019: 7159696.
22.
Marengo M, Briet C, Munier M, Boursier J, Rodien P, Suteau V. Fatty liver disease along Cushing’s syndrome evolution. J Clin Endocrinol Metab 2025; 110: e2037-44.
23.
Auer MK, Stalla GK, Stieg MR. Investigating the role of cortisol and growth hormone in fatty liver development: fatty liver index in patients with pituitary adenomas. Pituitary 2016; 19: 461-71.
24.
Matsumoto T, Yamasaki S, Arakawa A, et al. Exposure to a high total dosage of glucocorticoids produces non-alcoholic steatohepatits. Pathol Int 2007; 57: 388-9.
25.
Itoh S, Igarashi M, Tsukada Y, Ichinoe A. Nonalcoholic fatty liver with alcoholic hyalin after long-term glucocorticoid therapy. Acta Hepatogastroenterol 1977; 24: 415-8.
26.
Barrera F, Uribe J, Olvares N, Huerta P, Cabrera D, Romero-Gómez M. The Janus of a disease: diabetes and metabolic dysfunction-associated fatty liver disease. Ann Hepatol 2024; 29: doi: 10.1016/j.aohep.2024.101501.
27.
Targher G, Bertolini L, Rodella S, Zoppini G, Zenari L, Falezza G. Associations between liver histology and cortisol secretion in subjects with nonalcoholic fatty liver disease. Clin Endocrinol 2006; 64: 337-41.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.